Page 31 - JSOM Spring 2018
P. 31
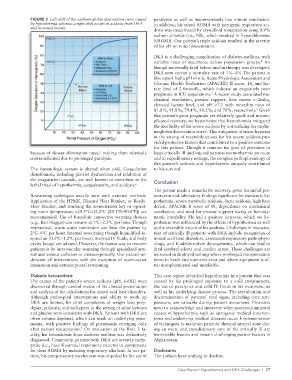
FIGURE 3 Left shift of the oxyhemoglobin dissociation curve caused paralytics as well as inappropriately low minute ventilation.
by hypothermia, whereas a right shift occurs in acidosis from DKA In addition, his mixed AGMA with iatrogenic respiratory aci-
and increased lactate.
dosis was exacerbated by crystalloid resuscitation using 0.9%
sodium chloride (i.e., NS), which resulted in hyperchloremic
NAGMA. Our patient’s triple acidosis resulted in the severity
of his pH on initial presentation.
DKA is a challenging complication of diabetes mellitus, with
variable rates of occurrence across population groups. Al-
8
though universally fatal before insulin therapy was developed,
DKA now carries a mortality rate of 1%–4% The patient in
this report had a pH of 6.6, Acute Physiologic Assessment and
Chronic Health Evaluation (APACHE) II score, 18, and lac-
tate level of 2.8mmol/L, which indicate an exquisitely poor
prognosis in ICU populations. A recent study associated me-
9
chanical ventilation, pressor support, base excess <−2mEq,
elevated lactate level, and pH <7.2 with mortality rates of
81.8%, 91.8%, 79.4%, 80.2%, and 70%, respectively. Given
9
this patient’s poor prognosis yet relatively quick and uncom-
plicated recovery, we hypothesize that hypothermia mitigated
the morbidity of his severe acidosis by normalizing his oxyhe-
moglobin dissociation curve. This mitigation of tissue hypoxia
in the setting of reversible causes for his severe acidosis pro-
vided protective factors that contributed to a positive outcome
for this patient. Though it remains the goal of providers to
because of slower elimination rates, making them relatively keep critically ill and injured patients normothermic en route
5
contraindicated due to prolonged paralysis. and in expeditionary settings, the complex pathophysiology of
this patient’s acidosis and hypothermia uniquely contributed
The hematologic system is altered when cold. Coagulation to his survival.
disturbances, including platelet dysfunction and inhibition of
the coagulation cascade, are well known to contribute to the Conclusion
lethal triad of hypothermia, coagulopathy, and acidosis. 6
The patient made a remarkable recovery, given his initial pre-
Rewarming techniques usually start with external methods. sentation and laboratory findings significant for moderate hy-
Application of the HPMK, Blizzard Heat Blanket, or Ready- pothermia, severe metabolic acidosis, lactic acidosis, high base
Heat Blanket, and warming the resuscitation bay or operat- deficit, APACHE II score of 18, dependence on mechanical
ing room (temperature >29.5°C–32.2°C [85.1°F–90.0°F]) are ventilation, and need for pressor support owing to hemody-
recommended. Use of forced-air convective warming devices namic instability. He had a positive outcome, which we hy-
(e.g., Bair Hugger) can rewarm at 1°C–2.5°C per hour. Though pothesize was influenced by the effects of hypothermia as well
impractical, warm-water immersion can heat the patient by as the reversible nature of his acidosis. Challenges in resuscita-
2°C–4°C per hour. Internal rewarming though humidified in- tion of critically ill patients with DKA include recognition of
spired air (0.5°C–1.2°C per hour), warmed IV fluids, and body mixed acid-base disorders, associated respiratory pathophysi-
cavity lavage are advised. However, the fastest way to rewarm ology, and fluid/electrolyte derangements, which can lead to
patients is by intravascular warming through specialized arte- fatal cerebral edema and cardiac arrest. These challenges are
rial and venous catheters or extracorporeally. Our patient un- increased in deployed settings where prolonged transportation
derwent all interventions with the exception of warm-water times in harsh environments exist and where equipment is of-
immersion and extracorporeal rewarming. ten unsophisticated and unreliable.
Diabetic ketoacidosis This case report identified hypothermia in a patient that was
The causes of the patient’s severe acidosis (pH, 6.682) were caused by his prolonged exposure to a cold environment,
discovered through careful review of his clinical presentation the use of paralytics and cold IV fluids in his treatment, as
and analysis of the calculations for mixed acid-base disorders. well as his underlying disease process. The reevaluation and
Although prehospital interventions and ability to work up documentation of patients’ vital signs, including core tem-
DKA are limited, his chief complaints of weight loss, poly- perature, are valuable during patient movement. Providers
dipsia, polyuria, and tachypnea in the setting of urine ketones need to acknowledge and intervene when nonenvironmental
and glucose were consistent with DKA. Patients with DKA are causes of hypothermia such as iatrogenic medical interven-
often volume depleted, which can mask an underlying pneu- tions and underlying medical diseases occur. Implementation
monia, with positive findings of pneumonia emerging only of techniques to maintain patients’ thermal neutral zone dur-
after patient resuscitation. On evaluation at the Role 3 fa- ing en route and expeditionary care of the critically ill are
7
cility, his ketoacidosis from diabetes mellitus was definitively memorable lessons and remain challenging patient factors in
diagnosed. Commonly, patients with DKA are severely tachy- Afghanistan.
pneic (i.e., have Kussmaul respiratory pattern) to compensate
for their AGMA by inducing respiratory alkalosis. In our pa- Disclosures
tient, his compensatory mechanism was impeded by the use of The authors have nothing to disclose.
Case Report: Hypothermia and DKA Challenges | 27