Page 136 - Journal of Special Operations Medicine - Winter 2014
P. 136
level of care requires increased use of medical person- Figure 2 Peritonsillar abscess.
nel and resources. If the mission environment does not
allow for this level of continued care, oral clindamycin
may be considered due to its easy dosing routine and
excellent oral bioavailability (approximately 90%). 3
Good initial choices for parenteral antibiotics include:
• Clindamycin 600mg IV in adults every 8 hours
• Ampicillin/sulbactam 3g IV every 6 hours in adults
• Cefazolin 1g every 8 hours plus metronidazole 500mg
IV every 8 hours
Steroids
Limited evidence supports the benefit of steroids in
PTA and PTC. Several trials appear to demonstrate a
benefit, but these results have not been consistently re-
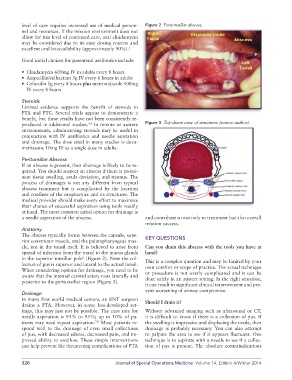
produced in additional studies. In remote or austere Figure 3 Top-down view of structures (source: author).
4,5
environments, administering steroids may be useful in
conjunction with IV antibiotics and needle aspiration
and drainage. The dose cited in many studies is dexa-
methasone 10mg IV as a single dose in adults.
Peritonsillar Abscess
If an abscess is present, then drainage is likely to be re-
quired. You should suspect an abscess if there is promi-
nent tissue swelling, uvula deviation, and trismus. The
process of drainages is not any different from typical
abscess treatment but is complicated by the location
and confines of the oropharynx and its structures. The
medical provider should make every effort to maximize
their chance of successful aspiration using tools readily
at hand. The most common initial option for drainage is
a needle aspiration of the abscess. and contribute to not only to treatment but also overall
mission success.
Anatomy
The abscess typically forms between the capsule, supe-
rior constrictor muscle, and the palatopharyngeus mus- KEY QUESTIONS
cle, not in the tonsil itself. It is believed to arise from Can you drain this abscess with the tools you have at
spread of infection from the tonsil to the mucus glands hand?
in the superior tonsillar pole (Figure 2). Note the col- This is a complex question and may be limited by your
6
lection of pus is superior and lateral to the actual tonsil. own comfort or scope of practice. The actual technique
When considering options for drainage, you need to be or procedure is not overly complicated and it can be
aware that the internal carotid artery runs laterally and done safely in an austere setting. In the right situation,
posterior to the peritonsillar region (Figure 3).
it can result in significant clinical improvement and pre-
vent worsening of airway compromise.
Drainage
In many first world medical centers, an ENT surgeon Should I drain it?
drains a PTA. However, in some less-developed set-
tings, this may just not be possible. The cure rate for Without advanced imaging such as ultrasound or CT,
needle aspiration is 93% to 95%; up to 10% of pa- it is difficult to know if there is a collection of pus. If
tients may need repeat aspiration. Most patients re- the swelling is impressive and displacing the uvula, then
7,8
spond well to the drainage of even small collections drainage is probably necessary. You can also attempt
of pus, with decreased edema, decreased pain, and im- to palpate the area to see if it appears fluctuant. One
proved ability to swallow. These simple interventions technique is to aspirate with a needle to see if a collec-
can help prevent life threatening complications of PTA tion of pus is present. The absolute contraindications
126 Journal of Special Operations Medicine Volume 14, Edition 4/Winter 2014