Page 61 - JSOM Summer 2025
P. 61
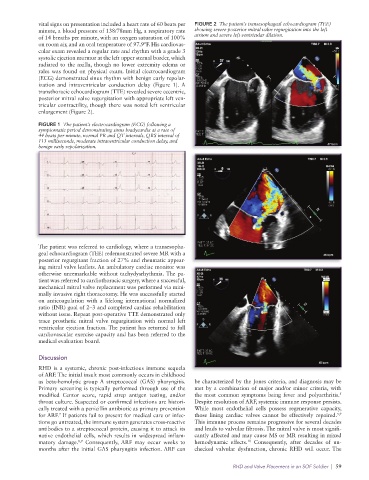
vital signs on presentation included a heart rate of 60 beats per FIGURE 2 The patient’s transesophageal echocardiogram (TEE)
minute, a blood pressure of 138/78mm Hg, a respiratory rate showing severe posterior mitral valve regurgitation into the left
of 14 breaths per minute, with an oxygen saturation of 100% atrium and severe left ventricular dilation.
on room air, and an oral temperature of 97.9°F. His cardiovas-
cular exam revealed a regular rate and rhythm with a grade 3
systolic ejection murmur at the left upper sternal border, which
radiated to the axilla, though no lower extremity edema or
rales was found on physical exam. Initial electrocardiogram
(ECG) demonstrated sinus rhythm with benign early repolar-
ization and intraventricular conduction delay (Figure 1). A
transthoracic echocardiogram (TTE) revealed severe eccentric,
posterior mitral valve regurgitation with appropriate left ven-
tricular contractility, though there was noted left ventricular
enlargement (Figure 2).
FIGURE 1 The patient’s electrocardiogram (ECG) following a
symptomatic period demonstrating sinus bradycardia at a rate of
44 beats per minute, normal PR and QT intervals, QRS interval of
113 milliseconds, moderate intraventricular conduction delay, and
benign early repolarization.
The patient was referred to cardiology, where a transesopha-
geal echocardiogram (TEE) redemonstrated severe MR with a
posterior regurgitant fraction of 27% and rheumatic appear-
ing mitral valve leaflets. An ambulatory cardiac monitor was
otherwise unremarkable without tachydysrhythmia. The pa-
tient was referred to cardiothoracic surgery, where a successful,
mechanical mitral valve replacement was performed via mini-
mally invasive right thoracotomy. He was successfully started
on anticoagulation with a lifelong international normalized
ratio (INR) goal of 2–3 and completed cardiac rehabilitation
without issue. Repeat post-operative TTE demonstrated only
trace prosthetic mitral valve regurgitation with normal left
ventricular ejection fraction. The patient has returned to full
cardiovascular exercise capacity and has been referred to the
medical evaluation board.
Discussion
RHD is a systemic, chronic post-infectious immune sequela
of ARF. The initial insult most commonly occurs in childhood
as beta-hemolytic group A streptococcal (GAS) pharyngitis. be characterized by the Jones criteria, and diagnosis may be
Primary screening is typically performed through use of the met by a combination of major and/or minor criteria, with
5
modified Centor score, rapid strep antigen testing, and/or the most common symptoms being fever and polyarthritis.
throat culture. Suspected or confirmed infections are histori- Despite resolution of ARF, systemic immune response persists.
cally treated with a penicillin antibiotic as primary prevention While most endothelial cells possess regenerative capacity,
5,9
for ARF. If patients fail to present for medical care or infec- those lining cardiac valves cannot be effectively repaired.
7
tions go untreated, the immune system generates cross-reactive This immune process remains progressive for several decades
antibodies to a streptococcal protein, causing it to attack its and leads to valvular fibrosis. The mitral valve is most signifi-
native endothelial cells, which results in widespread inflam- cantly affected and may cause MS or MR resulting in mixed
10
matory damage. Consequently, ARF may occur weeks to hemodynamic effects. Consequently, after decades of un-
8,9
months after the initial GAS pharyngitis infection. ARF can checked valvular dysfunction, chronic RHD will occur. The
RHD and Valve Placement in an SOF Soldier | 59