Page 78 - ATP-P 11th Ed
P. 78
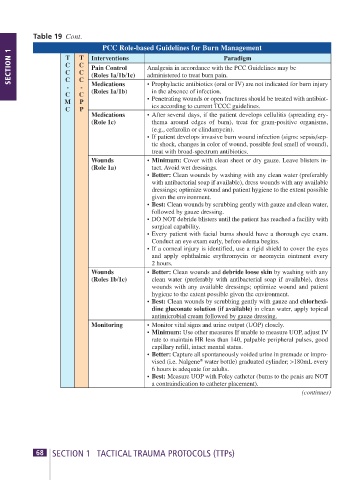
Table 19 Cont.
PCC Role-based Guidelines for Burn Management
SECTION 1 T T Interventions Analgesia in accordance with the PCC Guidelines may be
Paradigm
C C
Pain Control
C C
(Roles 1a/1b/1c)
administered to treat burn pain.
C
- C - Medications • Prophylactic antibiotics (oral or IV) are not indicated for burn injury
C C (Roles 1a/1b) in the absence of infection.
M P • Penetrating wounds or open fractures should be treated with antibiot-
C P ics according to current TCCC guidelines.
Medications • After several days, if the patient develops cellulitis (spreading ery-
(Role 1c) thema around edges of burn), treat for gram-positive organisms,
(e.g., cefazolin or clindamycin).
• If patient develops invasive burn wound infection (signs: sepsis/sep-
tic shock, changes in color of wound, possible foul smell of wound),
treat with broad-spectrum antibiotics.
Wounds • Minimum: Cover with clean sheet or dry gauze. Leave blisters in-
(Role 1a) tact. Avoid wet dressings.
• Better: Clean wounds by washing with any clean water (preferably
with antibacterial soap if available), dress wounds with any available
dressings; optimize wound and patient hygiene to the extent possible
given the environment.
• Best: Clean wounds by scrubbing gently with gauze and clean water,
followed by gauze dressing.
• DO NOT debride blisters until the patient has reached a facility with
surgical capability.
• Every patient with facial burns should have a thorough eye exam.
Conduct an eye exam early, before edema begins.
• If a corneal injury is identified, use a rigid shield to cover the eyes
and apply ophthalmic erythromycin or neomycin ointment every
2 hours.
Wounds • Better: Clean wounds and debride loose skin by washing with any
(Roles 1b/1c) clean water (preferably with antibacterial soap if available), dress
wounds with any available dressings; optimize wound and patient
hygiene to the extent possible given the environment.
• Best: Clean wounds by scrubbing gently with gauze and chlorhexi-
dine gluconate solution (if available) in clean water, apply topical
antimicrobial cream followed by gauze dressing.
Monitoring • Monitor vital signs and urine output (UOP) closely.
• Minimum: Use other measures If unable to measure UOP, adjust IV
rate to maintain HR less than 140, palpable peripheral pulses, good
capillary refill, intact mental status.
• Better: Capture all spontaneously voided urine in premade or impro-
vised (i.e. Nalgene water bottle) graduated cylinder; >180mL every
®
6 hours is adequate for adults.
• Best: Measure UOP with Foley catheter (burns to the penis are NOT
a contraindication to catheter placement).
(continues)
68 SECTION 1 TACTICAL TRAUMA PROTOCOLS (TTPs) ATP-P Handbook 11th Edition 69