Page 45 - JSOM Spring 2018
P. 45
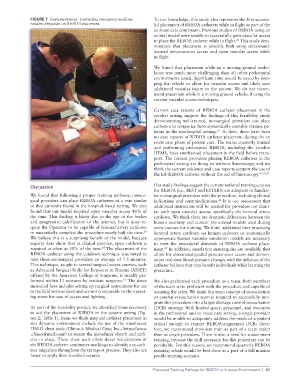
FIGURE 7 Implementation. Instructing emergency medicine To our knowledge, this study also represents the first success-
resident physician on REBOA placement. ful placement of REBOA catheters while in flight as part of the
en route care continuum. Previous studies of REBOA using an
animal model were unable to successfully gain vascular access
to place the REBOA catheter while in flight. This study dem-
26
onstrates that placement is possible both using ultrasound-
assisted percutaneous access and open vascular access while
in flight.
We found that placement while in a moving ground ambu-
lance was much more challenging than all other prehospital
environments tested. Significant time would be saved by stop-
ping the vehicle to allow for vascular access and likely save
additional vascular injury to the patient. We do not recom-
mend placement while in a moving ground vehicle, if using the
current vascular access techniques.
Current case reports of REBOA catheter placement in the
combat setting support the findings of this feasibility study
demonstrating well-trained, nonsurgical providers can place
catheters to temporize hemodynamically unstable trauma pa-
tients in the nonhospital setting. To date, there have been
16
no case reports of REBOA catheter placement during the en
route care phase of patient care. The teams currently trained
and performing prehospital REBOA, including the London
HEMS, have emphasized placement in the field before trans-
port. The current providers placing REBOA catheters in the
prehospital setting are doing so without fluoroscopy, and we
think the current evidence and case reports support the use of
the ER-REBOA catheter without the aid of fluoroscopy. 16,17,27
Discussion Our study findings suggest the current national training courses
for REBOA (i.e., BEST and ESTARS) are adequate to familiar-
We found that following a proper training pathway, nonsur- ize nonsurgical providers with the procedure, including clinical
gical providers can place REBOA catheters at a rate similar indications and contraindications. It is our assessment that
28
to that currently found in the hospital-based setting. We also additional instruction will be needed for providers not famil-
found that our model required open vascular access 46% of iar with open vascular access, specifically the femoral artery
the time. This finding is likely due to the age of the bodies cutdown. We think there are dramatic differences between the
and progressive calcification of the arteries, but it does re- human anatomy and current live-animal models used during
quire the Operator to be capable of femoral artery cutdown some courses for training. We think additional time practicing
to successfully complete the procedure nearly half the time. 20 femoral artery cutdown on human cadavers or anatomically
We believe this is a surprising benefit of the model, because appropriate human vascular simulation models are necessary
registry data show that in clinical practice, open cutdown is to meet the procedural demands of REBOA catheter place-
24
required as often as 50% of the time. The placement of the ment. In addition, simulation mannequins are available that
25
REBOA catheter using the cutdown technique was noted to allow for ultrasound-guided percutaneous access and demon-
take these nonsurgical providers an average of 7.5 minutes. strate real-time blood pressure changes with the inflation of the
This technique, taught in several surgical access courses, such catheter balloon that may benefit individuals while learning the
as Advanced Surgical Skills for Exposure in Trauma (ASSET) procedure.
offered by the American College of Surgeons, is usually per-
formed within 12 minutes by resident surgeons. The times We also performed each procedure as a team. Both members
25
measured here includes setting up surgical instruments for use of the team were proficient with the procedure and capable of
in the field environment and are not comparable to the operat- assisting the other. We think this team concept of resuscitation
ing room for ease of access and lighting. or combat resuscitation team is required to successfully inte-
grate this procedure into a larger damage control resuscitation
As part of the feasibility project, we identified items necessary (DCR) strategy. With limited space, personnel, and resources
to aid the placement of REBOA in the austere setting (Fig- in the prehospital and en route care setting, a single provider
ure 2; Table 1). Items we think may aid catheter placement in would be unable to adequately address the needs of a patient
this dynamic environment include the use of the translucent critical enough to require REBOA-augmented DCR; there-
HALO chest seals (Chinook Medical Gear, Inc., https://www fore, we recommend providers train as part of a team rather
.chinookmed.com/) to secure the introducer sheath and cath- than as single providers. There is also a need for sustainment
eter in place. These chest seals allow direct visualization of training, because the skill necessary for this procedure can be
the REBOA catheter centimeter markings to identify any cath- perishable. For this reason, we recommend quarterly REBOA
eter migration throughout the transport process. They also are training, which would be best done as a part of a full mission
faster to apply than standard sutures. profile training scenario.
Proposed Training Pathway for REBOA in Austere Environment | 41