Page 108 - JSOM Winter 2019
P. 108
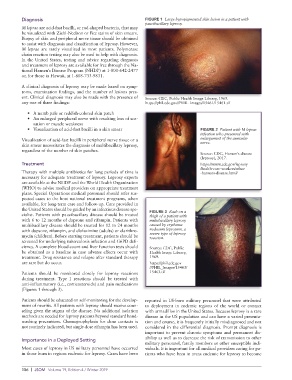
Diagnosis FIGURE 1 Large hypopigmented skin lesion in a patient with
paucibacillary leprosy.
M leprae are acid-fast bacilli, or rod-shaped bacteria, that may
be visualized with Ziehl-Neelson or Fite stains of skin smears.
Biopsy of skin and peripheral nerve tissue should be obtained
to assist with diagnosis and classification of leprosy. However,
M leprae are rarely visualized in most patients. Polymerase
chain reaction testing may also be used to help with diagnosis.
In the United States, testing and advice regarding diagnosis
and treatment of leprosy are available for free through the Na-
tional Hansen’s Disease Program (NHDP) at 1-800-642-2477
or, for those in Hawaii, at 1-808-733-9831.
A clinical diagnosis of leprosy may be made based on symp-
toms, examination findings, and the number of lesions pres-
ent. Clinical diagnosis may also be made with the presence of Source: CDC, Public Health Image Library, 1969.
any one of three findings: https://phil.cdc.gov//PHIL_Images/15461/15461.tif
• A numb pale or reddish-colored skin patch
• An enlarged peripheral nerve with resulting loss of sen-
sation or muscle weakness
• Visualization of acid-fast bacilli in a skin smear FIGURE 2 Patient with M leprae
infection who presented with
Visualization of acid-fast bacilli in peripheral nerve tissue or a enlargement of the auricular
skin smear necessitates the diagnosis of multibacillary leprosy, nerve.
regardless of the number of skin patches.
Source: CDC, Hansen’s disease
(leprosy), 2017.
Treatment https://www.cdc.gov/leprosy
/health-care-workers/other
Therapy with multiple antibiotics for long periods of time is -hansens-disease.html/
necessary for adequate treatment of leprosy. Leprosy experts
are available at the NHDP and the World Health Organization
(WHO) to advise medical providers on appropriate treatment
plans. Special Operations medical personnel should refer sus-
pected cases to the host national treatment programs, when
available, for long-term care and follow-up. Care provided in
the United States should be guided by an infectious disease spe- FIGURE 3 Rash on a
cialist. Patients with paucibacillary disease should be treated thigh of a patient with
with 6 to 12 months of dapsone and rifampin. Patients with multibacillary leprosy
multibacillary disease should be treated for 12 to 24 months caused by erythema
with dapsone, rifampin, and clofazimine (adults) or clarithro- nodosum leprosum, a
mycin (children). Before starting treatment, patients should be severe type of leprosy
reaction.
screened for underlying tuberculosis infection and G6PD defi-
ciency. A complete blood count and liver function tests should Source: CDC, Public
be obtained as a baseline in case adverse effects occur with Health Image Library,
treatment. Drug resistance and relapse after standard therapy 1969.
are rare but do occur. https://phil.cdc.gov
//PHIL_Images/15463/
Patients should be monitored closely for leprosy reactions 15463.tif
during treatment. Type 1 reactions should be treated with
anti-inflammatory (i.e., corticosteroids) and pain medications
(Figures 1 through 3).
Patients should be educated on self-monitoring for the develop- reported in US-born military personnel that were attributed
ment of neuritis. All patients with leprosy should receive coun- to deployment in endemic regions of the world or contact
seling given the stigma of the disease. No additional isolation with armadillos in the United States. Because leprosy is a rare
methods are needed for leprosy patients beyond standard hand- disease in the US population and can have a varied presenta-
washing precautions. Chemoprophylaxis for close contacts is tion and course, it is frequently initially misdiagnosed and not
not routinely indicated, but single-dose rifampin has been used. considered in the differential diagnosis. Prompt diagnosis is
important to prevent chronic symptoms and permanent dis-
Importance in a Deployed Setting ability as well as to decrease the risk of transmission to other
military personnel, family members or other susceptible indi-
Most cases of leprosy in US military personnel have occurred viduals. It is important for all medical providers caring for pa-
in those born in regions endemic for leprosy. Cases have been tients who have been in areas endemic for leprosy to become
106 | JSOM Volume 19, Edition 4 / Winter 2019