Page 30 - JSOM Winter 2021
P. 30
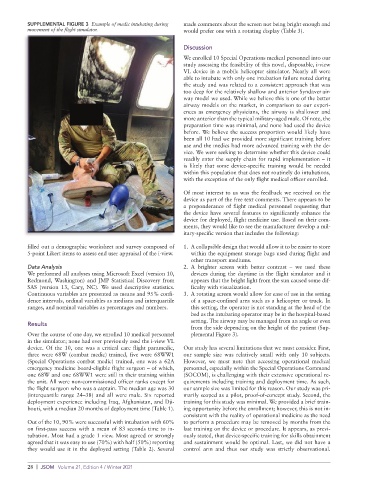
SUPPLEMENTAL FIGURE 3 Example of medic intubating during made comments about the screen not being bright enough and
movement of the flight simulator. would prefer one with a rotating display (Table 3).
Discussion
We enrolled 10 Special Operations medical personnel into our
study assessing the feasibility of this novel, disposable, i-view
VL device in a mobile helicopter simulator. Nearly all were
able to intubate with only one intubation failure noted during
the study and was related to a consistent approach that was
too deep for the relatively shallow and anterior Syndaver air-
way model we used. While we believe this is one of the better
airway models on the market, in comparison to our experi-
ences as emergency physicians, the airway is shallower and
more anterior than the typical military-aged male. Of note, the
preparation time was minimal, and none had used the device
before. We believe the success proportion would likely have
been all 10 had we provided more significant training before
use and the medics had more advanced training with the de-
vice. We were seeking to determine whether this device could
readily enter the supply chain for rapid implementation – it
is likely that some device-specific training would be needed
within this population that does not routinely do intubations,
with the exception of the only flight medical officer enrolled.
Of most interest to us was the feedback we received on the
device as part of the free text comments. There appears to be
a preponderance of flight medical personnel requesting that
the device have several features to significantly enhance the
device for deployed, flight medicine use. Based on their com-
ments, they would like to see the manufacturer develop a mil-
itary-specific version that includes the following:
filled out a demographic worksheet and survey composed of 1. A collapsible design that would allow it to be easier to store
5-point Likert items to assess end user appraisal of the i-view. within the equipment storage bags used during flight and
other transport mediums.
Data Analysis 2. A brighter screen with better contrast – we used these
We performed all analyses using Microsoft Excel (version 10, devices during the daytime in the flight simulator and it
Redmond, Washington) and JMP Statistical Discovery from appears that the bright light from the sun caused some dif-
SAS (version 13, Cary, NC). We used descriptive statistics. ficulty with visualization.
Continuous variables are presented as means and 95% confi- 3. A rotating screen would allow for ease of use in the setting
dence intervals, ordinal variables as medians and interquartile of a space-confined area such as a helicopter or truck. In
ranges, and nominal variables as percentages and numbers. this setting, the operator is not standing at the head of the
bed as the intubating operator may be in the hospital-based
setting. The airway may be managed from an angle or even
Results
from the side depending on the height of the patient (Sup-
Over the course of one day, we enrolled 10 medical personnel plemental Figure 3).
in the simulator; none had ever previously used the i-view VL
device. Of the 10, one was a critical care flight paramedic, Our study has several limitations that we must consider. First,
three were 68W (combat medic) trained, five were 68WW1 our sample size was relatively small with only 10 subjects.
(Special Operations combat medic) trained, one was a 62A However, we must note that accessing operational medical
emergency medicine board-eligible flight surgeon – of which, personnel, especially within the Special Operations Command
one 68W and one 68WW1 were still in their training within (SOCOM), is challenging with their extensive operational re-
the unit. All were non-commissioned officer ranks except for quirements including training and deployment time. As such,
the flight surgeon who was a captain. The median age was 30 our sample size was limited for this reason. Our study was pri-
(interquartile range 24–38) and all were male. Six reported marily scoped as a pilot, proof-of-concept study. Second, the
deployment experience including Iraq, Afghanistan, and Dji- training for this study was minimal. We provided a brief train-
bouti, with a median 20 months of deployment time (Table 1). ing opportunity before the enrollment; however, this is not in-
consistent with the reality of operational medicine as the need
Out of the 10, 90% were successful with intubation with 60% to perform a procedure may be removed by months from the
on first-pass success with a mean of 83 seconds time to in- last training on the device or procedure. It appears, as previ-
tubation. Most had a grade 1 view. Most agreed or strongly ously stated, that device-specific training for skills obtainment
agreed that it was easy to use (70%) with half (50%) reporting and sustainment would be optimal. Last, we did not have a
they would use it in the deployed setting (Table 2). Several control arm and thus our study was strictly observational.
28 | JSOM Volume 21, Edition 4 / Winter 2021