Page 73 - JSOM Summer 2022
P. 73
40
Acute or chronically anemic patients can present with a spec- limiting laboratory evaluation. Furthermore, in the setting
trum of symptoms, including dyspnea, weakness, fatigue, ir- of acute hemorrhage, initial testing may not demonstrate ane-
ritability, and headache, and most will not demonstrate any mia; therefore, repeat testing should be performed as indicated
1
visible evidence of active bleeding. 1–3,9,22 Many symptoms may with vital sign changes or following resuscitation measures. If
not manifest until hemoglobin levels fall below 7g/dL, given finger prick samples are used for point-of-care testing, medics
potential compensatory mechanisms, although there is sparse must remember that inaccuracies may occur because of de-
literature to directly correlate laboratory values and symptom creased capillary flow in cold or shock patients, or simple di-
onset. 1–3,20 Patients with chronic anemia may have significantly lution from interstitial fluid shifts. 41
lower hemoglobin levels with only mild symptoms, given grad-
ual rates of decline and ongoing adaptations. Other indices found on traditional laboratory evaluation, such
as hematocrit and RBC values, are derived from the hemo-
Initial findings of the acutely anemic patient may reveal he- globin concentration. 1,3,42 If available, this information can
modynamic instability, including hypotension, tachycardia, further characterize the anemia and help narrow its etiology,
tachypnea, and even hypoxemia. 1,20,26,27 The presence of fever primarily through the use of RDW and MCV. The MCV can
and considerations of anemia should prompt concerns for ma- help delineate anemia between microcytic, normocytic, and
laria in endemic regions, other infections, or such acute he- macrocytic classifications, thus narrowing etiologies (Table 2).
39
molytic anemias as DIC, HUS, or TTP. Additional signs and Overlap can occur between these groups, especially with
symptoms include decreased urine output, increased thirst, and iron-deficiency anemia (IDA). Although MCV values may not
altered mental status. Vital sign changes in anemia are incon- be available in an austere setting, differential diagnoses based
sistent and can change with patient demographics (primarily on these levels are discussed here for further consideration in
age), as well as possible comorbidities and medication usage. the setting of the atraumatic anemia patient in an austere set-
Pediatric patients may have delayed vital sign changes. 1,20 ting. Despite these expected limitations, the traditional differ-
Older patients do not consistently demonstrate compensatory ential for causes of anemia will be briefly discussed.
responses, and the use of such medications as beta-blockers
may prevent tachycardia. 1,6,20 Outward findings may include TABLE 2 Differential for Anemia by Mean Corpuscular Volume
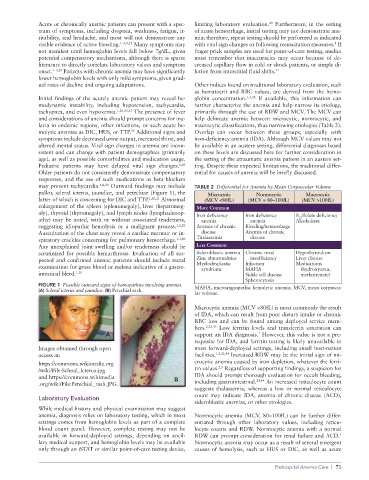
pallor, scleral icterus, jaundice, and petechiae (Figure 1), the Microcytic Normocytic Macrocytic
latter of which is concerning for DIC and TTP. 1,20,21 Abnormal (MCV <80fL) (MCV = 80–100fL) (MCV >100fL)
enlargement of the spleen (splenomegaly), liver (hepatomeg- More Common
aly), thyroid (thyromegaly), and lymph nodes (lymphadenop- Iron deficiency Iron deficiency B /folate deficiency
12
athy) may be noted, with or without associated tenderness, anemia anemia Alcoholism
suggesting idiopathic hemolysis or a malignant process. 1,2,20 Anemia of chronic Bleeding/hemorrhage
Auscultation of the chest may reveal a cardiac murmur or in- disease Anemia of chronic
spiratory crackles concerning for pulmonary hemorrhage. 1,3,20 Thalassemia disease
Any unexplained joint swelling and/or tenderness should be Less Common
scrutinized for possible hemarthrosis. Evaluation of all sus- Sideroblastic anemia Chronic renal Hypothyroidism
pected and confirmed anemic patients should include rectal Zinc abnormalities insufficiency Liver disease
examination for gross blood or melena indicative of a gastro- Myelodysplastic Infection Medications
syndrome
MAHA
(hydroxyurea,
intestinal bleed. 1,20 Sickle cell disease methotrexate)
Spherocytosis
FIGURE 1 Possible outward signs of hemopathies involving anemia. MAHA, microangiopathic hemolytic anemia; MCV, mean corpuscu-
(A) Scleral icterus and jaundice. (B) Petechial rash.
lar volume.
Microcytic anemia (MCV <80fL) is most commonly the result
of IDA, which can result from poor dietary intake or chronic
RBC loss and can be found among deployed service mem-
bers. 2,22,43 Low ferritin levels and transferrin saturation can
1
A support an IDA diagnosis. However, this value is not a pre-
requisite for IDA, and ferritin testing is likely unavailable in
Images obtained through open most forward-deployed settings, including small host-nation
access at: facilities. 1,2,22,44 Increased RDW may be the initial sign of mi-
https://commons.wikimedia.org crocytic anemia caused by iron depletion, whatever the ferri-
2,3
/wiki/File:Scleral_Icterus.jpg tin values. Regardless of supporting findings, a suspicion for
and https://commons.wikimedia B IDA should prompt thorough evaluation for occult bleeding,
.org/wiki/File:Petechial_rash.JPG. including gastrointestinal. 20,44 An increased reticulocyte count
suggests thalassemia, whereas a low or normal reticulocyte
count may indicate IDA, anemia of chronic disease (ACD),
Laboratory Evaluation
sideroblastic anemias, or other etiologies.
While medical history and physical examination may suggest
anemia, diagnosis relies on laboratory testing, which in most Normocytic anemia (MCV, 80–100fL) can be further differ-
settings comes from hemoglobin levels as part of a complete entiated through other laboratory values, including reticu-
blood count panel. However, complete testing may not be locyte counts and RDW. Normocytic anemia with a normal
available in forward-deployed settings, depending on ancil- RDW can prompt consideration for renal failure and ACD.
1
lary medical support, and hemoglobin levels may be available Normocytic anemia may occur as a result of several emergent
only through an iSTAT or similar point-of-care testing device, causes of hemolysis, such as HUS or DIC, as well as acute
Prehospital Anemia Care | 71