Page 54 - JSOM Summer 2022
P. 54
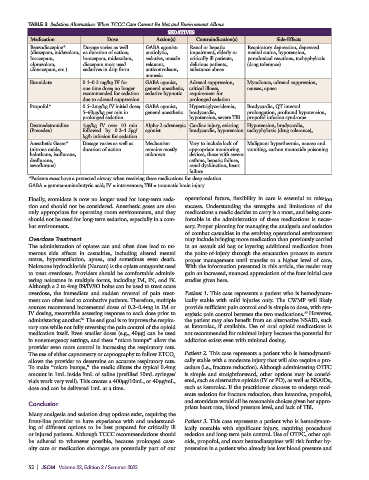
TABLE 3 Sedation Alternatives When TCCC Care Cannot Be Met and Environment Allows
SEDATIVES
Medication Dose Action(s) Contraindication(s) Side-Effects
Benzodiazepine* Dosage varies as well GABA agonist: Renal or hepatic Respiratory depression, depressed
(diazepam, midazolam, as duration of action; anxiolytic, impairment, elderly or mental status, hypotension,
lorazepam, lorazepam, midazolam, sedative, muscle critically ill patients, paradoxical reactions, tachyphylaxis
alprazolam, diazepam most used relaxant, delirious patients, (drug tolerance)
clonazepam, etc.) sedatives in drip form anticonvulsant, substance abuse
amnesic
Etomidate 0.1–0.3 mg/kg IV for GABA agonist, Adrenal suppression, Myoclonus, adrenal suppression,
one time dose; no longer general anesthetic, critical illness, nausea, apnea
recommended for sedation sedative hypnotic requirement for
due to adrenal suppression prolonged sedation
Propofol* 0.5–2mg/kg IV initial dose; GABA agonist, Hypertriglyceridemia, Bradycardia, QT interval
5–60μg/kg per min in general anesthetic bradycardia, prolongation, profound hypotension,
prolonged sedation hypotension, severe TBI propofol infusion syndrome
Dexmedetomidine 1μg/kg IV over 10 min Alpha-2 adrenergic Cardiac injury, existing Hypotension, bradycardia,
(Precedex) followed by 0.2–1.5μg/ agonist bradycardia, hypotension tachyphylaxis (drug tolerance),
kg/h infusion for sedation
Anesthetic Gases* Dosage varies as well as Mechanism Vary to include lack of Malignant hyperthermia, nausea and
(nitrous oxide, duration of action remains mostly appropriate monitoring vomiting, carbon monoxide poisoning
halothane, isoflurane, unknown devices, those with severe
desflurane, asthma, hepatic failure,
sevoflurane) renal dysfunction, heart
failure
*Patients must have a protected airway when receiving these medications for deep sedation.
GABA = gamma-aminobutyric acid; IV = intravenous; TBI = traumatic brain injury.
Finally, etomidate is now no longer used for long-term seda- operational future, flexibility in care is essential to mission
tion and should not be considered. Anesthetic gases are also success. Understanding the strengths and limitations of the
only appropriate for operating room environments, and they medications a medic decides to carry is a must, and being com-
should not be used for long-term sedation, especially in a com- fortable in the administration of these medications is neces-
bat environment. sary. Proper planning for managing the analgesia and sedation
of combat casualties in the evolving operational environment
Overdose Treatment may include bringing more medication than previously carried
The administration of opiates can and often does lead to nu- in an assault aid bag or layering additional medication from
merous side effects in casualties, including altered mental the point-of-injury through the evacuation process to ensure
status, hypoventilation, apnea, and sometimes even death. proper management until transfer to a higher level of care.
Naloxone hydrochloride (Narcan) is the opiate antagonist used With the information presented in this article, the reader may
to treat overdoses. Providers should be comfortable adminis- gain an increased, nuanced appreciation of the four initial case
tering naloxone in multiple forms, including IM, IN, and IV. studies given here.
Although a 2 to 4mg IN/IV/IO bolus can be used to treat acute
overdose, the immediate and sudden reversal of pain treat- Patient 1. This case represents a patient who is hemodynam-
ment can often lead to combative patients. Therefore, multiple ically stable with mild injuries only. The CWMP will likely
sources recommend incremental doses of 0.2–0.4mg in IM or provide sufficient pain control and is simple to dose, with syn-
IV dosing, meanwhile assessing response to each dose prior to ergistic pain control between the two medications. However,
27
26
administering another. The end goal is to improve the respira- the patient may also benefit from an alternative NSAID, such
tory rate while not fully reversing the pain control of the opioid as ketorolac, if available. Use of oral opioid medications is
medication itself. Even smaller doses (e.g., 40mg) can be used not recommended for minimal injury because the potential for
in nonemergency settings, and these “micro bumps” allow the addiction exists even with minimal dosing.
provider even more control in increasing the respiratory rate.
The use of either capnometry or capnography to follow ETCO Patient 2. This case represents a patient who is hemodynami-
2
allows the provider to determine an accurate respiratory rate. cally stable with a moderate injury that will also require a pro-
To make “micro bumps,” the medic dilutes the typical 0.4mg cedure (i.e., fracture reduction). Although administering OTFC
amount in 1mL inside 9mL of saline (prefilled 10mL syringes/ is simple and straightforward, other options may be consid-
vials work very well). This creates a 400mg/10mL, or 40mg/mL, ered, such as alternative opioids (IV or PO), as well as NSAIDs,
dose and can be delivered 1mL at a time. such as ketorolac. If the practitioner chooses to undergo mod-
erate sedation for fracture reduction, then ketamine, propofol,
and etomidate would all be reasonable choices given her appro-
Conclusion
priate heart rate, blood pressure level, and lack of TBI.
Many analgesia and sedation drug options exist, requiring the
front-line provider to have experience with and understand- Patient 3. This case represents a patient who is hemodynam-
ing of different options to be best prepared for critically ill ically unstable with significant injury, requiring procedural
or injured patients. Although TCCC recommendations should sedation and long-term pain control. Use of OTFC, other opi-
be adhered to whenever possible, because prolonged casu- oids, propofol, and most benzodiazepines will risk further hy-
alty care or medication shortages are potentially part of our potension in a patient who already has low blood pressure and
52 | JSOM Volume 22, Edition 2 / Summer 2022