Page 94 - JSOM Winter 2021
P. 94
Stratifying sites according to flow rate is useful when high- There are substantial data that support using an IO line when
volume resuscitation is required. As previously discussed, peripheral IV access is not attainable for various reasons.
sternal and humoral sites have distinct flow rate advantages. However, in our opinion, there is no formal stratification to
Consistent with Wolf’s law, iliac crest access would also have a help determine preferential location for access placement. The
theoretical advantage. Due to the iliac crest being non–weight iliac crest has some unique advantages compared with other
bearing, density and flow resistance are relatively low. This sites, such as site availability, potentially better flow rate, ease
suggests flow rates would be similar to sternal IO flow rates. of insertion, and workspace utilization.
More devoted studies would be required to confirm this. Cer-
tainly, tibial access consistently lags regarding this metric. Conclusion
This is the first report of a whole blood transfusion through an
Anatomic differences among the possible sites are important to iliac crest IO for hemorrhagic shock in a military prehospital
consider. The iliac crest has a relatively wide medullary cavity setting. Based on our experience, the possibility of needing to
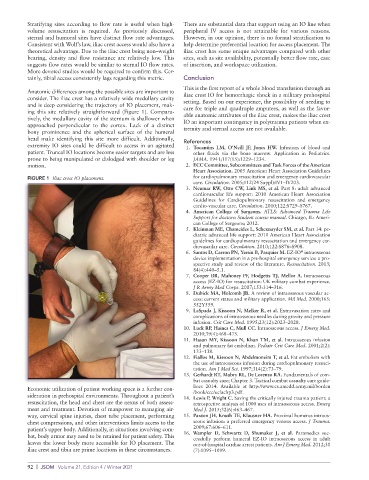
and is deep considering the trajectory of IO placement, mak- care for triple and quadruple amputees, as well as the favor-
ing this site relatively straightforward (Figure 1). Compara- able anatomic attributes of the iliac crest, makes the iliac crest
tively, the medullary cavity of the sternum is shallower when IO an important contingency in polytrauma patients when ex-
approached perpendicular to the cortex. Lack of a distinct tremity and sternal access are not available.
bony prominence and the spherical surface of the humeral
head make identifying this site more difficult. Additionally,
extremity IO sites could be difficult to access in an agitated References
1. Tocantins LM, O’Neill JF, Jones HW. Infusions of blood and
patient. Truncal IO locations become easier targets and are less other fluids via the bone marrow. Application in Pediatrics.
prone to being manipulated or dislodged with shoulder or leg JAMA. 1941;117(15):1229–1234.
motion. 2. ECC Committee, Subcommittees and Task Forces of the American
Heart Association. 2005 American Heart Association Guidelines
FIGURE 1 Iliac crest IO placement. for cardiopulmonary resuscitation and emergency cardiovascular
care. Circulation. 2005;112(24 Suppl):IV1–IV203.
3. Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced
cardiovascular life support: 2010 American Heart Association
Guidelines for Cardiopulmonary resuscitation and emergency
cardio-vascular care. Circulation. 2010;122:S729–S767.
4. American College of Surgeons. ATLS: Advanced Trauma Life
Support for doctors: Student course manual. Chicago, IL: Ameri-
can College of Surgeons; 2012.
5. Kleinman ME, Chameides L, Schexnayder SM, et al. Part 14: pe-
diatric advanced life support: 2010 American Heart Association
guidelines for cardiopulmonary resuscitation and emergency car-
diovascular care. Circulation. 2010;122:S876–S908.
6. Santos D, Carron PN, Yersin B, Pasquier M. EZ-IO intraosseous
®
device implementation in a pre-hospital emergency service: a pro-
spective study and review of the literature. Resuscitation. 2013;
84(4):440–5.1.
7. Cooper BR, Mahoney PF, Hodgetts TJ, Mellor A. Intraosseous
access (EZ-IO) for resuscitation: UK military combat experience.
J R Army Med Corps. 2007;153:314–316.
8. Dubick MA, Holcomb JB. A review of intraosseous vascular ac-
cess: current status and military application. Mil Med. 2000;165:
552Y559.
9. LaSpada J, Kissoon N, Melker R, et al. Extravasation rates and
complications of intraosseous needles during gravity and pressure
infusion. Crit Care Med. 1995;23(12):2023–2028.
10. Luck RP, Haines C, Mull CC. Intraosseous access. J Emerg Med.
2010;39(4):468–475.
11. Hasan MY, Kissoon N, Khan TM, et al. Intraosseous infusion
and pulmonary fat embolism. Pediatr Crit Care Med. 2001;2(2):
133–138.
12. Fiallos M, Kissoon N, Abdelmoneim T, et al. Fat embolism with
the use of intraosseous infusion during cardiopulmonary resusci-
tation. Am J Med Sci. 1997;314(2):73–79.
13. Gerhardt RT, Mabry RL, De Lorenzo RA. Fundamentals of com-
bat casualty care; Chapter 3. Tactical combat casualty care guide-
Economic utilization of patient working space is a further con- lines 2014. Available at http://www.cs.amedd.army.mil/borden
/book/ccc/uclachp3.pdf.
sideration in prehospital environments. Throughout a patient’s 14. Lewis P, Wright C. Saving the critically injured trauma patient: a
resuscitation, the head and chest are the nexus of both assess- retrospective analysis of 1000 uses of intraosseous access. Emerg
ment and treatment. Devotion of manpower to managing air- Med J. 2015;32(6):463–467.
way, cervical spine injuries, chest tube placement, performing 15. Paxton JH, Knuth TE, Klausner HA. Proximal humerus intraos-
chest compressions, and other interventions limits access to the seous infusion: a preferred emergency venous access. J Trauma.
patient’s upper body. Additionally, in situations involving com- 2009;67:606–611.
bat, body armor may need to be retained for patient safety. This 16. Wampler D, Schwartz D, Shumaker J, et al. Paramedics suc-
cessfully perform humeral EZ-IO intraosseous access in adult
leaves the lower body more accessible for IO placement. The out-of-hospital cardiac arrest patients. Am J Emerg Med. 2012;30
iliac crest and tibia are prime locations in these circumstances. (7):1095–1099.
92 | JSOM Volume 21, Edition 4 / Winter 2021