Page 100 - JSOM Summer 2018
P. 100
Methods for Early Control of Abdominal Hemorrhage
An Assessment of Potential Benefit
1
2
Paul M. Cantle, MD, MBT, FRCSC *; Matthew J. Hurley, BSc ;
3
Michael D. Swartz, PhD ; John B. Holcomb, MD, FACS 4
ABSTRACT
4–6
Background: Noncompressible truncal hemorrhage (NCTH) for compressible hemorrhage and extremity hemorrhage,
after injury is associated with a mortality increase that is un- NCTH accounts for 60% to 70% of potentially preventable
7
changed during the past 20 years. Current treatment consists deaths. A challenge in abdominal and pelvic injury hemor-
of rapid transport and emergent intervention. Three early hem- rhage control is the inability to apply direct manual pressure
orrhage control interventions that may improve survival are or effective proximal control to the site of a bleed. Reported
placement of a resuscitative endovascular balloon occlusion mortality rates for hypotensive patients requiring a trauma lap-
8,9
of the aorta (REBOA), injection of intracavitary self-expand- arotomy are 21% to 46%, and it is generally understood that
ing foam, and application of the Abdominal Aortic Junctional the faster a patient receives hemorrhage control, the better is
Tourniquet (AAJT ). The goal of this work was to ascertain the outcome. 10,11 With this in mind, hemorrhage control, even if
™
whether patients with uncontrolled abdominal or pelvic hem- temporary, should be achieved as early as possible. Three novel
orrhage might benefit by the early or prehospital use of one methods for early control of abdominal and pelvic hemorrhage
of these interventions. Methods: This was a single-center ret- currently exist.
rospective study of patients who received a trauma laparot-
omy from 2013 to 2015. Operative reports were reviewed. One method, resuscitative endovascular balloon occlusion of
The probable benefit of each hemorrhage control method was the aorta (REBOA), involves placing a balloon catheter within
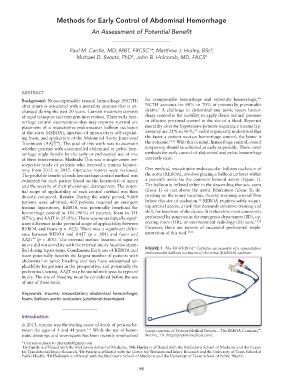
evaluated for each patient based on the location(s) of injury a patient’s aorta via the common femoral artery (Figure 1).
and the severity of their physiologic derangement. The poten- The balloon is inflated either in the descending thoracic aorta
tial scope of applicability of each control method was then (Zone 1) or just above the aortic bifurcation (Zone 3), de-
directly compared. Results: During the study period, 9,608 pending on the injury location, thereby stopping arterial flow
12
patients were admitted; 402 patients required an emergent below this site of occlusion. REBOA requires safely acquir-
trauma laparotomy. REBOA was potentially beneficial for ing arterial access, a task that demands extensive training and
hemorrhage control in 384 (96%) of patients, foam in 351 skill, for insertion of the device. It is therefore most commonly
(87%), and AAJT in 35 (9%). There was no statistically signif- performed by surgeons in the emergency department (ED), op-
icant difference in the potential scope of applicability between erating room (OR), or interventional radiology (IR) suite. 13,14
REBOA and foam (p = .022). There was a significant differ- However, there are reports of successful prehospital imple-
ence between REBOA and AAJT (p < .001) and foam and mentation of this tool. 15,16
AAJT (p < .001). The external surface location of signs of
™
injury did not correlate with the internal injury location identi-
™
fied during laparotomy. Conclusion: Early use of REBOA and FIGURE 1 The ER-REBOA Catheter, an example of a resuscitative
foam potentially benefits the largest number of patients with endovascular balloon occlusion of the aorta (REBOA) catheter.
abdominal or pelvic bleeding and may have widespread ap-
plicability for patients in the preoperative, and potentially the
prehospital, setting. AAJT may be useful with specific types of
injury. The site of bleeding must be considered before the use
of any of these tools.
Keywords: trauma; resuscitation; abdominal hemorrhage;
foam; balloon aortic occlusion; junctional tourniquet
Introduction
In 2013, trauma was the leading cause of death of persons be-
tween the ages of 1 and 44 years. While the use of hemo- Image courtesy of Prytime Medical Devices – The REBOA Company ,
1–3
™
static dressings and tourniquets has been recently emphasized Boerne, TX (http://prytimemedical.com).
*Correspondence to pmcantle@gmail.com
1 Dr Cantle is affiliated with the McGovern School of Medicine. Mr Hurley is affiliated with the McGovern School of Medicine and the Center
2
for Translational Injury Research. Dr Swartz is affiliated with the Center for Translational Injury Research and the University of Texas School of
3
4
Public Health. Dr Holcomb is affiliated with the McGovern School of Medicine and the University of Texas School of Public Health. .
98