Page 105 - JSOM Winter 2024
P. 105
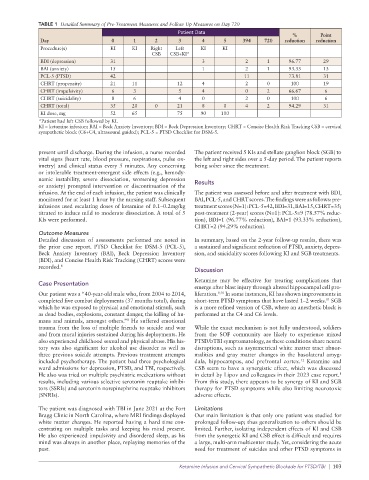
TABLE 1 Detailed Summary of Pre-Treatment Measures and Follow Up Measures on Day 720
Patient Data
% Point
Day 0 1 2 3 4 5 394 720 reduction reduction
Procedure(s) KI KI Right Left KI KI
CSB CSB+KI*
BDI (depression) 31 3 2 1 96.77 29
BAI (anxiety) 15 1 2 1 93.33 13
PCL-5 (PTSD) 42 11 73.81 31
CHRT (propensity) 21 11 12 4 2 0 100 19
CHRT (impulsivity) 6 3 5 4 0 2 66.67 6
CHRT (suicidality) 8 6 4 0 2 0 100 6
CHRT (total) 35 20 0 21 8 0 4 2 94.29 31
KI dose, mg 52 65 75 90 100
*Patient had left CSB followed by KI.
KI = ketamine infusion; BAI = Beck Anxiety Inventory; BDI = Beck Depression Inventory; CHRT = Concise Health Risk Tracking CSB = cervical
sympathetic block (C6+C4, ultrasound guided); PCL-5 = PTSD Checklist for DSM-5.
present until discharge. During the infusion, a nurse recorded The patient received 5 KIs and stellate ganglion block (SGB) to
vital signs (heart rate, blood pressure, respirations, pulse ox- the left and right sides over a 5-day period. The patient reports
imetry) and clinical status every 5 minutes. Any concerning being sober since the treatment.
or intolerable treatment-emergent side effects (e.g., hemody-
namic instability, severe dissociation, worsening depression Results
or anxiety) prompted intervention or discontinuation of the
infusion. At the end of each infusion, the patient was clinically The patient was assessed before and after treatment with BDI,
monitored for at least 1 hour by the nursing staff. Subsequent BAI, PCL-5, and CHRT scores. The findings were as follows: pre-
infusions used escalating doses of ketamine of 0.1–0.2mg/kg treatment scores (N=1): PCL-5=42, BDI=31, BAI=15, CHRT=35;
titrated to induce mild to moderate dissociation. A total of 5 post-treatment (2-year) scores (N=1): PCL-5=9 (78.57% reduc-
KIs were performed. tion), BDI=1 (96.77% reduction), BAI=1 (93.33% reduction),
CHRT=2 (94.29% reduction).
Outcome Measures
Detailed discussion of assessments performed are noted in In summary, based on the 2-year follow-up results, there was
the prior case report. PTSD Checklist for DSM-5 (PCL-5), a sustained and significant reduction of PTSD, anxiety, depres-
Beck Anxiety Inventory (BAI), Beck Depression Inventory sion, and suicidality scores following KI and SGB treatments.
(BDI), and Concise Health Risk Tracking (CHRT) scores were
recorded. 8
Discussion
Ketamine may be effective for treating complications that
Case Presentation
emerge after blast injury through altered hippocampal cell pro-
Our patient was a “40-year-old male who, from 2004 to 2014, liferation. 9,10 In some instances, KI has shown improvements in
completed five combat deployments (37 months total), during short-term PTSD symptoms that have lasted 1–2 weeks. SGB
11
which he was exposed to physical and emotional stimuli, such is a more refined version of CSB, where an anesthetic block is
as dead bodies, explosions, constant danger, the killing of hu- performed at the C4 and C6 levels.
mans and animals, amongst others.” He suffered emotional
8
trauma from the loss of multiple friends to suicide and war While the exact mechanism is not fully understood, soldiers
and from moral injuries sustained during his deployments. He from the SOF community are likely to experience mixed
also experienced childhood sexual and physical abuse. His his- PTSD/bTBI symptomatology, as these conditions share neural
tory was also significant for alcohol use disorder as well as disruptions, such as asymmetrical white matter tract abnor-
three previous suicide attempts. Previous treatment attempts malities and gray matter changes in the basolateral amyg-
12
included psychotherapy. The patient had three psychological dala, hippocampus, and prefrontal cortex. Ketamine and
ward admissions for depression, PTSD, and TBI, respectively. CSB seem to have a synergistic effect, which was discussed
He also was tried on multiple psychiatric medications without in detail by Lipov and colleagues in their 2023 case report.
8
results, including various selective serotonin reuptake inhibi- From this study, there appears to be synergy of KI and SGB
tors (SSRIs) and serotonin norepinephrine reuptake inhibitors therapy for PTSD symptoms while also limiting neurotoxic
(SNRIs). adverse effects.
The patient was diagnosed with TBI in June 2021 at the Fort Limitations
Bragg Clinic in North Carolina, where MRI findings displayed Our main limitation is that only one patient was studied for
white matter changes. He reported having a hard time con- prolonged follow-up; thus generalization to others should be
centrating on multiple tasks and keeping his mind present. limited. Further, isolating independent effects of KI and CSB
He also experienced impulsivity and disordered sleep, as his from the synergetic KI and CSB effect is difficult and requires
mind was always in another place, replaying memories of the a large, multi-arm multicenter study. Yet, considering the acute
past. need for treatment of suicides and other PTSD symptoms in
Ketamine Infusion and Cervical Sympathetic Blockade for PTSD/TBI | 103