Page 96 - JSOM Winter 2022
P. 96
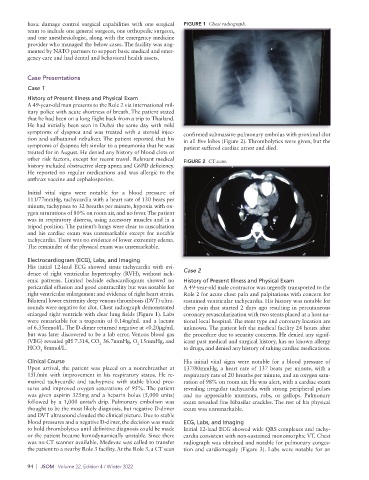
basic damage control surgical capabilities with one surgical FIGURE 1 Chest radiograph.
team to include one general surgeon, one orthopedic surgeon,
and one anesthesiologist, along with the emergency medicine
provider who managed the below cases. The facility was aug-
mented by NATO partners to support basic medical and emer-
gency care and had dental and behavioral health assets.
Case Presentations
Case 1
History of Present Illness and Physical Exam
A 49-year-old man presents to the Role 2 via international mil-
itary police with acute shortness of breath. The patient stated
that he had been on a long flight back from a trip to Thailand.
He had initially been seen in Dubai the same day with mild
symptoms of dyspnea and was treated with a steroid injec- confirmed submassive pulmonary embolus with proximal clot
tion and salbutamol nebulizer. The patient reported that his in all five lobes (Figure 2). Thrombolytics were given, but the
symptoms of dyspnea felt similar to a pneumonia that he was patient suffered cardiac arrest and died.
treated for in August. He denied any history of blood clots or
other risk factors, except for recent travel. Relevant medical FIGURE 2 CT scan.
history included obstructive sleep apnea and G6PD deficiency.
He reported no regular medications and was allergic to the
anthrax vaccine and cephalosporins.
Initial vital signs were notable for a blood pressure of
111/77mmHg, tachycardia with a heart rate of 130 beats per
minute, tachypnea to 32 breaths per minute, hypoxia with ox-
ygen saturations of 80% on room air, and no fever. The patient
was in respiratory distress, using accessory muscles and in a
tripod position. The patient’s lungs were clear to auscultation
and his cardiac exam was unremarkable except for notable
tachycardia. There was no evidence of lower extremity edema.
The remainder of the physical exam was unremarkable.
Electrocardiogram (ECG), Labs, and Imaging
His initial 12-lead ECG showed sinus tachycardia with evi-
dence of right ventricular hypertrophy (RVH), without isch- Case 2
emic patterns. Limited bedside echocardiogram showed no History of Present Illness and Physical Exam
pericardial effusion and good contractility but was notable for A 49-year-old male contractor was urgently transported to the
right ventricular enlargement and evidence of right heart strain. Role 2 for acute chest pain and palpitations with concern for
Bilateral lower extremity deep venous thrombosis (DVT) ultra- sustained ventricular tachycardia. His history was notable for
sounds were negative for clot. Chest radiograph demonstrated chest pain that started 2 days ago resulting in percutaneous
enlarged right ventricle with clear lung fields (Figure 1). Labs coronary revascularization with two stents placed at a host na-
were remarkable for a troponin of 0.14ng/mL and a lactate tional local hospital. The stent type and coronary location are
of 6.35mmol/L. The D-dimer returned negative at <0.20μg/mL unknown. The patient left the medical facility 24 hours after
but was later discovered to be a lab error. Venous blood gas the procedure due to security concerns. He denied any signif-
(VBG) revealed pH 7.314, CO 36.7mmHg, O 15mmHg, and icant past medical and surgical history, has no known allergy
2
2
HCO 8mmol/L. to drugs, and denied any history of taking cardiac medications.
3
Clinical Course His initial vital signs were notable for a blood pressure of
Upon arrival, the patient was placed on a nonrebreather at 137/80mmHg, a heart rate of 137 beats per minute, with a
15L/min with improvement in his respiratory status. He re- respiratory rate of 20 breaths per minute, and an oxygen satu-
mained tachycardic and tachypneic with stable blood pres- ration of 98% on room air. He was alert, with a cardiac exam
sures and improved oxygen saturations of 95%. The patient revealing irregular tachycardia with strong peripheral pulses
was given aspirin 325mg and a heparin bolus (5,000 units) and no appreciable murmurs, rubs, or gallops. Pulmonary
followed by a 1,000 units/h drip. Pulmonary embolism was exam revealed fine bibasilar crackles. The rest of his physical
thought to be the most likely diagnosis, but negative D-dimer exam was unremarkable.
and DVT ultrasound clouded the clinical picture. Due to stable
blood pressures and a negative D-dimer, the decision was made ECG, Labs, and Imaging
to hold thrombolytics until definitive diagnosis could be made Initial 12-lead ECG showed wide QRS complexes and tachy-
or the patient became hemodynamically unstable. Since there cardia consistent with non-sustained monomorphic VT. Chest
was no CT scanner available, Medevac was called to transfer radiograph was obtained and notable for pulmonary conges-
the patient to a nearby Role 3 facility. At the Role 3, a CT scan tion and cardiomegaly (Figure 3). Labs were notable for an
94 | JSOM Volume 22, Edition 4 / Winter 2022