Page 118 - JSOM Spring 2021
P. 118
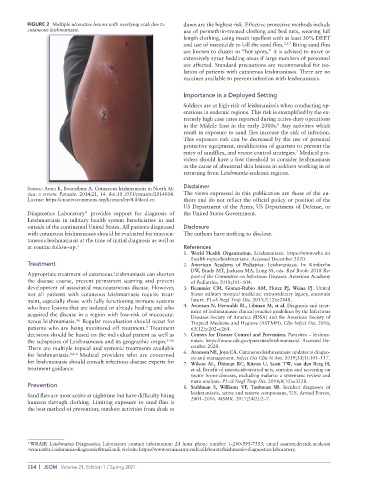
FIGURE 2 Multiple ulcerative lesions with overlying scab due to dawn are the highest risk. Effective protective methods include
cutaneous leishmaniasis. use of permethrin-treated clothing and bed nets, wearing full
length clothing, using insect repellent with at least 30% DEET
and use of insecticide to kill the sand flies. 2,5,7 Biting sand flies
are known to cluster in “hot spots,” it is advised to move or
extensively spray bedding areas if large numbers of personnel
are affected. Standard precautions are recommended for iso-
lation of patients with cutaneous leishmaniasis. There are no
vaccines available to prevent infection with leishmaniasis.
Importance in a Deployed Setting
Soldiers are at high-risk of leishmaniasis when conducting op-
erations in endemic regions. This risk is exemplified by the ex-
tremely high case rates reported during active-duty operations
in the Middle East in the early 2000s. Any activities which
8
result in exposure to sand flies increase the risk of infection.
This exposure risk can be decreased by the use of personal
protective equipment, modification of quarters to prevent the
entry of sandflies, and vector control strategies. Medical pro-
7
viders should have a low threshold to consider leishmaniasis
as the cause of abnormal skin lesions in soldiers working in or
returning from Leishmania-endemic regions.
Source: Aoun K, Bouratbine A. Cutaneous leishmaniasis in North Af- Disclaimer
rica: a review. Parasite. 2014;21, 14. doi:10.1051/parasite/2014014. The views expressed in this publication are those of the au-
License: https://creativecommons.org/licenses/by/4.0/deed.en thors and do not reflect the official policy or position of the
US Department of the Army, US Department of Defense, or
Diagnostics Laboratory* provides support for diagnosis of the United States Government.
Leishmaniasis in military health system beneficiaries in and
outside of the continental United States. All patients diagnosed Disclosure
with cutaneous leishmaniasis should be evaluated for mucocu- The authors have nothing to disclose.
taneous leishmaniasis at the time of initial diagnosis as well as
at routine follow-up. 4 References
1. World Health Organization. Leishmaniasis. https://www.who.int
/health-topics/leishmaniasis. Accessed December 2020.
Treatment 2. American Academy of Pediatrics. Leishmaniasis. In: Kimberlin
DW, Brady MT, Jackson MA, Long SS, eds. Red Book: 2018 Re-
Appropriate treatment of cutaneous leishmaniasis can shorten port of the Committee on Infectious Diseases. American Academy
the disease course, prevent permanent scarring and prevent of Pediatrics; 2018;501–504.
development of associated mucocutaneous disease. However, 3. Beaumier CM, Gomez-Rubio AM, Hotez PJ, Weina PJ. United
not all patients with cutaneous leishmaniasis require treat- States military tropical medicine: extraordinary legacy, uncertain
ment, especially those with fully functioning immune systems future. PLoS Negl Trop Dis. 2013;7(12):e2448.
who have lesions that are isolated or already healing and who 4. Aronson N, Herwaldt BL, Libman M, et al. Diagnosis and treat-
acquired the disease in a region with low-risk of mucocuta- ment of leishmaniasis: clinical practice guidelines by the Infectious
Diseases Society of America (IDSA) and the American Society of
neous leishmaniasis. Regular reevaluation should occur for Tropical Medicine and Hygiene (ASTMH). Clin Infect Dis. 2016;
3,6
patients who are being monitored off treatment. Treatment 63(12):e202–e264.
3
decisions should be based on the individual patient as well as 5. Centers for Disease Control and Prevention. Parasites – leishma-
the subspecies of Leishmaniasis and its geographic origin. 2–4,6 naisis. https://www.cdc.gov/parasites/leishmaniasis/. Accessed De-
There are multiple topical and systemic treatments available cember 2020.
for leishmaniasis. 2,4–6 Medical providers who are concerned 6. Aronson NE, Joya CA. Cutaneous leishmaniasis: updates in diagno-
sis and management. Infect Dis Clin N Am. 2019;33(1):101–117.
for leishmaniasis should consult infectious disease experts for 7. Wilson AL, Dhiman RC, Kitron U, Scott TW, van den Berg H,
treatment guidance. et al. Benefit of insecticide-treated nets, curtains and screening on
vector borne diseases, excluding malaria: a systematic review and
meta-analysis. PLoS Negl Trop Dis. 2014;8(10):e3228.
Prevention 8. Stahlman S, Williams VF, Taubman SB. Incident diagnoses of
Sand flies are most active at nighttime but have difficulty biting leishmaniasis, active and reserve components, U.S. Armed Forces,
humans through clothing. Limiting exposure to sand flies is 2001–2016. MSMR. 2017;24(2):2–7.
the best method of prevention; outdoor activities from dusk to
*WRAIR Leishmania Diagnostics Laboratory contact information: 24 hour phone number 1-240-595-7353; email usarmy.detrick.medcom
-wrair.mbx.leishmania-diagnostic@mail.mil; website https://www.wrair.army.mil/collaborate/leishmania-diagnostics-laboratory.
114 | JSOM Volume 21, Edition 1 / Spring 2021