Page 124 - JSOM Fall 2018
P. 124
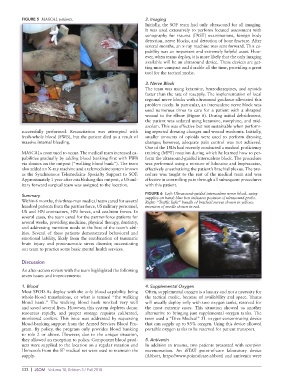
FIGURE 5 MASCAL patients. 2. Imaging
Initially, the SOF team had only ultrasound for all imaging.
It was used extensively to perform focused assessment with
sonography for trauma (FAST) examinations, foreign body
detection, nerve blocks, and detection of bone fracture. After
several months, an xray machine was sent forward. This ca
pability was an important and extremely helpful asset. How
ever, when teams deploy, it is more likely that the only imaging
available will be an ultrasound device. These devices are get
ting more compact and durable all the time, providing a great
tool for the tactical medic.
3. Nerve Block
The team was using ketamine, benzodiazepines, and opioids
faster than the rate of resupply. The implementation of local
regional nerve blocks with ultrasound guidance alleviated this
problem nicely. In particular, an interscalene nerve block was
used numerous times to care for a patient with a shrapnel
wound to the elbow (Figure 6). During initial debridement,
the patient was sedated using ketamine, morphine, and mid
azolam. This was effective but not sustainable when perform
successfully performed. Resuscitation was attempted with ing repeated dressing changes and wound washouts. Initially,
freshwhole blood (FWB), but the patient died as a result of smaller amounts of opioids were used to perform dressing
massive internal bleeding. changes; however, adequate pain control was not achieved.
One of the 18Ds had recently conducted a medical proficiency
MASCALs continued to occur. The medical team increased ca training (MPT) rotation during which he learned how to per
pabilities gradually by adding blood banking first with FWB form the ultrasoundguided interscalene block. The procedure
via donors on the outpost (“walking blood bank”). The team was performed using a mixture of lidocaine and bupivacaine,
also added an Xray machine and a telemedicine system known effectively anesthetizing the patient’s brachial plexus. The pro
as the Synchronous Telemedicine Specialty Support to SOF. cedure was taught to the rest of the medical team and was
Approximately 1 year after establishing this outpost, a US mil effective in controlling pain through all subsequent procedures
itary forward surgical team was assigned to the location. with this patient.
FIGURE 6 Left: Ultrasound-guided interscalene nerve block, using
Summary supplies on hand; blue box indicates position of ultrasound probe.
Within 6 months, this threeman medical team cared for several Right: “Traffic light” bundle of brachial nerves shown in yellow;
hundred patients from the partner force, US military personnel, insertion of needle shown in red.
US and HN contractors, HN forces, and coalition forces. In
several cases, the team cared for the partnerforce patients for
several weeks, providing medicine, physical therapy, dentistry,
and addressing nutrition needs to the best of the team’s abil
ities. Several of these patients demonstrated behavioral and
emotional lability, likely from the combination of traumatic
brain injury and posttraumatic stress disorder, necessitating
our team to practice some basic mental health services.
Discussion
An afteraction review with the team highlighted the following
seven issues and improvements:
1. Blood 4. Supplemental Oxygen
Most SFODAs deploy with the only blood capability being Often, supplemental oxygen is a luxury and not a necessity for
wholeblood transfusions, or what is termed “the walking the tactical medic, because of availability and space. Teams
blood bank.” The walking blood bank worked very well will usually deploy only with two oxygen tanks, reserved for
and saved several lives. However, this system depletes donor the most extreme cases. This situation showed us another
resources rapidly, and proper storage requires calibrated, alternative to bringing just supplemental oxygen tanks. The
monitored coolers. This issue was addressed by requesting team used a “Dive Medical” 5L oxygenconcentrating device
bloodbanking support from the Armed Services Blood Pro that can supply up to 93% oxygen. Using this device allowed
gram. By policy, the program only provides blood banking portable oxygen tanks to be reserved for patient transport.
to role 2 or above. However, due to the unique situation,
they allowed an exception to policy. Component blood prod 5. Antivenin
ucts were supplied to the location on a regular rotation and In addition to trauma, two patients presented with scorpion
Hemcools from the SF medical set were used to maintain the envenomation. An iSTAT pointofcare laboratory device
supply. (Abbott, https://www.pointofcare.abbott) and antivenin were
122 | JSOM Volume 18, Edition 3 / Fall 2018