Page 62 - JSOM Winter 2018
P. 62
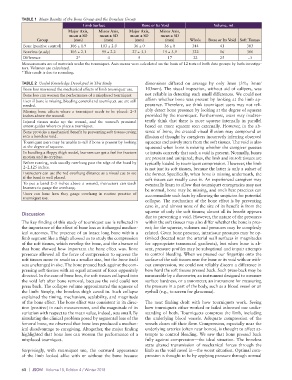
TABLE 1 Mean Results of the Bone Group and the Boneless Group
Limb Surface Bone or Its Void Volume, mL
Major Axis, Minor Axis, Major Axis, Minor Axis,
mean ± SD mean ± SD mean ± SD mean ± SD
Group (mm) (mm) (mm) (mm) Whole Bone or Its Void Soft Tissues
Bone (positive control) 106 ± 1.9 103 ± 2.0 36 ± 0 36 ± 0 344 41 303
Boneless (study) 103 ± 2.1 99 ± 2.2 27 ± 3.3 19 ± 3.9 322 16 306
Difference 2* 4 9 17 22 25 −3
Measurements are of materials under the tourniquet. Axis means were calculated on the basis of 12 tests of both data groups by both investiga-
tors. Volumes are calculated.
*This result is due to rounding.
TABLE 2 Useful Knowledge Developed in This Study dimensions differed on average by only 3mm (3%; 3mm/
Bone loss worsened the mechanical effects of limb tourniquet use. 103mm). The visual inspection, without aid of calipers, was
Bone loss can worsen the performance of a misplaced tourniquet. not reliable in detecting such small differences. We could not
Even if bone is missing, bleeding control and tourniquet use are still affirm whether bone was present by looking at the limb ap-
needed. pearance. Therefore, we think tourniquet users may not reli-
Missing bone affects where a tourniquet needs to be placed: 2–3 ably detect bone presence by looking at the degree of squeeze
inches above the wound. provided by the tourniquet. Furthermore, users may inadver-
Injured tissues make up the wound, and the wound’s proximal tently think that there is more squeeze internally in parallel
extent guides where to place a tourniquet. based on more squeeze seen externally. However, in the ab-
Bone provides a mechanical benefit by preventing soft tissues caving sence of bone, the created visual illusion may compound an
into a boneless void. illusion of thought by caregivers incorrectly inferring observed
Tourniquet users may be unable to tell if bone is present by looking squeezes exclusively stem from the soft tissues. The void is also
at the degree of squeeze. squeezed when bone is missing whether the caregiver guesses
In handling a floppy thigh model, learners can get a feel for fracture or intuits correctly that such a void is present. Normally, bones
motion and its crepitus. are present and uninjured; thus, the limb and its soft tissues are
Before turning, rods usually overhang past the edge of the band by typically loaded by tourniquet compression. However, the limb
2–2.125 inches. is not just its soft tissues, because the latter is only a subset of
Instructors can use the rod overhang distance as a visual cue to see the former. Specifically, when bone is missing underneath, the
if the band is well placed. soft tissues can readily cave in. An experienced caregiver may
To put a band 2–3 inches above a wound, instructors can teach eventually learn to allow that tourniquet emergencies may not
learners to gauge the overhang. be normal, bone may be missing, and one’s best practices can
Users can hone how they gauge overhang in routine practice of accommodate such facts by allowing the suspicion for potential
tourniquet use.
collapse. The mechanism of the bone effect is by preventing
cave in, and almost none of the size of its benefit is from the
squeeze of only the soft tissues; almost all its benefit appears
Discussion
due to preventing a void. However, the nature of the pressures
The key finding of this study of tourniquet use is reflected in within the soft tissues may also differ whether the bone is pres-
the importance of the effect of bone loss as it changed mechan- ent; for the squeeze, volumes and pressures may be complexly
ical outcomes. The presence of an intact long bone within a related. Given bone presence, intratissue pressures may be op-
limb segment like a thigh allowed us to study the compression timized (located near the arterial wall surfaces in magnitudes
of the soft tissues, which envelop the bone, and the absence of for appropriate transmural gradients), but when bone is ab-
that bone showed how important the bone effect was. Bone sent, pressure profiles may be suboptimal and impair attempts
presence allowed all the force of compression to squeeze the to control bleeding. When we pressed our fingertips onto the
soft tissues more to result in a smaller size, but the bone itself surface of the soft tissues near the bone or its void with or with-
was unchanged in size. The bone pressed back against the com- out compression, we could not reliably discern a difference in
pressing soft tissues with an equal amount of force oppositely how hard the soft tissues pressed back. Such press-back may be
directed. In the case of bone loss, the soft tissues collapsed into measurable by a durometer, an instrument designed to measure
the void left after bone removal, because the void could not surface hardness, or a tonometer, an instrument for measuring
press back. The collapse volume approximated the squeeze of the pressure in a part of the body, such as a blood vessel or an
the limb: Simply, the boneless thigh caved in. Such collapse eyeball (e.g., to screen for glaucoma).
explained the timing, mechanism, scalability, and magnitude
of the bone effect. The bone effect was consistent in its direc- The next finding dealt with how tourniquets work. Seeing
tion (positive) in each measurement, and the magnitude of its how tourniquets either worked or failed informed our under-
variation with respect to the mean value, indeed, was small. By standing of both. Tourniquets compress the limb, including
simulating the clinical problem posed by segmental loss of the the underlying blood vessels. Adequate compression of the
femoral bone, we observed that bone loss produced a mechan- vessels closes off their flow. Compression, especially near the
ical disadvantage to caregiving. Altogether, the major finding underlying arteries (often near bones), is thought to affect at-
highlighted that bone loss can worsen the performance of a tempts to control bleeding. We saw that bone pressed back
misplaced tourniquet. fully against compression—the ideal situation. The boneless
state altered transmission of mechanical forces through the
Surprisingly, with tourniquet use, the outward appearance limb as the void caved in—the worst situation. Optimal com-
of the limb looked alike with or without the bone because pression is thought to be by applying pressure through normal
60 | JSOM Volume 18, Edition 4 / Winter 2018