Page 74 - Journal of Special Operations Medicine - Winter 2015
P. 74
Although at least some of the current symptoms listed Symptoms of a TBI overlap with other neurological in-
above are required for a diagnosis of mTBI, the Na- juries, just like PTSD.
tional Institute of Neurological Disease and Stroke has
compiled a list of symptoms commonly associated with So, Which Is It?
a TBI (Table 1). 24
How much overlap is there between TBI and PTSD? The
The severity of TBI is normally defined by the acute in- overlap is substantial and difficult to separate out unless
jury characteristics and not by the severity of symptoms a complete history (medical, deployment, and incident
at random points after trauma. Severe TBIs are hard to history) is available. We will go into some detail to high-
25
miss. The mild to moderate TBIs, which make up 80% light how TBI and PTSD overlap, and Figure 3 sum-
to 90% of TBI cases, are less obvious, making identifi- marizes the diagnostic overlap of symptoms and criteria
cation of affected individuals difficult. The problem is between PTSD and TBI/PCS.
twofold. (1) Many times the individual who suffers a
TBI does not know what happened. One wakes up with-
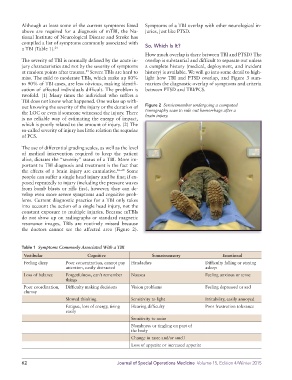
out knowing the severity of the injury or the duration of Figure 2 Servicemember undergoing a computed
the LOC or even if someone witnessed the injury. There tomography scan to rule out hemorrhage after a
brain injury.
is no reliable way of estimating the energy of impact,
which is poorly related to the amount of injury. (2) The
so-called severity of injury has little relation the sequelae
of PCS.
The use of differential grading scales, as well as the level
of medical intervention required to keep the patient
alive, dictates the “severity” status of a TBI. More im-
portant to TBI diagnosis and treatment is the fact that
the effects of a brain injury are cumulative. 26–28 Some
people can suffer a single head injury and be fine; if ex-
posed repeatedly to injury (including the pressure waves
from bomb blasts or rifle fire), however, they can de-
velop even more severe symptoms and cognitive prob-
lems. Current diagnostic practice for a TBI only takes
into account the action of a single head injury, not the
constant exposure to multiple injuries. Because mTBIs
do not show up on radiographs or standard magnetic
resonance images, TBIs are routinely missed because
the doctors cannot see the affected area (Figure 2).
Table 1 Symptoms Commonly Associated With a TBI
Vestibular Cognitive Somatosensory Emotional
Feeling dizzy Poor concentration, cannot pay Headaches Difficulty falling or staying
attention, easily distracted asleep
Loss of balance Forgetfulness, can’t remember Nausea Feeling anxious or tense
things
Poor coordination, Difficulty making decisions Vision problems Feeling depressed or sad
clumsy
Slowed thinking Sensitivity to light Irritability, easily annoyed
Fatigue, loss of energy, tiring Hearing difficulty Poor frustration tolerance
easily
Sensitivity to noise
Numbness or tingling on part of
the body
Change in taste and/or smell
Loss of appetite or increased appetite
62 Journal of Special Operations Medicine Volume 15, Edition 4/Winter 2015