Page 57 - JSOM Winter 2025
P. 57
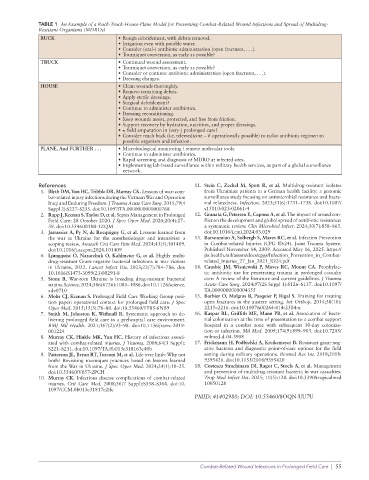
TABLE 1 An Example of a Ruck-Truck-House-Plane Model for Preventing Combat-Related Wound Infections and Spread of Multidrug-
Resistant Organisms (MDROs)
RUCK • Rough debridement, with debris removal.
• Irrigation even with potable water.
• Consider (oral-) antibiotic administration (open fractures, . . .).
• Tourniquet conversion, as early as possible?
TRUCK • Continued wound assessment.
• Tourniquet conversion, as early as possible?
• Consider or continue antibiotic administration (open fractures, . . .).
• Dressing changes.
HOUSE • Clean wounds thoroughly.
• Remove remaining debris.
• Apply sterile dressings.
• Surgical debridement?
• Continue to administer antibiotics.
• Dressing reconditioning.
• Keep wounds moist, protected, and free from friction.
• Support recovery by hydration, nutrition, and proper dressings.
• ± field amputation in (very-) prolonged care?
• Consider reach back (i.e. telemedicine – if operationally possible) to tailor antibiotic regimen to
possible organism and infection.
PLANE, And FURTHER . . . • Microbiological monitoring / remote molecular tools.
• Continue to administer antibiotics.
• Rapid screening and diagnosis of MDRO at infected sites.
• Implementing lab-based surveillance within military health services, as part of a global surveillance
network.
References 11. Stein C, Zechel M, Spott R, et al. Multidrug-resistant isolates
1. Blyth DM, Yun HC, Tribble DR, Murray CK. Lessons of war: com- from Ukrainian patients in a German health facility: a genomic
bat-related injury infections during the Vietnam War and Operation surveillance study focusing on antimicrobial resistance and bacte-
Iraqi and Enduring Freedom. J Trauma Acute Care Surg. 2015;79(4 rial relatedness. Infection. 2023;51(6):1731–1738. doi:10.1007/
Suppl 2):S227–S235. doi:10.1097/TA.0000000000000768 s15010-023-02061-4
2. Rapp J, Keenan S, Taylor D, et al. Sepsis Management in Prolonged 12. Granata G, Petersen E, Capone A, et al. The impact of armed con-
Field Care: 28 October 2020. J Spec Oper Med. 2020;20(4):27– flict on the development and global spread of antibiotic resistance:
39. doi:10.55460/I18B-1ZQM a systematic review. Clin Microbiol Infect. 2024;30(7):858–865.
3. Jarrassier A, Py N, de Rocquigny G, et al. Lessons learned from doi:10.1016/j.cmi.2024.03.029
the war in Ukraine for the anesthesiologist and intensivist: a 13. Barsoumian A, Solbergb S, Maves RC, et al. Infection Prevention
scoping review. Anaesth Crit Care Pain Med. 2024;43(5):101409. in Combat-related Injuries (CPG ID:24). Joint Trauma System.
doi:10.1016/j.accpm.2024.101409 Published November 14, 2009. Accessed May 16, 2025. https://
4. Ljungquist O, Nazarchuk O, Kahlmeter G, et al. Highly multi- jts.health.mil/assets/docs/cpgs/Infection_Prevention_in_Combat-
drug-resistant Gram-negative bacterial infections in war victims related_Injuries_27_Jan_2021_ID24.pdf
in Ukraine, 2022. Lancet Infect Dis. 2023;23(7):784–786. doi: 14. Causbie JM, Wisniewski P, Maves RC, Mount CA. Prophylac-
10.1016/S1473-3099(23)00291-8 tic antibiotic use for penetrating trauma in prolonged casualty
5. Stone R. War-torn Ukraine is breeding drug-resistant bacterial care: A review of the literature and current guidelines. J Trauma
strains. Science. 2024;386(6726):1085–1086. doi:10.1126/science. Acute Care Surg. 2024;97(2S Suppl 1):S126–S137. doi:10.1097/
adv0710 TA.0000000000004355
6. Mohr CJ, Keenan S. Prolonged Field Care Working Group posi- 15. Barbier O, Malgras B, Pasquier P, Rigal S. Training for treating
tion paper: operational context for prolonged field care. J Spec open fractures in the austere setting. Int Orthop. 2014;38(10):
Oper Med. 2015;15(3):78–80. doi:10.55460/1T85-6NB9 2215–2216. doi:10.1007/s00264-014-2504-x
7. Smith M, Johnston K, Withnall R. Systematic approach to de- 16. Kaspar RL, Griffith ME, Mann PB, et al. Association of bacte-
livering prolonged field care in a prehospital care environment. rial colonization at the time of presentation to a combat support
BMJ Mil Health. 2021;167(2):93–98. doi:10.1136/jramc-2019- hospital in a combat zone with subsequent 30-day coloniza-
001224 tion or infection. Mil Med. 2009;174(9):899–903. doi:10.7205/
8. Murray CK, Hinkle MK, Yun HC. History of infections associ- milmed-d-04-3908
ated with combat-related injuries. J Trauma. 2008;64(3 Suppl): 17. Frickmann H, Podbielski A, Kreikemeyer B. Resistant gram-neg-
S221–S231. doi:10.1097/TA.0b013e318163c40b ative bacteria and diagnostic point-of-care options for the field
9. Patterson JL, Bryan RT, Turconi M, et al. Life over limb: Why not setting during military operations. Biomed Res Int. 2018;2018:
both? Revisiting tourniquet practices based on lessons learned 9395420. doi:10.1155/2018/9395420
from the War in Ukraine. J Spec Oper Med. 2024;24(1):18–25. 18. Costescu Strachinaru DI, Ragot C, Stoefs A, et al. Management
doi:10.55460/V057-2PCH and prevention of multidrug-resistant bacteria in war casualties.
10. Murray CK. Infectious disease complications of combat-related Trop Med Infect Dis. 2025; 10(5):128. doi:10.3390/tropicalmed
injuries. Crit Care Med. 2008;36(7 Suppl):S358–S364. doi:10. 10050128
1097/CCM.0b013e31817e2ffc
PMID: 41402980; DOI: 10.55460/8OQN-UU7U
Combat-Related Wound Infections in Prolonged Field Care | 55