Page 95 - Journal of Special Operations Medicine - Spring 2017
P. 95
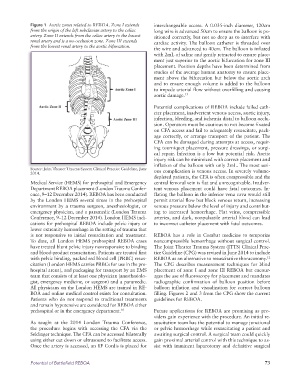
Figure 1 Aortic zones related to REBOA. Zone I extends interchangeable access. A 0.035-inch diameter, 120cm
from the origin of the left subclavian artery to the celiac long wire is advanced 50cm to ensure the balloon is po-
artery. Zone II extends from the celiac artery to the lowest sitioned correctly, but not so deep as to interfere with
renal artery and is a no-occlusion zone. Zone III extends cardiac activity. The balloon catheter is threaded over
from the lowest renal artery to the aortic bifurcation.
the wire and advanced to 40cm. The balloon is inflated
with 2mL of saline and gently retracted to ensure place-
ment just superior to the aortic bifurcation for zone III
placement. Position depths have been determined from
studies of the average human anatomy to ensure place-
ment above the bifurcation but below the aortic arch
and to ensure enough volume is added to the balloon
to impede arterial flow without overfilling and causing
aortic damage. 13
Potential complications of REBOA include failed cath-
eter placement, inadvertent venous access, aortic injury,
infection, bleeding, and ischemia distal to balloon occlu-
sion. Operators must be cautious to not become fixated
on CFA access and fail to adequately resuscitate, pack-
age correctly, or arrange transport of the patient. The
CFA can be damaged during attempts at access, requir-
ing tourniquet placement, pressure dressings, or surgi-
cal repair. Infection is a low but potential risk. Aortic
injury risk can be minimized with correct placement and
inflation of the balloon with only 2mL. The most seri-
Source: Joint Theater Trauma System Clinical Practice Guideline, June ous complication is venous access. In severely volume-
2014.
depleted patients, the CFA is often compressible and the
Medical Service (HEMS) for prehospital and Emergency central femoral vein is flat and unrecognizable. Inadver-
Department REBOA placement (London Trauma Confer- tent venous placement could have fatal outcomes. In-
ence, 9–12 December 2014). REBOA has been conducted flating the balloon in the inferior vena cava would still
by the London HEMS several times in the prehospital permit arterial flow but block venous return, increasing
environment by a trauma surgeon, anesthesiologist, or venous pressure below the level of injury and contribut-
emergency physician, and a paramedic (London Trauma ing to increased hemorrhage. Flat veins, compressible
Conference, 9–12 December 2014). London HEMS indi- arteries, and dark, nonpulsatile arterial blood can lead
cations for prehospital REBOA include pelvic injury or to incorrect catheter placement with fatal outcomes.
lower extremity hemorrhage in the setting of trauma that
is not responsive to initial resuscitation and treatment. REBOA has a role in Combat medicine to temporize
To date, all London HEMS prehospital REBOA cases noncompressible hemorrhage without surgical control.
have treated blunt pelvic injury nonresponsive to binding The Joint Theater Trauma System (JTTS) Clinical Prac-
and blood-product resuscitation. Patients are treated first tice Guideline (CPG) was revised in June 2014 to include
with pelvic binding, packed red blood cell (PRBC) resus- REBOA as an alternative to resuscitative thoracotomy.
12
citation (London HEMS carries PRBCs for use in the pre- The CPG describes measurement techniques for blind
hospital arena), and packaging for transport by an EMS placement of zone I and zone III REBOA but encour-
team that consists of at least one physician (anesthesiolo- ages the use of fluoroscopy for placement and mandates
gist, emergency medicine, or surgeon) and a paramedic. radiographic confirmation of balloon position before
All physicians on the London HEMS are trained in RE- balloon inflation and visualization for correct balloon
BOA and online medical control exists for consultation. filling. Figures 2 and 3 from the CPG show the current
Patients who do not respond to traditional treatments guidelines for REBOA.
and remain hypotensive are considered for REBOA either
prehospital or in the emergency department. 10 Future applications for REBOA are promising as pro-
viders gain experience with the procedure. An initial re-
As taught at the 2014 London Trauma Conference, suscitation team has the potential to manage junctional
the procedure begins with accessing the CFA via the or pelvic hemorrhage while resuscitating a patient and
Seldinger technique. The CFA can be accessed bilaterally awaiting surgical control. A surgical team could quickly
using either cut down or ultrasound to facilitate access. gain proximal arterial control with this technique to as-
Once the artery is accessed, an 8F Cordis is placed for sist with imminent laparotomy and definitive surgical
Potential of Battlefield REBOA 73