Page 23 - JSOM Winter 2018
P. 23
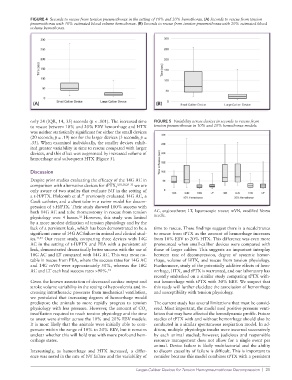
FIGURE 4 Seconds to rescue from tension pneumothorax in the setting of 10% and 20% hemothorax. (A) Seconds to rescue from tension
pneumothorax with 10% estimated blood volume hemothorax. (B) Seconds to rescue from tension pneumothorax with 20% estimated blood
volume hemothorax.
(A) (B)
only 24 (IQR, 14, 35) seconds (p < .001). The increased time FIGURE 5 Variability across devices in seconds to rescue from
to rescue between 10% and 20% EBV hemorrhage and HTX tension pneumothorax in 10% and 20% hemothorax models.
was neither statistically significant for either the small devices
(20 seconds; p = .19) nor for the larger devices (3 seconds; p =
.33). When examined individually, the smaller devices exhib-
ited greater variability in time to rescue compared with larger
devices, and this effect was augmented by increased volume of
hemorrhage and subsequent HTX (Figure 5).
Discussion
Despite prior studies evaluating the efficacy of the 14G AC in
comparison with alternative devices for tPTX, 9,10,18,29–31 we are
only aware of two studies that evaluate NT in the setting of
a t-H/PTX. Holcomb et al. previously evaluated 14G AC, a
32
Cook catheter, and a chest tube in a swine model for decom-
pression of t-H/PTX. Their study showed 100% success with
both 14G AC and tube thoracostomy in rescue from tension AC, angiocatheter; LT, laparoscopic trocar; mVN, modified Veress
physiology over 4 hours. However, this study was limited needle.
32
by a more modest definition of tension physiology and by the
lack of a persistent leak, which has been demonstrated to be a time to rescue. These findings suggest there is a recalcitrance
significant cause of 14G AC failure in animal and clinical stud- to rescue from tPTX as the amount of hemorrhage increases
ies. 11,25 Our recent study, comparing three devices with 14G from 10% EBV to 20% HTX. This difference was even more
AC in the setting of t-H/PTX and PEA with a persistent air pronounced when small-caliber devices were compared with
leak, demonstrated dramatically better success with the use of those of larger caliber. This suggests an important interplay
10G AC and LT compared with 14G AC. This was most no- between rate of decompression, degree of systemic hemor-
table in rescue from PEA, where the success rates for 14G AC rhage, volume of HTX, and rescue from tension physiology.
and 14G mVN were approximately 50%, whereas the 10G Furthermore, study of the potentially additive effects of hem-
AC and LT each had success rates >90%. 14 orrhage, HTX, and tPTX is warranted, and our laboratory has
recently embarked on a similar study comparing tPTX with-
Given the known association of decreased cardiac output and out hemorrhage with tPTX with 30% EBV. We suspect that
stroke volume variability in the setting of hypovolemia and in- this study will further elucidate the association of hemorrhage
creasing intrathoracic pressures from mechanical ventilation, and susceptibility with tension physiology.
we postulated that increasing degrees of hemorrhage would
predispose the animals to more rapidly progress to tension The current study has several limitations that must be consid-
physiology with less pressure. However, the amount of CO ered. Most important, the model used positive-pressure venti-
2
insufflation required to reach tension physiology and the time lation that may have affected the hemodynamic profile. Future
to onset were similar across the 10% and 20% EBV models. studies of tPTX with and without hemorrhage should also be
It is most likely that the animals were initially able to com- conducted in a similar spontaneous respiration model. In ad-
pensate within the range of 10% to 20% EBV, but it remains dition, multiple physiologic insults were incurred successively
unclear whether this will hold true with more profound hem- by each animal studied; however, judicious and responsible
orrhage states. resource management does not allow for a single event per
animal. Device failure is likely multifactorial and the ability
Interestingly, as hemorrhage and HTX increased, a differ- to discern causality of failure is difficult. This is important to
ence was noted in the rate of NT failure and the variability of consider because this model combines tPTX with a persistent
Larger-Caliber Devices for Tension Hemopneumothorax Decompression | 21