Page 133 - JSOM Spring 2020
P. 133
simplicity and convenience this continuum can be conceptual- with increased vascularity may not be painful and tendons
ized in three main stages as shown in Figure 3. The first stage without increased vascularity may be painful, but there is
32
is called reactive tendinopathy, which is an adaptive response generally a higher degree of pain in pathological tendons with
from an acute overload such as a sudden increase in activity. increased vascularity. 33
In this stage, tenocytes proliferate and increase their protein
production thickening the portion of the tendon under load Epidemiology
to better tolerate the stress. A 2- to 3-fold increase in collagen
formation can occur that peaks about 24 hours after activ- Incidence Rates of Achilles Tendinopathy in the Military
ity and remains elevated for 70 to 80 hours. The orderly ar- To determine the incidence rates of clinically diagnosed AT
rangement of collagen fibers is largely maintained. The second in the military population, the Defense Medical Epidemiol-
stage of the continuum of tendinopathy depicted in Figure 3 is ogy Database (DMED) was queried. AT was indicated in the
34
called tendon disrepair in which there is a marked increase in DMED with an International Classification of Diseases, 9th
tenocytes and protein production and collagen fibers separate Revision (ICD-9) code of 726.71 (Achilles tendinitis or bursi-
and become disorganized, largely in focal areas. There may be tis). (Although this article uses the term AT, the ICD-9 code-
an increase in vascularity and ingrowth of neurons. The third book still uses the term Achilles tendinitis.) Because rupture
stage is degenerative tendinopathy, in which there is cell death, of the Achilles tendon could also be indicative of an Achilles
large areas of the disorganization, and areas filled with vessels tendon pathology, ICD-9 code 727.67 (nontraumatic Achilles
and lacking collagen. The tendon appears to have little ability tendon rupture) was analyzed separately. The primary diagno-
to recover once it reaches this stage and if the pathology is sis and first occurrence of these codes were selected for analy-
widespread enough a rupture can occur. It is possible for some sis. Incidence for each year was calculated as: [new cases (n)/
sections of the tendon to be in different stages at the same military population (n) × 1000] to obtain the incidence rate as
time. 22,24,25 cases/1000 person-yr.
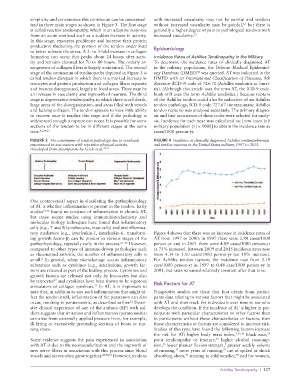
FIGURE 3 The continuum of tendon pathology due to overloads FIGURE 4 Incidence of clinically diagnosed Achilles tendinitis/bursitis
experienced in association with repetitive physical activity. and tendon ruptures in the United States military, 1997 to 2015.
Developed from descriptions by Cook et al. 24,25
One controversial aspect in elucidating the pathophysiology
of AT is whether inflammation is present in the tendon. Early
studies 10,26 found no evidence of inflammation in chronic AT,
but more recent studies using immunohistochemistry and
molecular biology techniques have found that inflammatory
cells (e.g., T and B lymphocytes, mast cells) and proinflamma-
tory mediators (e.g., interleukin-1, interleukin-6, transform- Figure 4 shows that there was an increase in incidence rates of
ing growth factor-β) can be present in various stages of the AT from 1997 to 2000: in 1997 there were 2.80 cases/1000
pathophysiology, especially early in the process. 27–29 However, person-yr and in 2001 there were 4.89 cases/1000 person-yr
compared to other types of immune-driven pathologies such (a 75% increase). Between 2009 and 2015 incidence rates rose
as rheumatoid arthritis, the number of inflammatory cells is from 4.34 to 5.10 cases/1000 person-yr (an 18% increase).
small. In general, when microdamage occurs inflammatory For Achilles tendon rupture, the incidence rose from 0.19
2
substances such as cytokines (e.g., interleukins, growth fac- case/1000 person-yr in 1997 to 0.48 case/1000 person-yr in
tors) are released as part of the healing process. Cytokines and 2001, but rates remained relatively constant after that time.
growth factors are released not only by leucocytes but also
by tenocytes and cytokines have been shown to be vigorous Risk Factors for AT
27
stimulators of collagen synthesis. In AT, it is important to
22
note that, in addition to any such inflammation that might af- Prospective studies are those that first obtain from partici-
fect the tendon itself, inflammation of the paratenon can also pants data relating to various factors that might be associated
occur, resulting in paratenonitis, as described earlier. Exten- with AT and then track the individuals over time to see who
12
sive clinical experience of one of the authors (RP) with sol- develops the condition. If the incidence of AT is higher in par-
diers suggests that irritation and inflammation (paratenonitis) ticipants with particular characteristics or other factors than
can arise from externally applied pressure from, for example, in participants without those characteristics or factors, then
ill-fitting or excessively protruding sections of boots or run- those characteristics or factors are considered to increase risk.
ning shoes. Studies of this type have found the following factors increase
the risk for AT: higher body mass index, 7,35,36 black race,
35
Some evidence suggests the pain experienced in association prior tendinopathy or fracture, higher alcohol consump-
35
with AT is due to the neovascularization and the ingrowth of tion, lower plantar flexion strength, greater weekly volume
35
7
new nerve fibers in association with this process since blood of running, more years of running, use of spiked or shock
37
37
vessels and nerves often grow together. 28,30,31 However, tendons absorbing shoes, training in cold weather, and for women,
37
38
Achilles Tendinopathy | 127