Page 69 - JSOM Summer 2018
P. 69
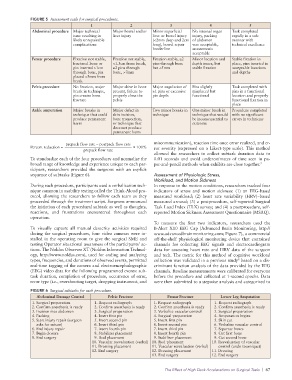
FIGURE 5 Assessment scale for surgical procedures.
1 2 3 4 5
Abdominal procedure Major technical Major bowel and/or Minor superficial No internal organ Task completed
issue resulting in liver injury liver or bowel injury injury, packing rapidly in a safe
likely unrepairable (<2mm deep and 2cm of abdomen manner with
complications long), bowel repair was acceptable, technical excellence
borderline anastomosis
acceptable
Femur procedure Fixation not stable, Fixation not stable, Fixation stable, ≥2 Minor location and Stable fixation in
fractured bone or <1.5cm from break, pins through bone depth issues, but place, pins inserted in
pin inserted >1cm ≥2 pins through but <5mm stable fixation acceptable locations
through bone, pin bone, >7mm and depths
placed <5mm from
break
Pelvis procedure No fixation, major Major skive in bone Major angulation of Pins slightly Task completed with
break in technique, present, failure to ≥1 pins or excessive misplaced but pins in a functional
pin creates bone properly close the pin depth functional location and properly
fracture pelvis functional fixation in
place
Ankle amputation Major breaks in Major defect in Two minor breaks in One minor break in Procedure completed
technique that could skin incision, technique technique that would with no significant
produce permanent bone transection, be inconsequential to errors in technique
harm or technique that outcome
does not produce
permanent harm
prepack flow rate – postpack flow rate miscommunication), reaction time once error realized, and er-
Percent reduction = 100% ror severity (expressed on a Likert-type scale). This method
prepack flow rate
allowed the researchers to collect subtask duration data to
To standardize each of the four procedures and normalize the 0.01 seconds and avoid underestimates of time seen in pa-
broad range of knowledge and experience unique to each par- per-and-pencil methods when exhibits are close together. 7
ticipant, researchers provided the surgeons with an explicit
sequence of subtasks (Figure 6). Assessment of Physiologic Stress,
Workload, and Motion Sickness
During each procedure, participants used a verbalization tech- In response to the motion conditions, researchers tracked four
nique common in usability testing called the Think-Aloud pro- indicators of stress and motion sickness: (1) an EEG-based
tocol, allowing the researchers to follow each team as they measured workload; (2) heart rate variability (HRV)–based
proceeded through the treatment script. Surgeons announced measured arousal; (3) a postprocedure, self-reported Surgical
the initiation of each procedural subtask as well as thoughts, Task Load Index (TLX) survey; and (4) a postprocedure, self-
reactions, and frustrations encountered throughout each reported Motion Sickness Assessment Questionnaire (MSAQ).
operation.
To measure the first two indicators, researchers used the
To visually capture all manual dexterity activities required B-Alert X10 EEG Cap (Advanced Brain Monitoring, http://
during the surgical procedures, four video cameras were in- www.advancedbrainmonitoring.com; Figure 7), a commercial
stalled in the operating room to give the surgical SME and off-the-shelf physiological monitoring device that contained
testing Operator situational awareness of the participants’ ac- channels for collecting EEG signals and electrocardiogram
tions. The Noldus Observer XT (Noldus Information Technol- data for assessing heart rate and HRV data of the surgeon
ogy, http://www.noldus.com), used for coding and analyzing and tech. The metric for this method of cognitive workload
types, frequencies, and durations of observed events, permitted collection was validated in a previous study based on a dis-
8
real-time tagging of the camera and electroencephalographic criminant function analysis of the data provided by the EEG
(EEG) video data for the following programmed events: sub- channels. Baseline measurements were calibrated for everyone
task duration, completion of procedure, occurrence of error, before the procedure and collected at 1-second epochs. Data
error type (i.e., overshooting target, dropping instrument, and were then submitted to a stepwise analysis and categorized to
FIGURE 6 Surgical subtasks for each procedure.
Abdominal Damage Control Pelvic Fracture Femur Fracture Lower Leg Amputation
1. Surgical preparation 1. Request radiograph 1. Request radiograph 1. Request radiograph
2. Confirm anesthesia is ready 2. Confirm anesthesia is ready 2. Confirm anesthesia is ready 2. Confirm anesthesia is ready
3. Incision into abdomen 3. Surgical preparation 3. Verbalize vascular control 3. Surgical preparation
4. Packing 4. Insert first pin 4. Surgical preparation 4. Amputation begins
5. Start injury repair (surgeon 5. Insert second pin 5. Insert first pin 5. Skin cut
asks for suture) 6. Insert third pin 6. Insert second pin 6. Verbalize vascular control
6. End injury repair 7. insert fourth pin 7. Insert third pin 7. Separate bones
7. Begin closure 8. Stabilizer placement 8. Insert fourth pin 8. Cut first bone
8. End surgery 9. Rod placement 9. Stabilizer placement 9. Cut second bone
10. Vascular reevaluation (verbal) 10. Rod placement 10. Reevaluation of vascular
11. Dressing placement 11. Vascular reevaluation (verbal) control (undo tourniquet)
12. End surgery 12. Dressing placement 11. Dressing
13. End surgery 12. End surgery
The Effect of High Deck Accelerations on Surgical Tasks | 67