Page 74 - JSOM Winter 2021
P. 74
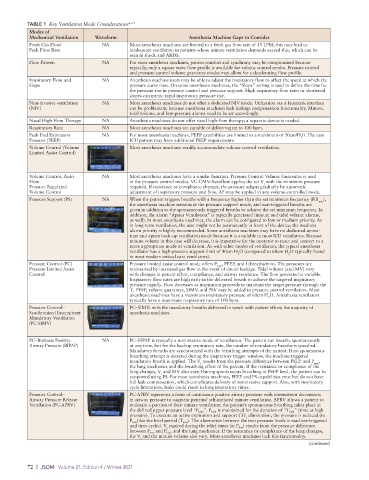
TABLE 1 Key Ventilation Mode Considerations 6–11
Modes of
Mechanical Ventilation Waveform Anesthesia Machine Gaps to Consider
Fresh Gas Flow/ NA Most anesthesia machines are limited to a fresh gas flow rate of 15 LPM; this may lead to
Peak Flow Rate inadequate ventilation in patients whose minute ventilation demands exceed this, which can be
seen in shock and ARDS.
Flow Pattern NA For most anesthesia machines, patient comfort and synchrony may be compromised because
typically, only a square wave flow profile is available for volume control modes. Pressure control
and pressure control volume guarantee modes may allow for a decelerating flow profile.
Inspiratory Flow and NA Anesthesia machine users may be able to adjust the inspiratory flow to affect the speed at which the
Slope pressure curve rises. On some anesthesia machines, the “Slope” setting is used to define the time for
the pressure rise in pressure control and pressure support. High inspiratory flow rates or shortened
slopes can mimic rapid inspiratory pressure rise.
Non-invasive ventilation NA Most anesthesia machines do not offer a dedicated NIV mode. Utilization via a facemask interface
(NIV) can be problematic because anesthesia machines lack leakage compensation functionality. Minute,
tidal volume, and low-pressure alarms need to be set accordingly.
Nasal High-Flow Therapy NA Anesthesia machines do not offer nasal high-flow therapy; a separate device is needed.
Respiratory Rate NA Most anesthesia machines are capable of delivering up to 100 bpm.
Peak End Expiratory NA For most anesthesia machines, PEEP capabilities are limited to a maximum of 30cm/H 0. The rare
2
Pressure (PEEP) ICU patient may have additional PEEP requirements.
Volume Control (Volume Most anesthesia machines readily accommodate volume control ventilation.
Limited Assist Control)
Volume Control, Auto NA Most anesthesia machines have a similar function. Pressure Control Volume Guarantee is used
Flow in the pressure control modes. VC-CMV-Autoflow applies the set V with the minimum pressure
t
Pressure Regulated required. If resistance or compliance changes, the pressure adapts gradually by automatic
Volume Control adjustment of inspiratory pressure and flow. AF may be applied in any volume-controlled mode.
Pressure Support (PS) NA When the patient triggers breaths with a frequency higher than the set minimum frequency (RR ),
min
the anesthesia machine remains in the pressure support mode, and non-triggered breaths are
given in addition to the spontaneously triggered breaths to achieve the set minimum frequency. In
addition, the alarm “Apnea Ventilation” is typically generated (minute and tidal volume alarms,
as well). In most anesthesia machines, the alarm can be configured to low or medium priority. As
in long-term ventilation, the user might not be permanently in front of the device; the medium
alarm priority is highly recommended. Some anesthesia machines may have no dedicated apnea-
time and apnea back-up ventilation mode because it is available in most ICU ventilators. Because
minute volume in this case will decrease, it is imperative for the operator to react and convert to a
more appropriate mode of ventilation. As with other modes of ventilation, the typical anesthesia
ventilator has a high-pressure support limit of 40cm H O (compared to 60cm H O typically found
2
2
in most modern critical care ventilators).
Pressure Control (PC) Pressure limited assist control mode offers P insp , PEEP, and f (breaths/min). The pressures are
Pressure Limited Assist maintained by increased gas flow in the event of circuit leakage. Tidal volume (and MV) vary
Control with changes in patient effort, compliance, and airway resistance. The flow generated is variable.
Inspiratory flow rates are high early in the delivered breath to achieve the targeted inspiratory
pressure rapidly. Flow decreases as inspiration proceeds to maintain the target pressure through the
T. PEEP, volume guarantee, SIMV, and PSV may be added to pressure control ventilation. Most
i
anesthesia machines have a maximum inspiratory pressure of 60cm H O. Anesthesia ventilators
2
typically have a maximum respiratory rate of 100 bpm.
Pressure Control– PC–SIMV: with the mandatory breaths delivered in synch with patient effort; the majority of
Synchronized Intermittent anesthesia machines
Mandatory Ventilation
(PC-SIMV)
PC–Biphasic Positive NA PC–BIPAP is typically a noninvasive mode of ventilation. The patient can breathe spontaneously
Airway Pressure (BIPAP) at any time, but for the backup respiratory rate, the number of mandatory breaths is specified.
Mandatory breaths are synchronized with the breathing attempts of the patient. If no spontaneous
breathing attempt is detected during the inspiratory trigger window, the machine-triggered
mandatory breath is applied. The V results from the pressure difference between PEEP and P insp ,
t
the lung mechanics and the breathing effort of the patient. If the resistance or compliance of the
lung changes, V and MV also vary. During spontaneous breathing at PEEP level, the patient can be
t
supported using PS. For most anesthesia machines, PEEP and PS capabilities exist but do not have
full leak compensation, which complicates delivery of noninvasive support. Also, with inspiratory
cycle limitations, leaks could result in long inspiratory times.
Pressure Control– PC-APRV represents a form of continuous positive airway pressure with intermittent decrements
Airway Pressure Release in airway pressure to augment patients’ self-initiated minute ventilation. APRV allows a patient to
Ventilation (PC-APRV) maintain a portion of their minute ventilation; the patient’s spontaneous breathing takes place at
the defined upper pressure level “P high ”. P high is maintained for the duration of “T high ” (time at high
pressure). To execute an active expiration and support CO elimination, the pressure is reduced (to
2
P low ) for the brief period (T low ). The alternation between the two pressure levels is machine-triggered
and time-cycled. V expired during the relief times (at P low ) results from the pressure difference
t
between P low and P high and the lung mechanics. If the resistance or compliance of the lung changes,
the V and the minute volume also vary. Most anesthesia machines lack this functionality.
t
(continues)
72 | JSOM Volume 21, Edition 4 / Winter 2021