Page 137 - Journal of Special Operations Medicine - Winter 2014
P. 137
to aspiration include severe trismus, coagulopathy and of oral stimulation and pressure, thereby reducing gag
inability of the patient to cooperate with the procedure. 6 reflex and movement.
• Use a 10mL syringe with an 18- or 20-gauge needle
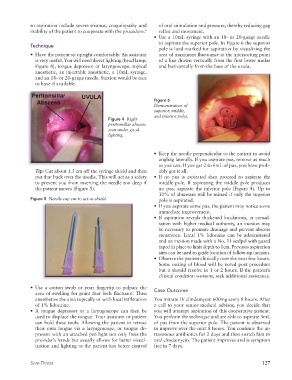
to aspirate the superior pole. In Figure 6 the superior
Technique
pole is land-marked for aspiration by visualizing the
• Have the patient sit upright comfortably. An assistant area of maximum fluctuance at the intersecting point
is very useful. You will need direct lighting (head lamp; of a line drawn vertically from the first lower molar
Figure 4), tongue depressor or laryngoscope, topical and horizontally from the base of the uvula.
anesthetic, an injectable anesthetic, a 10mL syringe,
and an 18- or 20-gauge needle. Suction would be nice
to have if available.
Figure 6
Demonstration of
superior, middle,
and inferior poles.
Figure 4 Right
peritonsillar abscess
seen under good
lighting.
• Keep the needle perpendicular to the patient to avoid
angling laterally. If you aspirate pus, remove as much
as you can. If you get 2 to 6mL of pus, you have prob-
Tip: Cut about 1.5 cm off the syringe shield and then ably got it all.
put that back over the needle. This will act as a safety • If no pus is aspirated then proceed to aspirate the
to prevent you from inserting the needle too deep if middle pole. If aspirating the middle pole produces
the patient moves (Figure 5). no pus, aspirate the inferior pole (Figure 4). Up to
30% of abscesses will be missed if only the superior
Figure 5 Needle cap cut to act as shield. pole is aspirated.
• If you aspirate some pus, the patient may notice some
immediate improvement.
• If aspiration reveals thickened loculations, in consul-
tation with higher medical authority, an incision may
be necessary to promote drainage and prevent abscess
recurrence. Local 1% lidocaine can be administered
and an incision made with a No. 11 scalpel with guard
taped in place to limit depth to 1cm. Previous aspiration
sites can be used to guide location of follow-up incision.
• Observe the patient clinically over the next few hours.
Some oozing of blood will be noted post procedure
but it should resolve in 1 or 2 hours. If the patient’s
clinical condition worsens, seek additional assistance.
• Use a cotton swab or your fingertip to palpate the
area of swelling for point that feels fluctuant. Then Case Outcome
anesthetize the area topically or with local infiltration You initiate IV clindamycin 600mg every 8 hours. After
of 1% lidocaine. a call to your senior medical advisor, you decide that
• A tongue depressor or a laryngoscope can then be you will attempt aspiration of this cooperative patient.
used to displace the tongue. Your assistant or patient You perform the technique and are able to aspirate 3mL
can hold these tools. Allowing the patient to retract of pus from the superior pole. The patient is observed
their own tongue via a laryngoscope, or tongue de- to improve over the next 8 hours. You continue the in-
pressor with an attached pen light not only frees the travenous antibiotics for 2 days and then switch him to
provider’s hands but usually allows for better visual- oral clindamycin. The patient improves and is symptom
ization and lighting as the patient has better control free in 7 days.
Sore Throat 127