Page 120 - Journal of Special Operations Medicine - Winter 2016
P. 120
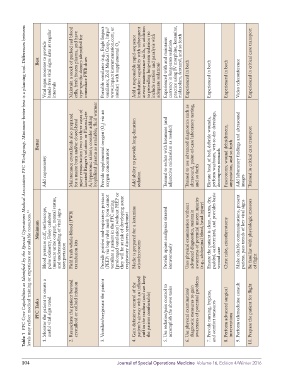
Table 1 PFC Core Capabilities as Identified by the Special Operations Medical Association PFC Workgroup. Minimum-better-best is a planning tool. Differences between
Vital signs monitor to provide intervals immediate FWB draw similar) with supplemental O 2 adequate sedation) Experienced with and maintains currency in long-term sedation midazolam, fentanyl, and so forth Experienced in both Experienced in both Experienced in both Video teleconference
Best hands-free vital signs data at regular Maintain a stock of packed red blood cells, fresh frozen plasma, and have type-specific donors identified for Portable ventilator (e.g., Eagle Impact ventilator, Zoll Medical Corp., http:// www.impact instrumentation.com; or Add a responsible rapid-sequence intubation capability with subsequent airway maintenance skills, in addition to providing long-term sedation (to include suction and paralysis with
Better Maintenance crystalloids also prepared for a major burn and/or closed-head injury resuscitation (two to three cases of lactated Ringer’s solution or PlasmaLyte A; hypertonic saline); consider adding lyophilized plasma as available; fluid warmer Provide supplemental oxygen (O 2 ) via an Add ability to provide long-duration Trained to sedate with ketamine (and adjunctive midazolam as needed) Trained to use advanced diagnostics such as
Add capnometry oxygen concentrator sedation and so forth decompress stomach amputation, and so forth images
Blood pressure cuff, stethoscope, pulse oximetry, Foley catheter and understanding of vital signs interpretation Field fresh whole-blood (FWB) transfusion kits ventilate a patient in the PFC setting respiratory distress syndrome) Medic is prepared for a ketamine cricothyrotomy Provide opiate analgesics titrated intravenously Uses physical examination without advanced diagnostics, maintain (e.g., abdominal bleed, head injury) wound care
levels may reflect medical training or experience or available resources. 11
Minimum (measure urine output), mental status, Provide positive end-expiratory pressure (PEEP) via bag-valve mask (you cannot [prolonged ventilation] without PEEP or they will be at risk of developing acute awareness of potential unseen injuries Ensure the patient is clean, warm, dry, padded, catheterized, and provides basic Make reliable communications, present Be familiar with physiologic stressors
Monitor the patient to create a Resuscitate the patient beyond patient’s airway with an inflated cuff in the trachea (and can keep awareness of potential problems
PFC Tasks useful vital sign trend crystalloid or colloid infusion 3. Ventilate/oxygenate the patient Gain definitive control of the the patient comfortable) Use sedation/pain control to accomplish the above tasks Use physical examination/ diagnostic measures to gain Provide nursing, hygiene, and comfort measures Perform advanced surgical 9. Perform telemedicine consult 10. Prepare the patient for flight
1. 2. 4. 5. 6. 7. 8. interventions
104 Journal of Special Operations Medicine Volume 16, Edition 4/Winter 2016