Page 95 - JSOM Fall 2022
P. 95
made this a poor option. First, the SLM was still receiving
urgent casualties and it was thought to be quicker to do a sur
gical airway then to attempt direct laryngoscopy with the on
going oral bleeding. Second, a helicopter medical evacuation
was available in 15 minutes. The helicopter did not have the
capability of ventilator support nor monitoring for a sedated
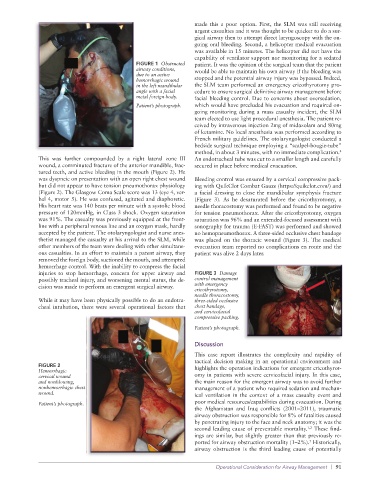
FIGURE 1 Obstructed patient. It was the opinion of the surgical team that the patient
airway conditions, would be able to maintain his own airway if the bleeding was
due to an active
hemorrhagic wound stopped and the potential airway injury was bypassed. Indeed,
in the left mandibular the SLM team performed an emergency cricothyrotomy pro
angle with a facial cedure to ensure surgical definitive airway management before
metal foreign body. facial bleeding control. Due to concerns about oversedation,
Patient’s photograph. which would have precluded his evacuation and required on
going monitoring during a mass casualty incident, the SLM
team elected to use light procedural anesthesia. The patient re
ceived by intravenous injection 2mg of midazolam and 80mg
of ketamine. No local anesthesia was performed according to
French military guidelines. The otolaryngologist conducted a
bedside surgical technique employing a “scalpelbougietube”
method, in about 3 minutes, with no immediate complication.
4
This was further compounded by a right lateral zone III An endotracheal tube was cut to a smaller length and carefully
wound, a comminuted fracture of the anterior mandible, frac secured in place before medical evacuation.
tured teeth, and active bleeding in the mouth (Figure 2). He
was dyspneic on presentation with an open right chest wound Bleeding control was ensured by a cervical compressive pack
but did not appear to have tension pneumothorax physiology ing with QuikClot Combat Gauze (https://quikclot.com/) and
(Figure 2). The Glasgow Coma Scale score was 13 (eye 4, ver a facial dressing to close the mandibular symphysis fracture
bal 4, motor 5). He was confused, agitated and diaphoretic. (Figure 3). As he desaturated before the cricothyrotomy, a
His heart rate was 140 beats per minute with a systolic blood needle thoracostomy was performed and found to be negative
pressure of 120mmHg, in Class 3 shock. Oxygen saturation for tension pneumothorax. After the cricothyrotomy, oxygen
was 91%. The casualty was previously equipped at the front saturation was 96% and an extendedfocused assessment with
line with a peripheral venous line and an oxygen mask, hardly sonography for trauma (EFAST) was performed and showed
accepted by the patient. The otolaryngologist and nurse anes no hemopneumothorax. A threesided occlusive chest bandage
thetist managed the casualty at his arrival to the SLM, while was placed on the thoracic wound (Figure 3). The medical
other members of the team were dealing with other simultane evacuation team reported no complications en route and the
ous casualties. In an effort to maintain a patent airway, they patient was alive 2 days later.
removed the foreign body, suctioned the mouth, and attempted
hemorrhage control. With the inability to compress the facial
injuries to stop hemorrhage, concern for upper airway and FIGURE 3 Damage
possibly tracheal injury, and worsening mental status, the de control management
cision was made to perform an emergent surgical airway. with emergency
cricothyrotomy,
needle thoracostomy,
While it may have been physically possible to do an endotra three-sided occlusive
cheal intubation, there were several operational factors that chest bandage,
and cervicofacial
compressive packing.
Patient’s photograph.
Discussion
This case report illustrates the complexity and rapidity of
tactical decision making in an operational environment and
FIGURE 2 highlights the operation indications for emergent cricothyrot
Hemorrhagic
cervical wound omy in patients with severe cervicofacial injury. In this case,
and nonblowing, the main reason for the emergent airway was to avoid further
nonhemorrhagic chest management of a patient who required sedation and mechan
wound. ical ventilation in the context of a mass casualty event and
Patient’s photograph. poor medical resources/capabilities during evacuation. During
the Afghanistan and Iraq conflicts (2001–2011), traumatic
airway obstruction was responsible for 8% of fatalities caused
by penetrating injury to the face and neck anatomy; it was the
1,2
second leading cause of preventable mortality. These find
ings are similar, but slightly greater than that previously re
5
ported for airway obstruction mortality (1–2%). Historically,
airway obstruction is the third leading cause of potentially
Operational Consideration for Airway Management | 91