Page 55 - JSOM Winter 2019
P. 55
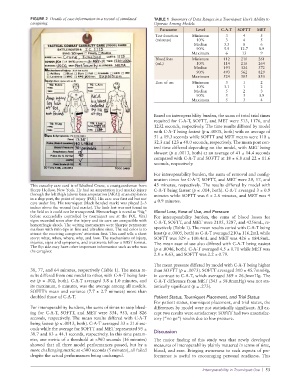
FIGURE 2 Details of case information in a record of simulated TABLE 1 Summary of Data Ranges in a Tourniquet User’s Ability to
caregiving. Operate Among Models
Parameter Level C-A-T SOFTT MET
Test duration Minimum 3 4 5
(minutes) 10% 3 4 5
Median 3.5 8 6
90% 5.9 12.7 8.9
Maximum 6 13 9
Blood loss Minimum 112 210 261
(mL) 10% 114 216 264
Median 193 324 372
90% 493 562 829
Maximum 524 585 853
Ease of use Minimum 3 1 2
10% 3.1 1 2
Median 5 2 3
90% 5 3 3.9
Maximum 5 3 4
Based on interoperability burden, the sums of total trial times
required for C-A-T, SOFTT, and MET were 513, 1176, and
1232 seconds, respectively. The time results differed by model
with C-A-T being fastest (p ≤ .0005, both) with an average of
51 ± 19.3 seconds while SOFTT and MET means were 118 ±
32.3 and 123 ± 40.0 seconds, respectively. The mean post con-
trol time differed depending on the model, with MET being
slowest (p ≤ .0013, both) at an average of 41 ± 14.4 seconds
compared with C-A-T and SOFTT at 18 ± 6.8 and 22 ± 11.6
seconds, respectively.
For interoperability burden, the sums of removal and config-
uration times for C-A-T, SOFTT, and MET were 29, 57, and
This casualty care card is of Ichabod Crane, a coastguardsman from 43 minutes, respectively. The results differed by model with
Sleepy Hollow, New York. He had an amputation (red marks) injury C-A-T being fastest (p ≤ .014, both). C-A-T averaged 3 ± 0.9
through the left thigh (above knee amputation [AKA]) at an explosion minutes while SOFTT was 6 ± 2.6 minutes, and MET was 4
in a ship port, the point of injury (POI). His care was first aid but not ± 0.9 minutes.
care under fire. His tourniquet (black banded mark) was placed 2–3
inches above the wound (red marks). The limb lost was not found in
the field so it could not be transported. Hemorrhage is noted as “big” Blood Loss, Ease of Use, and Pressure
before successfully controlled by tourniquet use at the POI. Vital For interoperability burden, the sums of blood losses for
signs recorded soon after the injury and its care are compatible with C-A-T, SOFTT, and MET were 2105, 3287, and 4256mL, re-
hemorrhagic shock. The writing instruments were Sharpie permanent
markers with twin-tips in fine and ultrafine sizes. The red color is to spectively (Table 1). The mean results varied with C-A-T being
attract the receiving caregivers’ attention first. This card tells a short least (p ≤ .0005, both) as C-A-T averaged 210 ± 116.2mL while
story: what, when, where, why, and how. The mechanisms of injury, SOFTT was 329 ± 100.4mL and MET was 426 ± 184.8mL.
injuries, signs and symptoms, and treatments follow a MIST format. The mean ease of use also differed with C-A-T being easiest
The flip side may have other important information such as who was (p ≤ .0046, both). C-A-T averaged 4.5 ± 0.71 while MET was
the caregiver.
2.8 ± 0.63, and SOFTT was 2.2 ± 0.79.
The mean pressure differed by model with C-A-T being higher
38, 77, and 64 minutes, respectively (Table 1). The mean re- than SOFTT (p = .0073). SOFTT averaged 310 ± 45.7mmHg,
sults differed from one model to other, with C-A-T being fast- in contrast to C-A-T, which averaged 369 ± 26.3mmHg. The
est (p ≤ .002, both). C-A-T averaged 3.8 ± 1.0 minutes, and C-A-T difference from MET (345 ± 58.0mmHg) was not sta-
its maximum, 6 minutes, was the average among all models. tistically significant (p = .273).
SOFTT’s mean and variance (7.7 ± 2.7 minutes) more than
doubled those of C-A-T. Patient Status, Tourniquet Placement, and Trial Status
For patient status, tourniquet placement, and trial status, the
For interoperability burdens, the sums of times to stop bleed- differences by model were not statistically significant. All ex-
ing for C-A-T, SOFTT, and MET were 334, 953, and 826 cept two results were satisfactory: SOFTT had two unsatisfac-
seconds, respectively. The mean results differed with C-A-T tory (“no go”) results due to low pressure.
being fastest (p ≤ .0013, both). C-A-T averaged 33 ± 21.6 sec-
onds while the average for SOFTT and MET represented 95 ± Discussion
38.7 and 83 ± 44.1 seconds, respectively. In this time param-
eter, one metric of a threshold at <960 seconds (16 minutes) The major finding of this study was that newly developed
showed that all three model performances passed, but by a measures of interoperability plainly mattered in terms of time,
more challenging metric at <300 seconds (5 minutes), all failed blood, and ease. Bringing awareness to such aspects of per-
despite the actual performances being unchanged. formance is useful to encouraging personal readiness. This
Interoperability in Tourniquet Use | 53