Page 79 - Journal of Special Operations Medicine - Fall 2017
P. 79
SKILLS
Figure 9 An empty intravenous (IV) solution bag taped to the arm allows the medic to start an IV and inject replica/dummy medications. It is
not practical to start an IV line on all role players because medications or “training” medications cannot be injected. By adding patient scripts
and cues, a unit can use its own members, or request tasking a different unit to provide patients. By allowing participants to act out what they
need reduces additional interactions between the evaluator and the medic. When using role players, having a “safe” word for these participants
instead of the medic asking if performing an IV, nasopharyngeal airway, and so forth is acceptable to that role player, the medic can then perform
the task without hesitation on the set-up IV bag. We see IVs as a stand-alone exercise that should be practiced among teammates monthly. To
overcome the loss of ability to draw and administer medications per protocol, we use empty IV bags and practice bones for interosseous (IO)
administration in a simple manner.
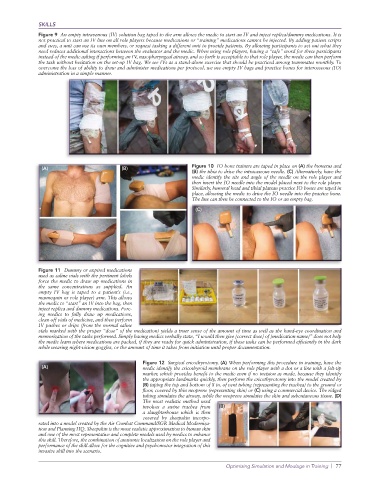
Figure 10 IO bone trainers are taped in place on (A) the humerus and
(A) (B)
(B) the tibia to drive the intraosseous needle. (C) Alternatively, have the
medic identify the site and angle of the needle on the role player and
then insert the IO needle into the model placed next to the role player.
Similarly, humeral head and tibial plateau practice IO bones are taped in
place, allowing the medic to drive the IO needle into the practice bone.
The line can then be connected to the IO or an empty bag.
(C)
Figure 11 Dummy or expired medications
used as saline vials with the pertinent labels
force the medic to draw up medications in
the same concentrations as supplied. An
empty IV bag is taped to a patient’s (i.e.,
mannequin or role player) arm. This allows
the medic to “start” an IV into the bag, then
inject replica and dummy medications. Forc-
ing medics to fully draw up medications,
clean off vials of medicine, and then perform
IV pushes or drips (from the normal saline
vials marked with the proper “dose” of the medication) yields a truer sense of the amount of time as well as the hand-eye coordination and
memorization of the tasks performed. Simply having medics verbally state, “I would then give [correct dose] of [medication name]” does not help
the medic learn where medications are packed, if they are ready for quick administration, if these tasks can be performed efficiently in the dark
while wearing night-vision goggles, or the amount of time it takes from initiation until proper documentation.
Figure 12 Surgical cricothyrotomy. (A) When performing this procedure in training, have the
(A) medic identify the cricothyroid membrane on the role player with a dot or a line with a felt-tip
marker, which provides benefit to the medic even if no incision as made, because they identify
the appropriate landmarks quickly, then perform the cricothyrotomy into the model created by
(B) taping the top and bottom of 8 in. of vent tubing (representing the trachea) to the ground or
floor, covered by thin neoprene (representing skin) or (C) using a commercial device. The ridged
tubing simulates the airway, while the neoprene simulates the skin and subcutaneous tissue. (D)
The most realistic method used
involves a swine trachea from (B)
a slaughterhouse which is then
covered by sheepskin incorpo-
rated into a model created by the Air Combat Command/SGR Medical Moderniza-
tion and Planning HQ. Sheepskin is the most realistic approximation to human skin
and one of the most representative and complete models used by medics to enhance
this skill. Therefore, the combination of anatomic localization on the role player and
performance of the skill allow for the cognitive and psychomotor integration of this
invasive skill into the scenario.
Optimizing Simulation and Moulage in Training | 77