Page 81 - JSOM Summer 2019
P. 81
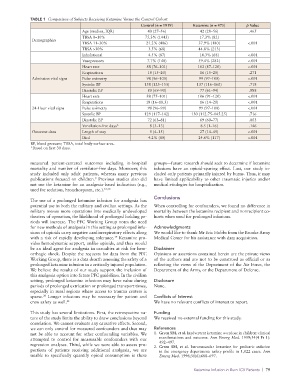
TABLE 1 Comparison of Subjects Receiving Ketamine Versus the Control Cohort
Control (n = 1919) Ketamine (n = 475) p Value
Age (median, IQR) 40 (27–56) 42 (28–56) .465
TBSA 0–10% 75.3% (1445) 17.3% (82)
Demographics
TBSA 11–30% 21.2% (406) 37.9% (180) <.001
TBSA >30% 3.5% (68) 44.8% (213)
Inhalational 4.5% (87) 14.3% (68) <.001
Vasopressors 7.7% (148) 59.4% (282) <.001
Heart rate 88 (76–101) 102 (87–120) <.001
Respirations 18 (15–20) 16 (15–20) .271
Admission vital signs Pulse oximetry 98 (96–100) 99 (97–100) <.001
Systolic BP 138 (123–153) 137 (116–160) .718
Diastolic BP 80 (69–90) 77 (61–94) .088
Heart rate 88 (75–101) 106 (91–120) <.001
Respirations 18 (16–18.5) 16 (14–20) <.001
24-Hour vital signs Pulse oximetry 98 (96–99) 99 (97–100) <.001
Systolic BP 129 (117–142) 130 (112.75–145.25) .716
Diastolic BP 72 (63–81) 69 (60–77) .003
Ventilation-free days* 8 (3–13) 8.5 (1–16) .146
Outcome data Length of stay 9 (4–15) 27 (14–49) <.001
Died 4.2% (80) 24.6% (117) <.001
BP, blood pressure; TBSA, total body surface area.
*Based on first 30 days.
measured patient-centered outcomes including in-hospital groups—future research should seek to determine if ketamine
mortality and number of ventilator-free days. Moreover, this infusions have an opioid-sparing effect. Last, our study in-
study included only adult patients, whereas many previous cluded only patients primarily injured by burns. Thus, it may
publications focused on children. Previous studies also did have limited applicability to other traumatic injuries and/or
9
not use the ketamine for an analgesia-based indication (e.g., medical etiologies for hospitalization.
used for sedation, bronchospasm, etc.). 16,18
Conclusions
The use of a prolonged ketamine infusion for analgesia has
potential use in both the military and civilian settings. As the When controlling for confounders, we found no difference in
military moves more operations into medically undeveloped mortality between the ketamine recipient and nonrecipient co-
theaters of operation, the likelihood of prolonged holding pe- horts when used for prolonged infusions.
riods will increase. The PFC Working Group notes the need
for new methods of analgesia in this setting as prolonged infu- Acknowledgments
sions of opioids carry negative cardiorespiratory effects along We would like to thank Mr Eric Hobbs from the Brooke Army
with a risk of rapidly developing tolerance. Ketamine pro- Medical Center for his assistance with data acquisition.
19
vides hemodynamic support, unlike opioids, and thus would
be an ideal agent for analgesia in casualties at risk for hem- Disclaimer
orrhagic shock. Despite the requests for data from the PFC Opinions or assertions contained herein are the private views
Working Group, there is a data dearth assessing the safety of a of the authors and are not to be construed as official or as
prolonged ketamine infusion in a critically injured population. reflecting the views of the Department of the Air Force, the
We believe the results of our study support the inclusion of Department of the Army, or the Department of Defense.
this analgesia option into future PFC guidelines. In the civilian
setting, prolonged ketamine infusions may have value during Disclosure
periods of prolonged extrication or prolonged transport times, None.
especially in rural regions where access to trauma centers is
sparse. Longer infusions may be necessary for patient and Conflicts of Interest
20
crew safety as well. 21 We have no relevant conflicts of interest to report.
This study has several limitations. First, the retrospective na- Funding
ture of the study limits the ability to draw conclusions beyond We received no external funding for this study.
correlation. We cannot evaluate any causative effects. Second,
we can only control for measured confounders and thus may References
not be able to account for other confounding variables. We 1. Green SM, et al. Inadvertent ketamine overdose in children: clinical
attempted to control for measurable confounders with our manifestations and outcome. Ann Emerg Med. 1999;34(4 Pt 1):
492–497.
regression analyses. Third, while we were able to assess pro- 2. Green SM, et al. Intramuscular ketamine for pediatric sedation
portions of patients receiving additional analgesia, we are in the emergency department: safety profile in 1,022 cases. Ann
unable to specifically quantify opioid consumption in these Emerg Med. 1998;31(6):688–697.
Ketamine Infusion in Burn ICU Patients | 79