Page 65 - JSOM Summer 2022
P. 65
Shock and Vasopressors
2
1
Peter Lampman *; Kyle Kennington ; Seth M. Assar, MD 3
ABSTRACT
Shock is a life-threatening condition carrying a high mortality Presentation
rate when untreated. The consequences of shock are cellular
and meta bolic derangements, which are initially reversible. The The diagnosis of shock considers clinical, hemodynamic, and
authors present the case of a Servicemember who sustained biochemical features and cannot be established by a specific
mortar shrapnel wounds that resulted in shock. parameter. Clinical features common to shock include tachy-
cardia, hypotension, tachypnea, altered mental status, oliguria,
Keywords: shock; homeostasis; critical care and a spectrum of skin changes (cold to warm, pale to flushed)
dependent on etiology. Tachycardia is typically an early com-
pensatory mechanism to provide perfusion in shock states. It
is the common precursor to frank hypotension, which occurs
Introduction in most shock patients. The inverse and converse statements
are not true: an absence of hypotension does not exclude ac-
“. . . shock is a lack of homeostasis and without homeo- tive shock and the presence of hypotension does not indicate
stasis the patient does not survive.” shock. Tachypnea is another compensatory mechanism indic-
Walter B. Cannon, United States ative of the presence of an insidious acute metabolic acidosis.
Army Medical Corps (1918)
Often referred to as one of the “windows to the body,” the skin
and mucosal surfaces often reveal histologic derangements of
Shock is a life-threatening condition characterized by cellular
and tissue hypoxia resulting from circulatory failure-associ- shock. The severe peripheral vasoconstriction characteristic of
ated hypoperfusion. The consequences of shock are cellular cardiogenic shock may result in cold and pale skin. Alterna-
and metabolic derangements, which are initially reversible. tively, peripheral shunting in septic shock may leave the skin
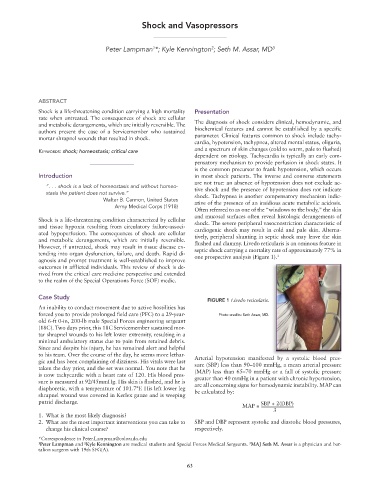
However, if untreated, shock may result in tissue disease ex- flushed and clammy. Livedo reticularis is an ominous feature in
tending into organ dysfunction, failure, and death. Rapid di- septic shock carrying a mortality rate of approximately 77% in
1
agnosis and prompt treatment is well-established to improve one prospective analysis (Figure 1).
outcomes in afflicted individuals. This review of shock is de-
rived from the critical care medicine perspective and extended
to the realm of the Special Operations Force (SOF) medic.
Case Study
FIGURE 1 Livedo reticularis.
An inability to conduct movement due to active hostilities has
forced you to provide prolonged field care (PFC) to a 29-year- Photo credits: Seth Assar, MD.
old 6-ft 0-in, 200-lb male Special Forces engineering sergeant
(18C). Two days prior, this 18C Servicemember sustained mor-
tar shrapnel wounds to his left lower extremity, resulting in a
minimal ambulatory status due to pain from retained debris.
Since and despite his injury, he has remained alert and helpful
to his team. Over the course of the day, he seems more lethar-
gic and has been complaining of dizziness. His vitals were last Arterial hypotension manifested by a systolic blood pres-
taken the day prior, and the set was normal. You note that he sure (SBP) less than 90–100 mmHg, a mean arterial pressure
is now tachycardic with a heart rate of 120. His blood pres- (MAP) less than 65–70 mmHg or a fall of systolic pressure
sure is measured at 92/45mmHg. His skin is flushed, and he is greater than 40 mmHg in a patient with chronic hypertension,
diaphoretic, with a temperature of 101.7°F. His left lower leg are all concerning signs for hemodynamic instability. MAP can
shrapnel wound was covered in Kerlex gauze and is weeping be calculated by:
putrid discharge. SBP + 2(DBP)
MAP =
3
1. What is the most likely diagnosis?
2. What are the most important interventions you can take to SBP and DBP represent systolic and diastolic blood pressures,
change his clinical course? respectively.
*Correspondence to Peter.Lampman@colorado.edu
3
1 Peter Lampman and Kyle Kennington are medical students and Special Forces Medical Sergeants. MAJ Seth M. Assar is a physician and bat-
2
talion surgeon with 19th SFG(A).
63