Page 119 - Journal of Special Operations Medicine - Spring 2017
P. 119
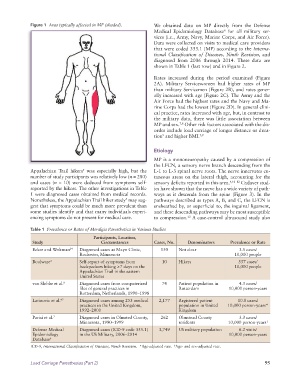
Figure 1 Area typically affected in MP (shaded). We obtained data on MP directly from the Defense
Medical Epidemiology Database for all military ser-
6
vices (i.e., Army, Navy, Marine Corps, and Air Force).
Data were collected on visits to medical care providers
that were coded 355.1 (MP) according to the Interna-
tional Classification of Diseases, Ninth Revision, and
diagnosed from 2006 through 2014. These data are
shown in Table 1 (last row) and in Figure 2.
Rates increased during the period examined (Figure
2A). Military Servicewomen had higher rates of MP
than military Servicemen (Figure 2B), and rates gener-
ally increased with age (Figure 2C). The Army and the
Air Force had the highest rates and the Navy and Ma-
rine Corps had the lowest (Figure 2D). In general clini-
cal practice, rates increased with age, but, in contrast to
the military data, there was little association between
MP and sex. Other risk factors associated with the dis-
7,8
order include load carriage of longer distance or dura-
tion and higher BMI. 7,9
5
Etiology
MP is a mononeuropathy caused by a compression of
the LFCN, a sensory nerve branch descending from the
5
Appalachian Trail hikers was especially high, but the L-1 to L-3 spinal nerve roots. The nerve innervates cu-
number of study participants was relatively low (n = 280) taneous areas on the lateral thigh, accounting for the
and cases (n = 10) were deduced from symptoms self- sensory deficits reported in this area. 4,10–12 Cadaver stud-
reported by the hikers. The other investigations in Table ies have shown that the nerve has a wide variety of path-
1 were diagnosed cases obtained from medical records. ways as it descends from the spine (Figure 3). In the
5
Nonetheless, the Appalachian Trail hiker study may sug- pathways described as types A, B, and C, the LFCN is
gest that symptoms could be much more prevalent than ensheathed by, or superficial to, the inguinal ligament,
some studies identify and that many individuals experi- and these descending pathways may be most susceptible
encing symptoms do not present for medical care. to compression. A case-control ultrasound study also
13
Table 1 Prevalence or Rates of Meralgia Paresthetica in Various Studies
Participants, Location,
Study Circumstances Cases, No. Denominators Prevalence or Rate
Ecker and Woltman 24 Diagnosed cases at Mayo Clinic, 150 Not clear 3.5 cases/
Rochester, Minnesota 10,000 people
Boulware 5 Self-report of symptoms from 10 Hikers 357 cases/
backpackers hiking ≥7 days on the 10,000 people
Appalachian Trail in the eastern
United States
van Slobbe et al. 8 Diagnosed cases from computerized 74 Patient population in 4.3 cases/
files of general practices in Rotterdam 10,000 person-years
Rotterdam, Netherlands, 1990–1998
Latinovic et al. 47 Diagnosed cases among 253 medical 2,177 Registered patient 10.8 cases/
practices in the United Kingdom, population in United 10,000 person-years*
1992–2000 Kingdom
Parisi et al. 7 Diagnosed cases in Olmsted County, 262 Olmstead County 3.3 cases/
Minnesota, 1990–1999 residents 10,000 person-years †
Defense Medical Diagnosed cases (ICD-9 code 355.1) 3,749 US military population 6.2 visits/
Epidemiology in the US Military, 2006–2014 10,000 person-years
Database 6
ICD-9, International Classification of Diseases, Ninth Revision. *Age-adjusted rate. Age- and sex-adjusted rate.
†
Load Carriage Paresthesias (Part 2) 95