Page 14 - 2023 SMOG Digital
P. 14
Trauma
ABDOMINAL INJURY
Signs and Symptoms
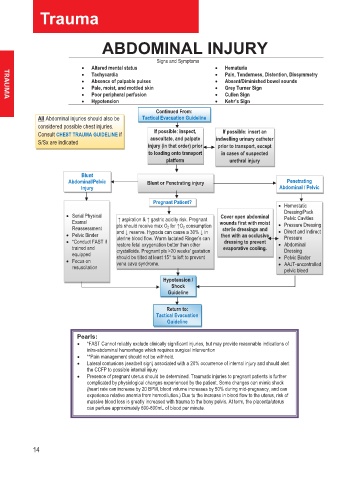
• Altered mental status • Hematuria
• Tachycardia • Pain, Tenderness, Distention, Dissymmetry
• Absence of palpable pulses • Absent/Diminished bowel sounds
• Pale, moist, and mottled skin • Grey Turner Sign
• Poor peripheral perfusion • Cullen Sign
• Hypotension • Kehr’s Sign
Continued From:
All Abdominal injuries should also be Tactical Evacuation Guideline
considered possible chest injuries.
Consult CHEST TRAUMA GUIDELINE if If possible: inspect, If possible: insert an
S/Sx are indicated auscultate, and palpate indwelling urinary catheter
injury (in that order) prior prior to transport, except
to loading onto transport in cases of suspected
platform urethral injury
Blunt
Abdominal/Pelvic Blunt or Penetrating injury Penetrating
Injury Abdominal / Pelvic
Pregnant Patient?
• Hemostatic
• Serial Physical Cover open abdominal Dressing/Pack
Pelvic Cavities
Exams/ ↑ aspiration & ↑ gastric acidity risk. Pregnant wounds first with moist
Reassessment pts should receive max O 2 for ↑O 2 consumption sterile dressings and • Pressure Dressing
• Pelvic Binder and ↓ reserve. Hypoxia can cause a 30% ↓ in then with an occlusive • Direct and Indirect
Pressure
uterine blood flow. Warm lactated Ringer’s can
• *Conduct FAST if restore fetal oxygenation better than other dressing to prevent • Abdominal
trained and crystalloids. Pregnant pts >20 weeks’ gestation evaporative cooling. Dressing
equipped should be tilted at least 15° to left to prevent • Pelvic Binder
• Focus on vena cava syndrome. • AAJT-uncontrolled
resuscitation pelvic bleed
Hypotension /
Shock
Guideline
Return to:
Tactical Evacuation
Guideline
Pearls:
• *FAST Cannot reliably exclude clinically significant injuries, but may provide reasonable indications of
intra-abdominal hemorrhage which requires surgical intervention
• **Pain management should not be withheld.
• Lateral contusions (seatbelt sign) associated with a 20% occurrence of internal injury and should alert
the CCFP to possible internal injury
• Presence of pregnant uterus should be determined. Traumatic injuries to pregnant patients is further
complicated by physiological changes experienced by the patient. Some changes can mimic shock
(heart rate can increase by 20 BPM, blood volume increases by 50% during mid-pregnancy, and can
experience relative anemia from hemodilution.) Due to the increase in blood flow to the uterus, risk of
massive blood loss is greatly increased with trauma to the bony pelvis. At term, the placenta/uterus
can perfuse approximately 600-800mL of blood per minute.
14