Page 53 - JSOM Summer 2018
P. 53
over mission length. Average estimates were required given that Discussion
variables such as length of mission, DCST location, CASEVAC
asset and location of POI could not realistically be controlled in In this study, the ERST significantly improves time to DCR
a combat environment over the length of the mission. and DCS in an environment without robust aeromedical evac-
uation following surgical stabilization. With the ability to re-
Prospective “Time to ED” and “Time to OR” were averaged duce prehospital time in penetrating trauma, the ERST can
and were compared with retrospective averaged times “With- reduce time to surgical hemorrhage control, thereby poten-
out ERST.” Data were entered into Microsoft Excel and an- tially enabling a reduction in trauma mortality.
alyzed by paired t-test and one-way ANOVA for significant
difference. The ERST resulted from the discrepancy between elevated
risk of SOF missions and medical evacuation within US Af-
rica Command (AFRICOM). The development of a suitable
Results medical response to the discrepancy of trauma coverage in
Eleven Special Operations missions were supported by the AFRICOM posed a unique challenge. Comparative access to
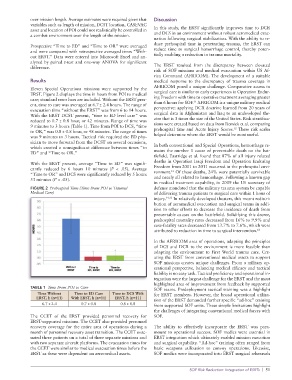
ERST. Figure 2 displays the time in hours from POI to medical surgical care is similar to early experiences in Operation Endur-
care; standard error bars are included. Without the ERST pres- ing Freedom with time to operative treatment averaging greater
11
ent, time to care was averaged at 6.7 ± 2.4 hours. The range of than 6 hours for SOF. AFRICOM is a unique military medical
evacuation time “without the ERST” was from 6 to 14 hours. perspective: applying DCR doctrine learned from 20 years of
With the ERST DCST present, “time to ED level care” was surgical data in Afghanistan and Iraq to an undeveloped the-
reduced to 0.7 ± 0.8 hour, or 42 minutes. Range of time was ater that is 3 times the size of the United States. Risk stratifica-
9 minutes to 3 hours (Table 1). Time from POI to DCS, “time tions were created based on data from Remick et al. comparing
12
to OR,” was 0.8 ± 0.8 hour, or 48 minutes. The range of times prehospital time and Acute Injury Scores. These risk scales
was 9 minutes to 3 hours. Tactical risk required the ED phy- helped determine where the ERST would be most useful.
sician to move forward from the DCST on several occasions,
which created a nonsignificant difference between times “to In both conventional and Special Operations, hemorrhage re-
ED” and “Time to OR.” mains the number 1 cause of preventable death on the bat-
tlefield. Eastridge et al. found that 87% of all injury related
With the ERST present, average “Time to ED” was signifi- deaths in Operation Iraqi Freedom and Operation Enduring
cantly reduced by 6 hours 10 minutes (P < .05). Average Freedom from 2001 to 2011 occurred in the prehospital envi-
13
“Time to OR” and DCS were significantly reduced by 5 hours ronment. Of these deaths, 24% were potentially survivable
53 minutes (P < .05). and nearly all related to hemorrhage. Following a known gap
in medical treatment capability, in 2009 the US secretary of
FIGURE 2 Prehospital Time (Time From POI to Trauma/ defense mandated that the military trauma system be capable
Medical Care) of delivering trauma patients to surgical care within 1 hour of
injury. 14,15 In relatively developed theaters, this meant redistri-
bution of aeromedical evacuation and surgical teams in addi-
tion to other efforts to decrease the incidence of death from
preventable causes on the battlefield. Solidifying this decree,
prehospital mortality rates decreased from 16% to 9.9% and
case-fatality rates decreased from 13.7% to 7.6%, which were
attributed to reduction in time to surgical intervention. 16
In the AFRICOM area of operations, adapting the principles
of DCS and DCR to the environment is more feasible than
adapting the environment to First World trauma care. Cre-
ating the ERST from conventional medical assets to support
SOF missions creates unique challenges. From a military op-
erational perspective, balancing medical efficacy and tactical
liability is no easy task. Tactical proficiency and operational in-
tegration were the largest challenge for the ERST and the most
highlighted area of improvement from feedback by supported
TABLE 1 Time From POI to Care SOF teams. Predeployment tactical training was a highlight
Time Without Time to ED Care Time to DCS With for ERST members. However, the broad operational utiliza-
ERST, h (n=11) With ERST, h (n=11) ERST, h (n=11) tion of the ERST demanded further specific “ad-hoc” training
6.7 ± 2.4 0.7 ± 0.8 0.8 ± 0.8 from supported SOF units. These simple limitations highlight
the challenges of integrating conventional medical forces with
The CCET of the ERST provided personnel recovery for SOF.
ERST-supported missions. The CCET also provided personnel
recovery coverage for the entire area of operations during a The ability to effectively incorporate the ERST was para-
month of personnel recovery asset transition. The CCET evac- mount to operational success. SOF medics were essential in
uated three patients on a total of three separate missions and ERST integration which ultimately enabled mission execution
with two separate aircraft platforms. The evacuation times for and surgical capability. “Ad-hoc” training often ranged from
the CCET were similar to medical evacuation times before the basic weapons utilization to convoy operations. Likewise,
ERST as these were dependent on aeromedical assets. SOF medics were incorporated into ERST surgical rehearsals
SOF Risk Reduction: Integration of ESRTs | 51