Page 38 - JSOM Fall 2018
P. 38
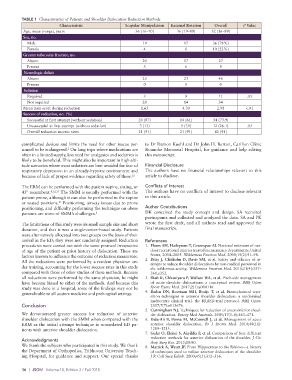
TABLE 1 Characteristics of Patients and Shoulder Dislocation Reduction Methods
Characteristic Scapular Manipulation External Rotation Overall P Value
Age, mean (range), years 36 (16–70) 36 (19–89) 32 (16–89)
Sex, no.
Male 19 17 36 (78%)
Female 4 6 10 (22%)
Greater tuberosity fracture, no.
Absent 20 17 27
Present 3 6 9
Neurologic deficit
Absent 23 23 46
Present 0 0 0
Sedation
Required 3 9 11 .05
Not required 20 14 34
Mean pain score during reduction 1.65 4.30 2.98 <.01
Success of reduction, no. (%)
Successful at first attempt (without sedation) 20 (87) 14 (61) 34 (73.9)
Unsuccessful at first attempt (without sedation) 3 (13) 9 (39) 12 (26.1) .05
Overall reduction success rates 21 (91) 21 (91) 42 (91)
complicated devices and limits the need for other rescue per to Dr Damon Kuehl and Dr John H. Burton, Carilion Clinic
sonnel to be endangered. On long trips where medications are Roanoke Memorial Hospital, for guidance and help editing
2
often in a limited supply, less need for analgesics and sedatives is this manuscript.
likely to be beneficial. This might also be important in highalti
tude scenarios where most sedatives are best avoided for fear of Financial Disclosure
respiratory depression in an alreadyhypoxic environment and The authors have no financial relationships relevant to this
because of lack of proper evidence regarding safety of these. 32 article to disclose.
The ERM can be performed with the patient supine, sitting, or Conflicts of Interest
45º recumbent. 8,12,13 The SMM is usually performed with the The authors have no conflicts of interest to disclose relevant
patient prone, although it can also be performed in the supine to this article.
or seated positions. Positioning, airway issues due to prone
15
positioning, and difficulty performing the technique on obese Author Contributions
patients are some of SMM’s challenges. 8 DK conceived the study concept and design. SA recruited
participants and collected and analyzed the data. SA and PK
The limitations of this study were its small sample size and short wrote the first draft, and all authors read and approved the
duration, and that is was a singlecenter–based study. Patients final manuscript.
were alternatively allocated into two groups on the basis of their
arrival in the ED; they were not randomly assigned. Reduction References
procedures were carried out with the same protocol irrespective 1. Flores AH, Haileyesus T, Greenspan AI. National estimates of out
of age of the patient or prior history of dislocation. These are door recreational injuries treated in emergency departments, United
factors known to influence the outcome of reduction maneuvers. States, 2004–2005. Wilderness Environ Med. 2008;19(2):91–98.
All the reductions were performed by a resident physician un 2. Ditty J, Chisholm D, Davis SM, et al. Safety and efficacy of at
der training, accounting for the lower success rates in this study tempts to reduce shoulder dislocations by nonmedical personnel in
the wilderness setting. Wilderness Environ Med. 2010;21(4):357–
compared with those of other studies of these methods. Because 361.e352.
all reductions were performed by the same physician, he might 3. Shah R, Chhaniyara P, Wallace WA, et al. Pitchside management
have become biased to either of the methods. And because this of acute shoulder dislocations: a conceptual review. BMJ Open
study was done in a hospital, some of the findings may not be Sport Exerc Med. 2017;2(1):e000116.
generalizable to all austere medicine and prehospital settings. 4. Baden DN, Roetman MH, Boeije T, et al. Biomechanical repo
sition techniques in anterior shoulder dislocation: a randomised
multicentre clinical trial the BRASDtrial protocol. BMJ Open.
Conclusion 2017;7(7):e013676.
5. Cunningham NJ. Techniques for reduction of anteroinferior shoul
We demonstrated greater success for reduction of anterior der dislocation. Emerg Med Australa. 2005;17(5–6):463–471.
shoulder dislocation with the SMM when compared with the 6. Dala-Ali B, Penna M, McConnell J, et al. Management of acute
ERM as the initial attempt technique in nonsedated ED pa anterior shoulder dislocation. Br J Sports Med. 2014;48(16):
tients with anterior shoulder dislocation. 1209–1215.
7. Guler O, Ekinci S, Akyildiz F, et al. Comparison of four different
reduction methods for anterior dislocation of the shoulder. J Or-
Acknowledgments thop Surg Res. 2015;10:80.
We thank the subjects who participated in this study. We thank 8. Mattick A, Wyatt JP. From Hippocrates to the Eskimo—a history
the Department of Orthopedics, Tribhuvan University Teach of techniques used to reduce anterior dislocation of the shoulder.
ing Hospital, for guidance and support. Our special thanks J R Coll Surg Edinb. 2000;45(5):312–316.
36 | JSOM Volume 18, Edition 3 / Fall 2018