Page 149 - JSOM Spring 2018
P. 149
clinic to obtain posteroanterior and lateral radiographs of the 4mm, those that have an articular “step-off” greater than
affected limb. The lateral images visualized an isolated trans- 3mm and those with extensor mechanism disruption (i.e.,
verse patella fracture (Figure 1). The patient was given 60mg inability to perform straight leg raise).
ketorolac intramuscularly for pain relief. The limb was stabi- 2. Surgical repair should be performed as soon as possible but
lized with a posterior splint that did not include the ankle so no later than 7 to 14 days following the injury in order to
that the patient could bear weight as tolerated. The Service- decrease the likelihood of long-term functional deficits.
member was scheduled to depart for Fort Bragg, NC, 3 days 3. Open fractures add additional risk. They should undergo
after the incident with plans to arrive at Fort Bragg, NC, 3 to surgical repair within 12 hours or risk septic arthritis
5 days after departure. within 72 hours and chronic osteomyelitis. Patients should
receive antibiotics and local wound care as soon as possible
Clinical Questions while awaiting surgical repair.
1. Is more immediate evacuation required in order to avoid 4. Nonoperative management for patella fractures without
permanent deficit? the above characteristics include splint immobilization,
2. What is the proper splinting position for this patient until early weight bearing, and early physical therapy.
transport can be arranged? 5. The ideal splint for a patella fracture is a posterior knee
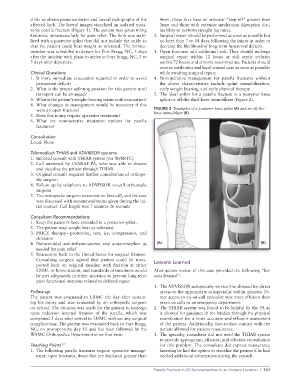
3. What is the patient’s weight-bearing status until evacuation? splint or off-the-shelf knee immobilizer (Figure 2).
4. What changes in management would be necessary if this
were an open fracture? FIGURE 2 Examples of a posterior knee splint (A) and an off-the-
5. Does this injury require operative treatment? knee immobilizer (B).
6. What are nonoperative treatment options for patella
fractures?
Consultation
Local: None
Telemedical: THIAB and ADVISSOR systems
1. Initiated consult with THIAB system (via WebRTC)
2. Call answered by USARAF PA, who was able to discuss
and visualize the patient through THIAB
3. Original consult required further consultation of orthope-
dic surgeon
4. Follow up by telephone to ADVISSOR on-call orthopedic
surgeon
5. The orthopedic surgeon answered on first call, and the case
was discussed with recommendations given during the ini-
tial contact. Call length was 7 minutes 26 seconds
Consultant Recommendations
1. Keep the patient’s knee extended in a posterior splint.
2. The patient may weight bear as tolerated.
3. PRICE therapy—protection, rest, ice, compression, and
elevation
4. Nonsteroidal anti-inflammatories and acetaminophen as (A) (B)
needed for pain relief
5. Evacuation back to the United States for surgical fix ation.
Consulting surgeon agreed that patient could be trans- Lessons Learned
ported back on original timeline with fixation at either
LRMC or home station, and standards of timeliness would After action review of this case provided the following “les-
be met adequately in either situation to prevent long-term sons learned”:
poor functional outcome related to delayed repair.
1. The ADVISSOR subspecialty service line allowed for direct
Follow-up access to the appropriate subspecialist within minutes. Di-
The patient was evacuated to LRMC the day after sustain- rect access to an on-call specialist was more efficient than
ing his injury and was evaluated by an orthopedic surgeon previous calls to an emergency department.
on arrival. The decision was made for the patient to undergo 2. The THIAB system was found to be helpful by the PA as
open reduction internal fixation of the patella, which was it allowed for guidance of the Medics through the physical
completed 3 days after arrival to LRMC without any surgical examination for a more accurate and efficient assessment
complications. The patient was evacuated back to Fort Bragg, of the patient. Additionally, face-to-face contact with the
NC, on postoperative day 15 and has been followed by the patient allowed for patient reassurance.
WAMC Orthopedics Department since that time. 3. The specialty consultant did not need the THIAB system
to provide appropriate, efficient, and effective consultation
Teaching Points 1,2 for this problem. The consultant did express reassurance
1. The following patella fractures require operative manage- knowing he had the option to visualize the patient if he had
ment: open fractures, those that are displaced greater than needed additional information during the consult.
Patella Fracture in US Servicemember in an Austere Location | 143