Page 97 - JSOM Winter 2022
P. 97
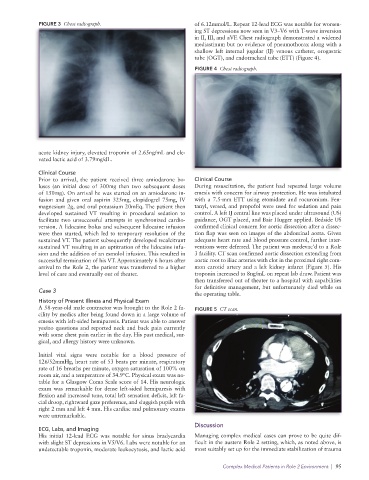
FIGURE 3 Chest radiograph. of 6.12mmol/L. Repeat 12-lead ECG was notable for worsen-
ing ST depressions now seen in V3–V6 with T-wave inversion
in II, III, and aVF. Chest radiograph demonstrated a widened
mediastinum but no evidence of pneumothorax along with a
shallow left internal jugular (IJ) venous catheter, orogastric
tube (OGT), and endotracheal tube (ETT) (Figure 4).
FIGURE 4 Chest radiograph.
acute kidney injury, elevated troponin of 2.65ng/mL and ele-
vated lactic acid of 3.79mg/dL.
Clinical Course
Prior to arrival, the patient received three amiodarone bo- Clinical Course
luses (an initial dose of 300mg then two subsequent doses During resuscitation, the patient had repeated large volume
of 150mg). On arrival he was started on an amiodarone in- emesis with concern for airway protection. He was intubated
fusion and given oral aspirin 325mg, clopidogrel 75mg, IV with a 7.5-mm ETT using etomidate and rocuronium. Fen-
magnesium 2g, and oral potassium 20mEq. The patient then tanyl, versed, and propofol were used for sedation and pain
developed sustained VT resulting in procedural sedation to control. A left IJ central line was placed under ultrasound (US)
facilitate two unsuccessful attempts in synchronized cardio- guidance, OGT placed, and Bair Hugger applied. Bedside US
version. A lidocaine bolus and subsequent lidocaine infusion confirmed clinical concern for aortic dissection after a dissec-
were then started, which led to temporary resolution of the tion flap was seen on images of the abdominal aorta. Given
sustained VT. The patient subsequently developed recalcitrant adequate heart rate and blood pressure control, further inter-
sustained VT resulting in an uptitration of the lidocaine infu- ventions were deferred. The patient was medevac’d to a Role
sion and the addition of an esmolol infusion. This resulted in 3 facility. CT scan confirmed aortic dissection extending from
successful termination of his VT. Approximately 6 hours after aortic root to iliac arteries with clot in the proximal right com-
arrival to the Role 2, the patient was transferred to a higher mon carotid artery and a left kidney infarct (Figure 5). His
level of care and eventually out of theater. troponin increased to 8ng/mL on repeat lab draw. Patient was
then transferred out of theater to a hospital with capabilities
for definitive management, but unfortunately died while on
Case 3
the operating table.
History of Present Illness and Physical Exam
A 58-year-old male contractor was brought to the Role 2 fa- FIGURE 5 CT scan.
cility by medics after being found down in a large volume of
emesis with left-sided hemiparesis. Patient was able to answer
yes/no questions and reported neck and back pain currently
with some chest pain earlier in the day. His past medical, sur-
gical, and allergy history were unknown.
Initial vital signs were notable for a blood pressure of
126/52mmHg, heart rate of 53 beats per minute, respiratory
rate of 16 breaths per minute, oxygen saturation of 100% on
room air, and a temperature of 34.9°C. Physical exam was no-
table for a Glasgow Coma Scale score of 14. His neurologic
exam was remarkable for dense left-sided hemiparesis with
flexion and increased tone, total left sensation deficit, left fa-
cial droop, rightward gaze preference, and sluggish pupils with
right 2 mm and left 4 mm. His cardiac and pulmonary exams
were unremarkable.
Discussion
ECG, Labs, and Imaging
His initial 12-lead ECG was notable for sinus bradycardia Managing complex medical cases can prove to be quite dif-
with slight ST depressions in V5/V6. Labs were notable for an ficult in the austere Role 2 setting, which, as noted above, is
undetectable troponin, moderate leukocytosis, and lactic acid most suitably set up for the immediate stabilization of trauma
Complex Medical Patients in Role 2 Environment | 95