Page 68 - JSOM Summer 2022
P. 68
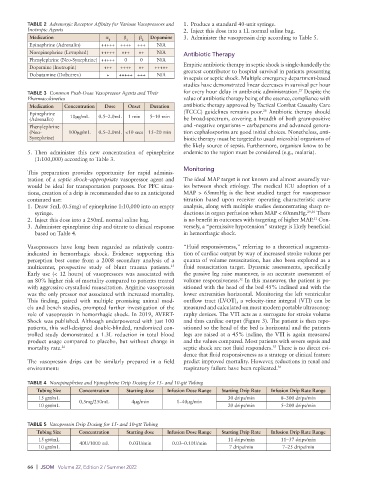
TABLE 2 Adrenergic Receptor Affinity for Various Vasopressors and 1. Produce a standard 40-unit syringe.
Inotropic Agents 2. Inject this dose into a 1L normal saline bag.
Medication α 1 β 1 β 2 Dopamine 3. Administer the vasopressin drip according to Table 5.
Epinephrine (Adrenalin) +++++ ++++ +++ N/A
Norepinephrine (Levophed) +++++ +++ ++ N/A Antibiotic Therapy
Phenylephrine (Neo-Synephrine) +++++ 0 0 N/A
Dopamine (Inotropin) +++ ++++ ++ +++++ Empiric antibiotic therapy in septic shock is single-handedly the
greatest contributor to hospital survival in patients presenting
Dobutamine (Dobutrex) + +++++ +++ N/A
in sepsis or septic shock. Multiple emergency department-based
studies have demonstrated linear decreases in survival per hour
27
TABLE 3 Common Push-Dose Vasopressor Agents and Their for every hour delay in antibiotic administration. Despite the
Pharmacokinetics value of antibiotic therapy being of the essence, compliance with
Medication Concentration Dose Onset Duration antibiotic therapy approved by Tactical Combat Casualty Care
28
Epinephrine 10mg/mL 0.5–2.0mL 1 min 5–10 min (TCCC) guidelines remains poor. Antibiotic therapy should
(Adrenalin) be broad-spectrum, covering a breadth of both gram- positive
Phenylephrine and -negative organisms – carbapenems and advanced genera-
(Neo- 100mg/mL 0.5–2.0mL <10 secs 15–20 min tion cephalosporins are good initial choices. Nonetheless, anti-
Synephrine) biotic therapy must be targeted to usual microbial organisms of
the likely source of sepsis. Furthermore, organism know to be
5. Then administer this new concentration of epinephrine endemic to the region must be considered (e.g., malaria).
(1:100,000) according to Table 3.
Monitoring
This preparation provides opportunity for rapid adminis-
tration of a septic shock–appropriate vasopressor agent and The ideal MAP target is not known and almost assuredly var-
would be ideal for transportation purposes. For PFC situa- ies between shock etiology. The medical ICU adoption of a
tions, creation of a drip is recommended due to an anticipated MAP > 65mmHg is the best studied target for vasopressor
continued use: titration based upon receiver operating characteristic curve
1. Draw 5mL (0.5mg) of epinephrine 1:10,000 into an empty analysis, along with multiple studies demonstrating sharp re-
syringe. ductions in organ perfusion when MAP < 60mmHg. 29,30 There
2. Inject this dose into a 250mL normal saline bag. is no benefit in outcomes with targeting of higher MAP. Con-
31
3. Administer epinephrine drip and titrate to clinical response versely, a “permissive hypotension” strategy is likely beneficial
based on Table 4. in hemorrhagic shock.
Vasopressors have long been regarded as relatively contra- “Fluid responsiveness,” referring to a theoretical augmenta-
indicated in hemorrhagic shock. Evidence supporting this tion of cardiac output by way of increased stroke volume per
perception best come from a 2008 secondary analysis of a quanta of volume resuscitation, has also been explored as a
multicenter, prospective study of blunt trauma patients. fluid resuscitation target. Dynamic assessments, specifically
25
Early use (< 12 hours) of vasopressors was associated with the passive leg raise maneuver, is an accurate assessment of
an 80% higher risk of mortality compared to patients treated volume responsiveness. In this maneuver, the patient is po-
32
with aggressive crystalloid resuscitation. Arginine vasopressin sitioned with the head of the bed 45% inclined and with the
was the only pressor not associated with increased mortality. lower extremities horizontal. Monitoring the left ventricular
This finding, paired with multiple promising animal mod- outflow tract (LVOT), a velocity-time integral (VTI) can be
els and bench studies, prompted further investigation of the measured and calculated on most modern portable ultrasonog-
role of vasopressin in hemorrhagic shock. In 2019, AVERT- raphy devices. The VTI acts as a surrogate for stroke volume
Shock was published. Although underpowered with just 100 and thus cardiac output (Figure 3). The patient is then repo-
patients, this well-designed double-blinded, randomized con- sitioned so the head of the bed is horizontal and the patients
trolled study demonstrated a 1.3L reduction in total blood legs are raised at a 45% incline, the VTI is again measured
product usage compared to placebo, but without change in and the values compared. Most patients with severe sepsis and
mortality rate. 26 septic shock are not fluid responders. There is no direct evi-
33
dence that fluid responsiveness as a strategy or clinical feature
The vasopressin drips can be similarly prepared in a field predict improved mortality. However, reductions in renal and
environment: respiratory failure have been replicated. 34
TABLE 4 Norepinephrine and Epinephrine Drip Dosing for 15- and 10-gtt Tubing
Tubing Size Concentration Starting dose Infusion Dose Range Starting Drip Rate Infusion Drip Rate Range
15 gtt/mL 0.5mg/250mL 4mg/min 1–40mg/min 30 drips/min 8–300 drips/min
10 gtt/mL 20 drips/min 5–200 drips/min
TABLE 5 Vasopressin Drip Dosing for 15- and 10-gtt Tubing
Tubing Size Concentration Starting dose Infusion Dose Range Starting Drip Rate Infusion Drip Rate Range
15 gtt/mL 40U/1000 mL 0.03U/min 0.03–0.10U/min 11 drips/min 11–37 drips/min
10 gtt/mL 7 drips/min 7–25 drips/min
66 | JSOM Volume 22, Edition 2 / Summer 2022