Page 59 - Journal of Special Operations Medicine - Fall 2017
P. 59
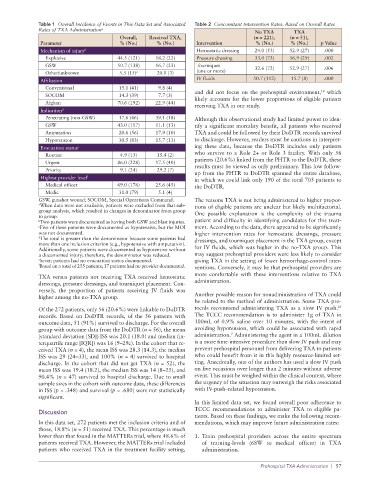
Table 1 Overall Incidence of Events in This Data Set and Associated Table 2 Concomitant Intervention Rates, Based on Overall Rates
Rates of TXA Administration a No TXA TXA
Overall, Received TXA, (n = 221), (n = 51),
Parameter % (No.) % (No.) Intervention % (No.) % (No.) p Value
Mechanism of injury b Hemostatic dressing 24.0 (53) 52.9 (27) .000
Explosive 44.5 (121) 18.2 (22) Pressure dressing 33.0 (73) 56.9 (29) .002
GSW 50.7 (138) 16.7 (23) Tourniquet 32.6 (72) 52.9 (27) .006
Other/unknown 5.5 (15) c 20.0 (3) (one or more)
Affiliation IV fluids 50.7 (112) 15.7 (8) .000
Conventional 15.1 (41) 9.8 (4) 18
SOCOM 14.3 (39) 7.7 (3) and did not focus on the prehospital environment, which
likely accounts for the lower proportions of eligible patients
Afghan 70.6 (192) 22.9 (44) receiving TXA in our study.
Indication d
Penetrating (non-GSW) 17.6 (46) 39.1 (18) Although this observational study had limited power to iden-
GSW 43.0 (117) 11.1 (13) tify a significant mortality benefit, all patients who received
Amputation 20.6 (56) 17.9 (10) TXA and could be followed by their DoDTR records survived
Hypotension 30.5 (83) 15.7 (13) to discharge. However, readers must be cautious in interpret-
Evacuation status e ing these data, because the DoDTR includes only patients
Routine 4.9 (13) 15.4 (2) who survive to a Role 2+ or Role 3 facility. With only 56
Urgent 86.0 (228) 17.5 (40) patients (20.6%) linked from the PHTR to the DoDTR, these
results must be viewed as only preliminary. This low follow-
Priority 9.1 (24) 29.2 (7) up from the PHTR to DoDTR spanned the entire database,
Highest provider level f in which we could link only 190 of the total 705 patients to
Medical officer 69.0 (176) 25.6 (45) the DoDTR.
Medic 31.0 (79) 5.1 (4)
GSW, gunshot wound; SOCOM, Special Operations Command. The reasons TXA is not being administered to higher propor-
a When data were not available, patients were excluded from that sub- tions of eligible patients are unclear but likely multifactorial.
group analysis, which resulted in changes in denominator from group One possible explanation is the complexity of the trauma
to group.
b Two patients were documented as having both GSW and blast injuries. patient and difficulty in identifying candidates for this treat-
c Five of these patients were documented as hypotensive, but the MOI ment. According to the data, there appeared to be significantly
was not documented. higher intervention rates for hemostatic dressings, pressure
d The total is greater than the denominator because some patients had dressings, and tourniquet placement in the TXA group, except
more than one inclusion criterion (e.g., hypotensive with amputation).
Additionally, some patients were documented as hypotensive without for IV fluids, which was higher in the no-TXA group. This
a documented injury; therefore, the denominator was reduced. may suggest prehospital providers were less likely to consider
e Seven patients had no evacuation status documented. giving TXA in the setting of fewer hemorrhage-control inter-
f Based on a total of 255 patients; 17 patients had no provider documented. ventions. Conversely, it may be that prehospital providers are
TXA versus patients not receiving TXA received hemostatic more comfortable with these interventions relative to TXA
dressings, pressure dressings, and tourniquet placement. Con- administration.
versely, the proportion of patients receiving IV fluids was
higher among the no-TXA group. Another possible reason for nonadministration of TXA could
be related to the method of administration. Some TXA pro-
25
Of the 272 patients, only 56 (20.6%) were linkable to DoDTR tocols recommend administering TXA as a slow IV push.
records. Based on DoDTR records, of the 56 patients with The TCCC recommendation is to administer 1g of TXA in
outcome data, 51 (91%) survived to discharge. For the overall 100mL of 0.9% saline over 10 minutes, with the intent of
group with outcome data from the DoDTR (n = 56), the mean avoiding hypotension, which could be associated with rapid
7
(standard deviation [SD]) ISS was 20.1 (18.0) and median (in- administration. Administering the agent in a 100mL dilution
terquartile range [IQR]) was 16 (9–29c). In the cohort that re- is a more time-intensive procedure than slow IV push and may
ceived TXA (n = 4), the mean ISS was 28.3 (14.3), the median prevent prehospital personnel from delivering TXA to patients
ISS was 29 (24–33), and 100% (n = 4) survived to hospital who could benefit from it in this highly resource-limited set-
discharge. In the cohort that did not get TXA (n = 52), the ting. Anecdotally, one of the authors has used a slow IV push
mean ISS was 19.4 (18.2), the median ISS was 14 (8–25), and on five occasions over longer than 2 minutes without adverse
90.4% (n = 47) survived to hospital discharge. Due to small event. This must be weighed within the clinical context, where
sample sizes in the cohort with outcome data, these differences the urgency of the situation may outweigh the risks associated
in ISS (p = .348) and survival (p = .680) were not statistically with IV-push–related hypotension.
significant.
In this limited data set, we found overall poor adherence to
Discussion TCCC recommendations to administer TXA to eligible pa-
tients. Based on these findings, we make the following recom-
In this data set, 272 patients met the inclusion criteria and of mendations, which may improve future administration rates:
those, 18.8% (n = 51) received TXA. This percentage is much
lower than that found in the MATTERs trial, where 48.6% of 1. Train prehospital providers across the entire spectrum
patients received TXA. However, the MATTERs trial included of training-levels (68W to medical officer) in TXA
patients who received TXA in the treatment facility setting, administration.
Prehospital TXA Administration | 57