Page 14 - JSOM Spring 2025
P. 14
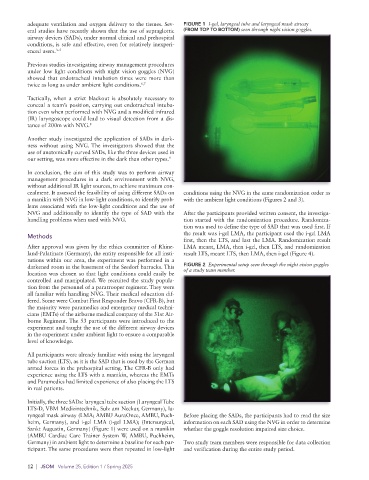
adequate ventilation and oxygen delivery to the tissues. Sev- FIGURE 1 I-gel, laryngeal tube and laryngeal mask airway
eral studies have recently shown that the use of supraglottic (FROM TOP TO BOTTOM) seen through night vision goggles.
airway devices (SADs), under normal clinical and prehospital
conditions, is safe and effective, even for relatively inexperi-
enced users. 3–5
Previous studies investigating airway management procedures
under low light conditions with night vision goggles (NVG)
showed that endotracheal intubation times were more than
twice as long as under ambient light conditions. 6,7
Tactically, when a strict blackout is absolutely necessary to
conceal a team’s position, carrying out endotracheal intuba-
tion even when performed with NVG and a modified infrared
(IR) laryngoscope could lead to visual detection from a dis-
tance of 200m with NVG. 8
Another study investigated the application of SADs in dark-
ness without using NVG. The investigators showed that the
use of anatomically curved SADs, like the three devices used in
our setting, was more effective in the dark than other types. 9
In conclusion, the aim of this study was to perform airway
management procedures in a dark environment with NVG,
without additional IR light sources, to achieve maximum con-
cealment. It assessed the feasibility of using different SADs on conditions using the NVG in the same randomization order as
a manikin with NVG in low-light conditions, to identify prob- with the ambient light conditions (Figures 2 and 3).
lems associated with the low-light conditions and the use of
NVG and additionally to identify the type of SAD with the After the participants provided written consent, the investiga-
handling problems when used with NVG. tion started with the randomization procedure. Randomiza-
tion was used to define the type of SAD that was used first. If
the result was i-gel LMA, the participant used the i-gel LMA
Methods
first, then the LTS, and last the LMA. Randomization result
After approval was given by the ethics committee of Rhine- LMA meant, LMA, then i-gel, then LTS, and randomization
land-Palatinate (Germany), the entity responsible for all insti- result LTS, meant LTS, then LMA, then i-gel (Figure 4).
tutions within our area, the experiment was performed in a
darkened room in the basement of the Seedorf barracks. This FIGURE 2 Experimental setup seen through the night vision goggles
location was chosen so that light conditions could easily be of a study team member.
controlled and manipulated. We recruited the study popula-
tion from the personnel of a paratrooper regiment. They were
all familiar with handling NVG. Their medical education dif-
fered. Some were Combat First Responder Bravo (CFR-B), but
the majority were paramedics and emergency medical techni-
cians (EMTs) of the airborne medical company of the 31st Air-
borne Regiment. The 53 participants were introduced to the
experiment and taught the use of the different airway devices
in the experiment under ambient light to ensure a comparable
level of knowledge.
All participants were already familiar with using the laryngeal
tube suction (LTS), as it is the SAD that is used by the German
armed forces in the prehospital setting. The CFR-B only had
experience using the LTS with a manikin, whereas the EMTs
and Paramedics had limited experience of also placing the LTS
in real patients.
Initially, the three SADs: laryngeal tube suction (Laryngeal Tube
LTS-D, VBM Medizintechnik, Sulz am Neckar, Germany), la-
ryngeal mask airway (LMA; AMBU AuraOnce, AMBU, Puch- Before placing the SADs, the participants had to read the size
heim, Germany), and i-gel LMA (i-gel LMA); (Intersurgical, information on each SAD using the NVG in order to determine
Sankt Augustin, Germany) (Figure 1) were used on a manikin whether the goggle resolution impaired size choice.
(AMBU Cardiac Care Trainer System W, AMBU, Puchheim,
Germany) in ambient light to determine a baseline for each par- Two study team members were responsible for data collection
ticipant. The same procedures were then repeated in low-light and verification during the entire study period.
12 | JSOM Volume 25, Edition 1 / Spring 2025