Page 77 - ATP-P 11th Ed
P. 77
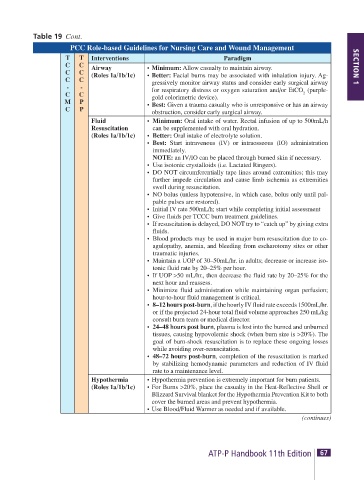
Table 19 Cont.
PCC Role-based Guidelines for Nursing Care and Wound Management
T T Interventions Paradigm
C C Airway • Minimum: Allow casualty to maintain airway. SECTION 1
C C (Roles 1a/1b/1c) • Better: Facial burns may be associated with inhalation injury. Ag-
C C gressively monitor airway status and consider early surgical airway
- - for respiratory distress or oxygen saturation and/or EtCO (purple-
C C gold colorimetric device). 2
M P • Best: Given a trauma casualty who is unresponsive or has an airway
C P obstruction, consider early surgical airway.
Fluid • Minimum: Oral intake of water. Rectal infusion of up to 500mL/h
Resuscitation can be supplemented with oral hydration.
(Roles 1a/1b/1c) • Better: Oral intake of electrolyte solution.
• Best: Start intravenous (IV) or intraosseous (IO) administration
immediately.
NOTE: an IV/IO can be placed through burned skin if necessary.
• Use isotonic crystalloids (i.e. Lactated Ringers).
• DO NOT circumferentially tape lines around extremities; this may
further impede circulation and cause limb ischemia as extremities
swell during resuscitation.
• NO bolus (unless hypotensive, in which case, bolus only until pal-
pable pulses are restored).
• Initial IV rate 500mL/h; start while completing initial assessment
• Give fluids per TCCC burn treatment guidelines.
• If resuscitation is delayed, DO NOT try to “catch up” by giving extra
fluids.
• Blood products may be used in major burn resuscitation due to co-
agulopathy, anemia, and bleeding from escharotomy sites or other
traumatic injuries.
• Maintain a UOP of 30–50mL/hr. in adults; decrease or increase iso-
tonic fluid rate by 20–25% per hour.
• If UOP >50 mL/hr., then decrease the fluid rate by 20–25% for the
next hour and reassess.
• Minimize fluid administration while maintaining organ perfusion;
hour-to-hour fluid management is critical.
• 8–12 hours post-burn, if the hourly IV fluid rate exceeds 1500mL/hr.
or if the projected 24-hour total fluid volume approaches 250 mL/kg
consult burn team or medical director.
• 24–48 hours post burn, plasma is lost into the burned and unburned
tissues, causing hypovolemic shock (when burn size is >20%). The
goal of burn-shock resuscitation is to replace these ongoing losses
while avoiding over-resuscitation.
• 48–72 hours post-burn, completion of the resuscitation is marked
by stabilizing hemodynamic parameters and reduction of IV fluid
rate to a maintenance level.
Hypothermia • Hypothermia prevention is extremely important for burn patients.
(Roles 1a/1b/1c) • For Burns >20%, place the casualty in the Heat-Reflective Shell or
Blizzard Survival blanket for the Hypothermia Prevention Kit to both
cover the burned areas and prevent hypothermia.
• Use Blood/Fluid Warmer as needed and if available.
(continues)
66 SECTION 1 TACTICAL TRAUMA PROTOCOLS (TTPs) ATP-P Handbook 11th Edition 67