Page 103 - JSOM Fall 2022
P. 103
Exfiltration was performed using a collapsible litter, travers skills, availability of bottled or generated oxygen and ventila
ing a 30to40degree incline over 2 miles. During the 1hour tors, and the patient’s subsequent sedation needs. Because of
exfiltration, spontaneous regular respirations returned, and these limitations and the ability of some obtunded patients to
her GCS improved to 9T with eye opening to speech (E3) and maintain oxygenation with simple airway adjuncts (e.g., posi
motor localization to pain (M5). The previously sluggish right tioning, nasopharyngeal airway), intubation and cricothyroi
pupil regained reactivity and constricted to 1 mm with light. dotomy should be reserved for those who fail to maintain a
The patient required short periods of increased ventilation to goal SpO > 90%.
2
maintain an endtidal CO of 30–35mmHg. Blood loss from
2
her penetrating head wound was significant but estimation of Herniation is the mechanical result of uncontrolled ICP whereby
volume was not possible. Blood products were available but brain parenchyma is translated across intracranial structures
not administered. such as the tentorium cerebelli, falx cerebri, and foramen mag
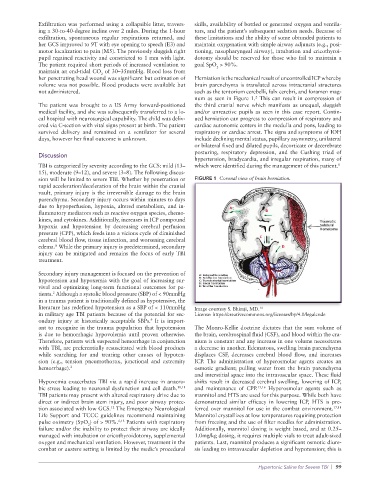
num as seen in Figure 1. This can result in compression of
2
The patient was brought to a US Army forwardpositioned the third cranial nerve which manifests as unequal, sluggish
medical facility, and she was subsequently transferred to a lo and/or unreactive pupils as seen in this case report. Contin
cal hospital with neurosurgical capability. The child was deliv ued herniation can progress to compression of respiratory and
ered via Csection with vital signs present at birth. The patient cardiac autonomic centers in the medulla and pons, leading to
survived delivery and remained on a ventilator for several respiratory or cardiac arrest. The signs and symptoms of IOH
days, however her final outcome is unknown. include declining mental status, pupillary asymmetry, unilateral
or bilateral fixed and dilated pupils, decorticate or decerebrate
posturing, respiratory depression, and the Cushing triad of
Discussion
hypertension, bradycardia, and irregular respiration, many of
TBI is categorized by severity according to the GCS: mild (13– which were identified during the management of this patient. 8
15), moderate (9–12), and severe (3–8). The following discus
sion will be limited to severe TBI. Whether by penetration or FIGURE 1 Coronal view of brain herniation.
rapid acceleration/deceleration of the brain within the cranial
vault, primary injury is the irreversible damage to the brain
parenchyma. Secondary injury occurs within minutes to days
due to hypoperfusion, hypoxia, altered metabolism, and in
flammatory mediators such as reactive oxygen species, chemo
kines, and cytokines. Additionally, increases in ICP compound
hypoxia and hypotension by decreasing cerebral perfusion
pressure (CPP), which feeds into a vicious cycle of diminished
cerebral blood flow, tissue infarction, and worsening cerebral
edema. While the primary injury is predetermined, secondary
8
injury can be mitigated and remains the focus of early TBI
treatment.
Secondary injury management is focused on the prevention of
hypotension and hypoxemia with the goal of increasing sur
vival and optimizing longterm functional outcomes for pa
2
tients. Although a systolic blood pressure (SBP) of < 90mmHg
in a trauma patient is traditionally defined as hypotensive, the
literature has redefined hypotension as a SBP of < 110mmHg Image courtesy S. Bhimji, MD.
14
in military age TBI patients because of the potential for sec License: https://creativecommons.org/licenses/by/4.0/legalcode
9
ondary injury at historically acceptable SBPs. It is import
ant to recognize in the trauma population that hypotension The MonroKellie doctrine dictates that the sum volume of
is due to hemorrhagic hypovolemia until proven otherwise. the brain, cerebrospinal fluid (CSF), and blood within the cra
Therefore, patients with suspected hemorrhage in conjunction nium is constant and any increase in one volume necessitates
with TBI, are preferentially resuscitated with blood products a decrease in another. Edematous, swelling brain parenchyma
while searching for and treating other causes of hypoten displaces CSF, decreases cerebral blood flow, and increases
sion (e.g., tension pneumothorax, junctional and extremity ICP. The administration of hyperosmolar agents creates an
hemorrhage). 2 osmotic gradient; pulling water from the brain parenchyma
and interstitial space into the intravascular space. These fluid
Hypoxemia exacerbates TBI via a rapid increase in anaero shifts result in decreased cerebral swelling, lowering of ICP,
bic stress leading to neuronal dysfunction and cell death. 10,11 and maintenance of CPP. 15,16 Hyperosmolar agents such as
TBI patients may present with altered respiratory drive due to mannitol and HTS are used for this purpose. While both have
direct or indirect brain stem injury, and poor airway protec demonstrated similar efficacy in lowering ICP, HTS is pre
tion associated with low GCS. The Emergency Neurological ferred over mannitol for use in the combat environment. 17,18
12
Life Support and TCCC guidelines recommend maintaining Mannitol crystallizes at low temperatures requiring protection
pulse oximetry (SpO ) of > 90%. 6,13 Patients with respiratory from freezing and the use of filter needles for administration.
2
failure and/or the inability to protect their airway are ideally Additionally, mannitol dosing is weight based, and at 0.25–
managed with intubation or cricothyroidotomy, supplemental 1.0mg/kg dosing, it requires multiple vials to treat adultsized
oxygen and mechanical ventilation. However, treatment in the patients. Last, mannitol produces a significant osmotic diure
combat or austere setting is limited by the medic’s procedural sis leading to intravascular depletion and hypotension; this is
Hypertonic Saline for Severe TBI | 99