Page 142 - JSOM Spring 2020
P. 142
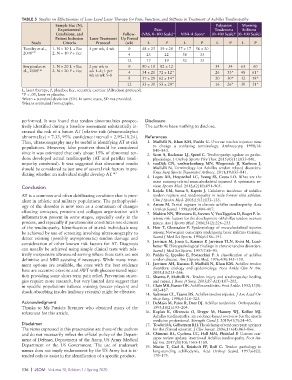
TABLE 5 Studies on Effectiveness of Low-Level Laser Therapy for Pain, Function, and Stiffness in Treatment of Achilles Tendinopathy
Sample Size (N), Palpation Morning
Experimental Pain Tenderness Stiffness
Conditions, and Follow- (VAS, 0–100 Scale) a VISA-A Score a (0–100 Scale) (0–100 Scale)
b
Patient Inclusion Laser Treatment Up Period
Study Criteria Protocol (wk) L P L P L P L P
Tumilty et al., 1. N = 10 L + Ecc 3 per wk, 4 wk 0 48 ± 25 39 ± 20 57 ± 17 56 ± 20
2008 135 2. N = 10 P + Ecc 4 25 22 38 35
12 17 19 32 35
Stergioulas et 1. N = 20 L + Ecc 2 per wk in 0 80 ± 10 82 ± 12 34 34 63 60
al., 2008 136 2. N = 20 P + Ecc wk 1–4; 1 per 4 54 ± 20 72 ± 12* 26 33* 48 61*
wk in wk 5–8
8 37 ± 28 62 ± 14* 20 30* 32 58*
12 33 ± 30 53 ± 20* 16 26* 30 51*
L, laser therapy; P, placebo; Ecc, eccentric exercise (Alfredson protocol).
*P < .05, laser vs placebo.
a Mean ± standard deviation (SD). In some cases, SD not provided.
b Means estimated from graphs.
performed. It was found that tendon abnormalities prospec- Disclosure
tively identified during a baseline assessment substantially in- The authors have nothing to disclose.
creased the risk of a future AT [relative risk (abnormality/no
abnormality) = 7.33, 95% confidence interval = 2.95–18.24]. References
Thus, ultrasonography may be useful in identifying AT at-risk 1. Maffulli N, Khan KM, Puddu G. Overuse tendon injuries: time
populations. However, false positives should be considered to change a confusing terminology. Arthroscopy. 1998;14:
840–843.
since it was estimated that only about 15% of abnormal ten- 2. Scott A, Backman LJ, Speed C. Tendinopathy: update on patho-
dons developed actual tendinopathy (AT and patellar tendi- physiology. J Orthop Sports Phy Ther. 2015;45(11):833–841.
nopathy combined). It was suggested that ultrasound results 3. vanDijk CN, vanSterkenburg MN, Wiegerinck JI, Karlsson J,
should be considered as just one of several risk factors in pre- Maffulli N. Terminology for Achilles tendon related disorders.
dicting whether an individual might develop AT. 147 Knee Surg Sports Traumatol Arthosc. 2011;19:835–841.
4. Lopes AD, Hespanhol LC, Yeung SS, Costa LO. What are the
main running-related musculoskeletal injuries? A systematic re-
Conclusion view. Sports Med. 2012;42(10):891–905.
5. Kujala UM, Sarna S, Kaprio J. Cululative incidence of anhilles
AT is a common and often debilitating condition that is prev- tendon rupture and tendinopathy in male former elite athletes.
alent in athletic and military populations. The pathophysiol- Clin J Sports Med. 2005;15(3):133–135.
ogy of the disorder is now seen as a continuum of changes 6. Astom M. Partial rupture in chronic achilles tendinopathy. Acta
Orthop Scand. 1998;69(4):404–407.
effecting tenocytes, proteins and collagen organization with 7. Mahieu NN, Witvrouw E, Stevens V, VanTiggelen D, Roget P. In-
inflammation present in some stages, especially early in the trinsic risk factors for the development ofAchilles tendon overuse
process, and especially if paratenonitis constitutes one element injury. Am J Sports Med. 2006;34(2):226–235.
of the tendinopathy. Identification of at-risk individuals may 8. Heir T, Glomsaker P. Epidemiology of musculoskeletal injuries
be achieved by use of screening involving ultrasonography to among Norwegian conscripts undergoing basic military training.
detect existing (possibly asymptomatic) tendon damage and Scand J Med Sci Sports. 1996;6:186–191.
consideration of other known risk factors for AT. Diagnosis 9. Jarvinen M, Jozsa L, Kannus P, Jarvinen TLN, Kvist M, Lead-
can usually be achieved using simple clinical tests with rela- better W. Histopathological findings in chronic tendon disorders.
Scand J Med Sci Sports. 1997;7:86–95.
tively inexpensive ultrasound serving where these tests are not 10. Puddu G, Ippolito E, Postacchini F. A classification of achilles
definitive and MRI assisting if necessary. While many treat- tendon disease. Am J Sports Med. 1976;4(4):145–150.
ment options are available, the ones with the best evidence 11. Jarvinen AH, Kannus P, Maffulli N, Khan KM. Achilles tendon
base are eccentric exercise and SWT with glucocorticoid injec- disorders: etiology and epidemiology. Foot Ankle Clin N Am.
2005;10:255–266.
tion providing some short-term pain relief. Prevention strate- 12. Sharma P, Maffulli N. Tendon injury and tendinopathy: healing
gies require more research, but very limited data suggest that and repair. J Bone Jt Surg. 2005;87-A(1):187–202.
in specific populations balance training (soccer players) and 13. Clain MR, Baxter DE. Achilles tendinitis. Foot Ankle. 1992;13(8):
shock-absorbing insoles (military recruits) might be effective. 482–487.
14. Saltzman CL, Tearse DS. Achilles tendon injuries. J Am Acad Or-
thop Surg. 1998;6:316–325.
Acknowledgment 15. DeMaio M, Paine R, Drez DJ. Achilles tendonitis. Orthopaedics.
Thanks to Ms Patricia Bremner who obtained many of the 1995;18(2):195–204.
references for this article. 16. Kaplan K, Olivencia O, Dreger M, Hanney WJ, Kolber MJ.
Achilles tendinopathy: an evidence-based overview for the sports
medicine professional. Strength Cond J. 2019;41(5):24–40.
Disclaimer 17. Towler DA, Gelberman RH. Thealchemy of tendon repair: a primer
The views expressed in this presentation are those of the authors for the (S)mad scientist. J Clin Invest. 2006;116(4):863–866.
and do not necessarily reflect the official policy of the Depart- 18. Chimenti RL, Cychosz CC, Hall MM, Phisitkul P. Current con-
ment of Defense, Department of the Army, US Army Medical cepts review update: insertional Achilles tendinopathy. Foot An-
kle Int. 2017;30(10):1160–1169.
Department or the US Government. The use of trademark 19. Movin T, Gad A, Reinholt FP, Rolf C. Tendon pathology in
names does not imply endorsement by the US Army but is in- long-standing achillodynia. Acta Orthop Scand. 1997;68(2):
tended only to assist in the identification of a specific product. 170–175.
136 | JSOM Volume 20, Edition 1 / Spring 2020