Page 103 - JSOM Summer 2018
P. 103
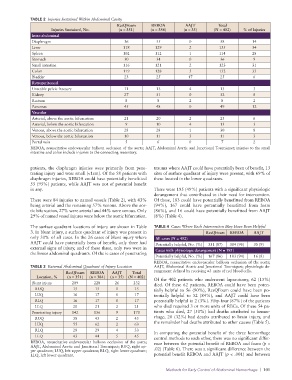
TABLE 2 Injuries Sustained Within Abdominal Cavity
ResQFoam REBOA AAJT Total
Injuries Sustained, No. (n = 351) (n = 384) (n = 35) (N = 402) % of Injuries
Intra-abdominal
Diaphragm 36 55 0 58 14
Liver 118 129 2 135 34
Spleen 102 112 1 114 28
Stomach 30 34 0 36 9
Small intestine 116 121 2 123 31
Colon 119 128 5 132 33
Bladder 23 25 17 25 6
Retroperitoneal
Unstable pelvic fracture 11 13 4 13 3
Kidney 27 31 0 32 8
Rectum 8 8 2 8 2
Pancreas 45 48 0 49 12
Vascular
Arterial, above the aortic bifurcation 21 20 2 23 6
Arterial, below the aortic bifurcation 9 10 4 13 3
Venous, above the aortic bifurcation 28 28 1 30 8
Venous, below the aortic bifurcation 10 11 3 11 3
Portal vein 5 6 0 7 2
REBOA, resuscitative endovascular balloon occlusion of the aorta; AAJT, Abdominal Aortic and Junctional Tourniquet; injuries to the small
intestine and colon include injuries to the connecting mesentery.
patients, the diaphragm injuries were primarily from pene- trauma where AAJT could have potentially been of benefit, 13
trating injury and were small (<1cm). Of the 58 patients with sites of surface quadrant of injury were present, with 69% of
diaphragm injuries, REBOA could have potentially benefitted these located in the lower quadrants.
55 (95%) patients, while AAJT was not of potential benefit
in any. There were 195 (49%) patients with a significant physiologic
derangement that contributed to their need for intervention.
There were 84 injuries to named vessels (Table 2), with 43% Of these, 183 could have potentially benefitted from REBOA
being arterial and the remaining 57% venous. Above the aor- (94%), 167 could have potentially benefitted from foam
tic bifurcation, 27% were arterial and 44% were venous. Only (86%), and 16 could have potentially benefitted from AAJT
29% of named vessel injures were below the aortic bifurcation. (8%) (Table 4).
The surface quadrant locations of injury are shown in Table TABLE 4 Cases Where Each Intervention May Have Been Helpful
3. In blunt injury, a surface quadrant of injury was present in ResQFoam REBOA AAJT
only 30% of all cases. In the 26 cases of blunt injury where All cases (N = 402)
AAJT could have potentially been of benefit, only three had Potentially helpful, No. (%) 351 (87) 384 (96) 35 (9)
external signs of injury, and of these three, only two were in
the lower abdominal quadrants. Of the ie cases of penetrating Cases with physiologic derangement (N = 195)
Potentially helpful, No. (%) 167 (86) 183 (94) 16 (8)
REBOA, resuscitative endovascular balloon occlusion of the aorta;
TABLE 3 External Abdominal Quadrant of Injury Location AAJT, Abdominal Aortic and Junctional Tourniquet; physiologic de-
ResQFoam REBOA AAJT Total rangement defined by receiving ≥3 units of red blood cells.
Location, % (n = 351) (n = 384) (n = 35) (N = 402) Of the 402 patients who underwent laparotomy, 62 (15%)
Blunt injury 209 228 26 232 died. Of these 62 patients, REBOA could have been poten-
RUQ 15 15 1 15 tially helpful to 56 (90%), ResQFoam could have been po-
LUQ 16 17 0 17 tentially helpful to 52 (84%), and AAJT could have been
RLQ 16 17 0 17 potentially helpful in 2 (3%). Fifty-four (87%) of the patients
LLQ 20 21 2 21 who died required 3 or more units of RBCs. Of these 54 pa-
Penetrating injury 142 156 9 170 tients who died, 27 (50%) had deaths attributed to hemor-
RUQ 38 43 2 45 rhage, 20 (32%) had deaths attributed to brain injury, and
LUQ 55 62 2 63 the remainder had deaths attributed to other causes (Table 5).
RLQ 28 29 4 33 In comparing the potential benefit of the three hemorrhage
LLQ 43 44 5 45 control methods to each other, there was no significant differ-
REBOA, resuscitative endovascular balloon occlusion of the aorta; ence between the potential benefit of REBOA and foam (p =
AAJT, Abdominal Aortic and Junctional Tourniquet; RUQ, right up- .02) (Table 6). There was a significant difference between the
per quadrant; LUQ, left upper quadrant; RLQ, right lower quadrant;
LLQ, left lower quadrant. potential benefit REBOA and AAJT (p < .001) and between
Methods for Early Control of Abdominal Hemorrhage | 101