Page 57 - JSOM Summer 2018
P. 57
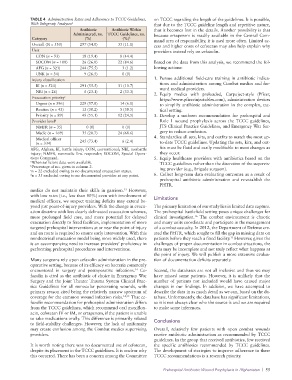
TABLE 4 Administration Rates and Adherence to TCCC Guidelines, on TCCC regarding the length of the guidelines. It is possible,
With Subgroup Analyses a that due to the TCCC guideline length and repetitive nature,
Antibiotic Antibiotic Within that it becomes lost in the details. Another possibility is that
Administered, no. TCCC Guidelines, no. because ertapenem is readily available in the Central Com-
Category (%) (%) b mand area of responsibility, it is used more often. Limited ac-
Overall (N = 550) 297 (54.0) 33 (11.1) cess and higher costs of cefotetan may also help explain why
Unit providers instead rely on cefazolin.
CON (n = 93) 18 (19.4) 8 (44.4)
SOCOM (n = 100) 26 (26.0) 22 (84.6) Based on the data from this analysis, we recommend the fol-
AFG (n = 323) 244 (75.5) 3 (1.2) lowing actions:
UNK (n = 34) 9 (26.5) 0 (0)
Injury classification 1. Pursue additional field-care training in antibiotic indica-
tions and administration among Combat medics and for-
BI (n = 524) 291 (55.5) 31 (10.7) ward medical providers.
NBI (n = 26) 6 (23.1) 2 (33.3) 2. Equip medics with preloaded, Carpuject-style (Pfizer,
Evacuation priority c https://www.pfizerinjectables.com), administration devices
Urgent (n = 396) 229 (57.8) 14 (6.1) to simplify antibiotic administration in the complex, tac-
Routine (n = 43) 13 (30.2) 5 (38.5) tical setting.
Priority (n = 89) 49 (55.1) 12 (24.5) 3. Develop a uniform recommendation for prehospital and
Provider level d Role 1 wound prophylaxis across the TCCC guidelines,
NMFR (n = 35) 0 (0) 0 (0) JTS Clinical Practice Guidelines, and Emergency War Sur-
Medic (n = 169) 35 (20.7) 24 (68.6) gery to reduce confusion.
Medical officer 4. Standardize all sets, kits, and outfits to match the most up-
(n = 334) 245 (73.4) 6 (2.4) to-date TCCC guidelines. Updating the sets, kits, and out-
AFG, Afghan; BI, battle injury; CON, conventional; NBI, nonbattle fits must be fluid and easily modifiable to meet changes as
injury; NMFR, nonmedic first responder; SOCOM, Special Opera- they occur.
tions Command. 5. Equip healthcare providers with antibiotics based on the
a When sufficient data were available. TCCC guidelines rather than the discretion of the supervis-
b Percentage of no. given in column 2.
c n = 22 excluded owing to no documented evacuation status. ing provider (e.g., brigade surgeon).
d n = 35 excluded owing to no documented provider at any point. 6. Collect long-term data evaluating outcomes as a result of
prehospital antibiotic administration and re-establish the
PHTR.
medics do not maintain their skills in garrison. However,
13
with low rates (i.e., less than 80%) even with involvement of Limitations
medical officers, we suspect training deficits may extend be-
yond just point-of-injury providers. With the change in evacu- The primary limitation of our study lies in limited data capture.
ation doctrine with less clearly delineated evacuation schemes, The prehospital battlefield setting poses unique challenges for
more prolonged field care, and more potential for delayed clinical investigation. The combat environment is chaotic
16
evacuation directly to fixed facilities, implementation of more and many units coordinate and participate in the management
targeted prehospital interventions at or near the point of injury of a combat casualty. In 2012, the Department of Defense cre-
and en route is required to ensure early intervention. With this ated the PHTR, which sought to fill the gap in missing data on
nondoctrinal evacuation model being more widely used, there patients before they reach a fixed facility. However, given the
15
is an accompanying need to increase providers’ proficiency in challenges of proper documentation in combat situations, the
performing prehospital procedures and interventions. data may be incomplete and not truly reflect what happens at
the point of injury. We will publish a more extensive evalua-
Many surgeons rely upon cefazolin administration in the pre- tion of documentation deficits separately.
operative setting, because of its efficacy on bacteria commonly
encountered in surgery and postoperative infections. Ce- Second, the databases are not all inclusive and thus we may
14
fazolin is cited as the antibiotic of choice in Emergency War have missed some patients. However, it is unlikely that the
Surgery and the Joint Theater Trauma System Clinical Prac- number of patients not included would have caused major
tice Guidelines for all nonocular penetrating wounds, with changes in our findings. In addition, we have attempted to
primary reason cited being the relatively narrow spectrum of describe the data in as much detail as we can, based on the da-
coverage for the common wound infection risks. 14,15 That ce- tabase. Unfortunately, the database has significant limitations,
fazolin recommendation for prehospital administration differs so it is not always clear who the source is and we are required
from the TCCC guidelines, which recommend oral moxiflox- to make some inferences.
acin, cefotetan IV or IM, or ertapenem, if the patient is unable
to take medications orally. This difference is primarily related Conclusions
to field-stability challenges. However, the lack of uniformity
may create confusion among the Combat medics supervising Overall, relatively few patients with open combat wounds
providers. receive antibiotic administration as recommended by TCCC
guidelines. In the group that received antibiotics, few received
It is worth noting there was no documented use of cefotetan, the specific antibiotics recommended by TCCC guidelines.
despite its placement in the TCCC guidelines. It is unclear why The development of strategies to improve adherence to these
this occurred. There has been a concern among the Committee TCCC recommendations is a research priority.
Prehospital Antibiotic Wound Prophylaxis in Afghanistan | 55