Page 53 - JSOM Summer 2022
P. 53
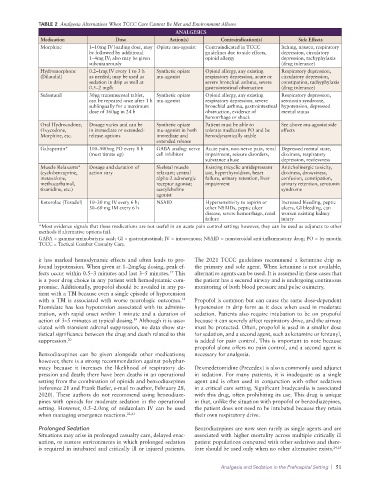
TABLE 2 Analgesia Alternatives When TCCC Care Cannot Be Met and Environment Allows
ANALGESICS
Medication Dose Action(s) Contraindication(s) Side Effects
Morphine 1–10mg IV loading dose, may Opiate mu-agonist Contraindicated in TCCC Itching, nausea, respiratory
be followed by additional guidelines due to side effects, depression, circulatory
1–4mg IV; also may be given opioid allergy depression, tachyphylaxis
subcutaneously (drug tolerance)
Hydromorphone 0.2–1mg IV every 1 to 3 h Synthetic opiate Opioid allergy, any existing Respiratory depression,
(Dilaudid) as needed; may be used as mu-agonist respiratory depression, acute or circulatory depression,
sedation in drip as well at severe bronchial asthma, severe constipation, tachyphylaxis
0.5–2 mg/h gastrointestinal obstruction (drug tolerance)
Sufentanil 30mg transmucosal tablet, Synthetic opiate Opioid allergy, any existing Respiratory depression,
can be repeated once after 1 h mu-agonist respiratory depression, severe serotonin syndrome,
sublingually for a maximum bronchial asthma, gastrointestinal hypotension, depressed
dose of 360mg in 24 h obstruction, evidence of mental status
hemorrhage or shock
Oral Hydrocodone, Dosage varies and can be Synthetic opiate Patient must be able to See above mu-agonist side
Oxycodone, in immediate or extended- mu-agonist in both tolerate medication PO and be effects
Morphine, etc. release options immediate and hemodynamically stable
extended release
Gabapentin* 100–900mg PO every 8 h GABA analog: nerve Acute pain, non-nerve pain, renal Depressed mental state,
(must titrate up) cell inhibitor impairment, seizure disorders, dizziness, respiratory
substance abuse depression, restlessness
Muscle Relaxants* Dosage and duration of Skeletal muscle Existing tricyclic antidepressant Anticholinergic toxicity,
(cyclobenzaprine, action vary relaxant; central use, hyperthyroidism, heart dizziness, drowsiness,
metaxalone, alpha-2 adrenergic failure, urinary retention, liver confusion, constipation,
methocarbamol, receptor agonist; impairment urinary retention, serotonin
tizanidine, etc.) acetylcholine syndrome
agonist
Ketorolac (Toradol) 10–30 mg IV every 6 h; NSAID Hypersensitivity to aspirin or Increased bleeding, peptic
30–60 mg IM every 6 h other NSAIDs, peptic ulcer ulcers, GI bleeding, can
disease, severe hemorrhage, renal worsen existing kidney
failure injury
*Most evidence signals that these medications are not useful in an acute pain control setting; however, they can be used as adjuncts to other
methods if alternative options fail.
GABA = gamma-aminobutyric acid; GI = gastrointestinal; IV = intravenous; NSAID = nonsteroidal anti-inflammatory drug; PO = by mouth;
TCCC = Tactical Combat Casualty Care.
it has marked hemodynamic effects and often leads to pro- The 2021 TCCC guidelines recommend a ketamine drip as
found hypotension. When given at 1–2mg/kg dosing, peak ef- the primary and sole agent. When ketamine is not available,
fects occur within 0.5–3 minutes and last 3–5 minutes. This alternative agents can be used. It is assumed in these cases that
17
is a poor drug choice in any patient with hemodynamic com- the patient has a secured airway and is undergoing continuous
promise. Additionally, propofol should be avoided in any pa- monitoring of both blood pressure and pulse oximetry.
tient with a TBI because even a single episode of hypotension
with a TBI is associated with worse neurologic outcomes. Propofol is common but can cause the same dose-dependent
18
Etomidate has less hypotension associated with its adminis- hypotension in drip form as it does when used in moderate
tration, with rapid onset within 1 minute and a duration of sedation. Patients also require intubation to be on propofol
action of 3–5 minutes at typical dosing. Although it is asso- because it can severely affect respiratory drive, and the airway
19
ciated with transient adrenal suppression, no data show sta- must be protected. Often, propofol is used in a smaller dose
tistical significance between the drug and death related to this for sedation, and a second agent, such as ketamine or fentanyl,
suppression. 20 is added for pain control. This is important to note because
propofol alone offers no pain control, and a second agent is
Benzodiazepines can be given alongside other medications; necessary for analgesia.
however, there is a strong recommendation against polyphar-
macy because it increases the likelihood of respiratory de- Dexmedetomidine (Precedex) is also a commonly used adjunct
pression and death; there have been deaths in an operational in sedation. For many patients, it is inadequate as a single
setting from the combination of opioids and benzodiazepines agent and is often used in conjunction with other sedatives
(reference 21 and Frank Butler, e-mail to author, February 28, in a critical care setting. Significant bradycardia is associated
2020). These authors do not recommend using benzodiaze- with this drug, often prohibiting its use. This drug is unique
pines with opioids for moderate sedation in the operational in that, unlike the situation with propofol or benzodiazepines,
setting. However, 0.5–2.0mg of midazolam IV can be used the patient does not need to be intubated because they retain
when managing emergence reactions. 22,23 their own respiratory drive.
Prolonged Sedation Benzodiazepines are now seen rarely as single agents and are
Situations may arise in prolonged casualty care, delayed evac- associated with higher mortality across multiple critically ill
uation, or austere environments in which prolonged sedation patient populations compared with other sedatives and there-
is required in intubated and critically ill or injured patients. fore should be used only when no other alternative exists. 24,25
Analgesia and Sedation in the Prehospital Setting | 51