Page 36 - JSOM Spring 2021
P. 36
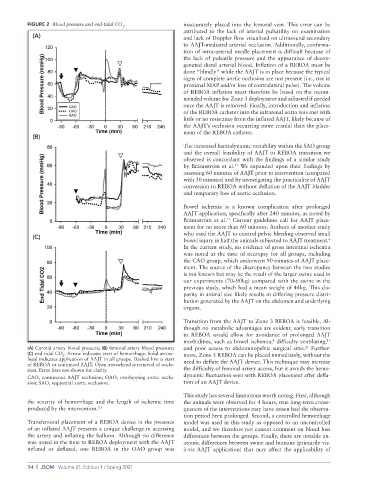
FIGURE 2 Blood pressure and end-tidal CO . inaccurately placed into the femoral vein. This error can be
2
attributed to the lack of arterial pulsatility on examination
(A) and lack of Doppler flow visualized on ultrasound secondary
to AAJT-mediated arterial occlusion. Additionally, confirma-
tion of intra-arterial needle placement is difficult because of
the lack of pulsatile pressure and the appearance of deoxy-
genated distal arterial blood. Inflation of a REBOA must be
done “blindly” while the AAJT is in place because the typical
signs of complete aortic occlusion are not present (i.e., rise in
proximal MAP and/or loss of contralateral pulse). The volume
of REBOA inflation must therefore be based on the recom-
mended volume for Zone 3 deployment and adjusted if needed
once the AAJT is removed. Finally, introduction and inflation
of the REBOA catheter into the infrarenal aorta was met with
little or no resistance from the inflated AAJT, likely because of
the AAJT’s occlusion occurring more cranial than the place-
ment of the REBOA catheter.
(B)
The increased hemodynamic variability within the SAO group
and the overall feasibility of AAJT to REBOA transition we
observed is concordant with the findings of a similar study
by Brännström et al. We expanded upon their findings by
21
assessing 60 minutes of AAJT prior to intervention (compared
with 30 minutes) and by investigating the practicality of AAJT
conversion to REBOA without deflation of the AAJT bladder
and temporary loss of aortic occlusion.
Bowel ischemia is a known complication after prolonged
AAJT application, specifically after 240 minutes, as noted by
Brännström et al. Current guidelines call for AAJT place-
13
ment for no more than 60 minutes. Authors of another study
who used the AAJT to control pelvic bleeding observed small
(C)
bowel injury in half the animals subjected to AAJT treatment.
6
In the current study, no evidence of gross intestinal ischemia
was noted at the time of necropsy for all groups, including
the CAO group, which underwent 90 minutes of AAJT place-
ment. The source of the discrepancy between the two studies
is not known but may be the result of the larger swine used in
our experiments (70–90kg) compared with the swine in the
previous study, which had a mean weight of 44kg. This dis-
parity in animal size likely results in differing pressure distri-
bution generated by the AAJT on the abdomen and underlying
organs.
Transition from the AAJT to Zone 3 REBOA is feasible. Al-
though no metabolic advantages are evident, early transition
to REBOA would allow for avoidance of prolonged AAJT
morbidities, such as bowel ischemia, difficulty ventilating,
6
11
(A) Carotid artery blood pressure; (B) femoral artery blood pressure; and poor access to abdominopelvic surgical sites. Further-
21
(C) end-tidal CO . Arrow indicates start of hemorrhage. Solid arrow- more, Zone 3 REBOA can be placed immediately, without the
2
head indicates application of AAJT in all groups. Dashed line is start need to deflate the AAJT device. This technique may increase
of REBOA or continued AAJT. Open arrowhead is removal of occlu-
sion. Error bars not shown for clarity. the difficulty of femoral artery access, but it avoids the hemo-
CAO, continuous AAJT occlusion; OAO, overlapping aortic occlu- dynamic fluctuation seen with REBOA placement after defla-
sion; SAO, sequential aortic occlusion. tion of an AAJT device.
This study has several limitations worth noting. First, although
the severity of hemorrhage and the length of ischemic time the animals were observed for 4 hours, true long-term conse-
produced by the intervention. 7,9 quences of the interventions may have arisen had the observa-
tion period been prolonged. Second, a controlled hemorrhage
Transfemoral placement of a REBOA device in the presence model was used in this study as opposed to an uncontrolled
of an inflated AAJT presents a unique challenge in accessing model, and we therefore not cannot comment on blood loss
the artery and inflating the balloon. Although no difference differences between the groups. Finally, there are notable an-
was noted in the time to REBOA deployment with the AAJT atomic differences between swine and humans (primarily vis-
inflated or deflated, one REBOA in the OAO group was à-vis AAJT application) that may affect the applicability of
34 | JSOM Volume 21, Edition 1 / Spring 2021