Page 120 - Journal of Special Operations Medicine - Spring 2017
P. 120
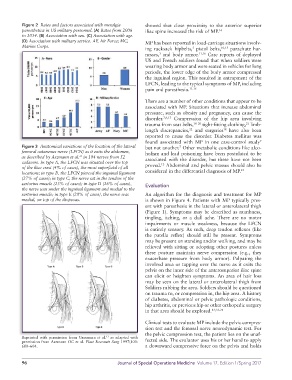
Figure 2 Rates and factors associated with meralgia showed that close proximity to the anterior superior
paresthetica in US military personnel. (A) Rates from 2006 iliac spine increased the risk of MP. 14
to 2014. (B) Association with sex. (C) Association with age.
(D) Association with military service. AF, Air Force; MC, MP has been reported in load-carriage situations involv-
Marine Corps.
ing rucksack hipbelts, pistol belts, 10,15 parachute har-
5
nesses, and body armor. 11,16 Case reports of deployed
3
US and French soldiers found that when soldiers were
wearing body armor and were seated in vehicles for long
periods, the lower edge of the body armor compressed
the inguinal region. This resulted in entrapment of the
LFCN, leading to the typical symptoms of MP, including
pain and paresthesia. 11,16
There are a number of other conditions that appear to be
associated with MP. Situations that increase abdominal
pressure, such as obesity and pregnancy, can cause the
disorder. 7,9,17 Compression of the hip area involving
trauma from seat belts, 18–20 tight-fitting clothing, limb-
21
length discrepancies, and surgeries have also been
22
18
reported to cause the disorder. Diabetes mellitus was
found associated with MP in one case-control study
7
Figure 3 Anatomical variations of the location of the lateral but not another. Other metabolic conditions like alco-
7
femoral cutaneous nerve (LFCN) as it exits the abdomen, holism and lead poisoning have been postulated to be
as described by Aszmann et al. in 104 nerves from 52 associated with the disorder, but these have not been
13
cadavers. In type A, the LFCN was situated over the top 12
of the iliac crest (4% of cases), the most superficial of all proved. Abdominal and pelvic masses should also be
23
locations; in type B, the LFCN pierced the inguinal ligament considered in the differential diagnosis of MP.
(27% of cases); in type C, the nerve sat in the tendon of the
sartorius muscle (23% of cases); in type D (26% of cases), Evaluation
the nerve was under the inguinal ligament and medial to the
sartorius muscle; in type E (20% of cases), the nerve was An algorithm for the diagnosis and treatment for MP
medial, on top of the iliopsoas. is shown in Figure 4. Patients with MP typically pres-
ent with paresthesia in the lateral or anterolateral thigh
(Figure 1). Symptoms may be described as numbness,
tingling, itching, or a dull ache. There are no motor
impairments or muscle weakness, because the LFCN
is entirely sensory. As such, deep tendon reflexes (like
the patella reflex) should still be present. Symptoms
may be present on standing and/or walking, and may be
relieved with sitting or adopting other postures unless
these posture maintain nerve compression (e.g., they
exacerbate pressure from body armor). Palpating the
involved area or tapping over the nerve as it exits the
pelvis on the inner side of the anterosuperior iliac spine
can elicit or heighten symptoms. An area of hair loss
may be seen on the lateral or anterolateral thigh from
Soldiers rubbing the area. Soldiers should be questioned
on trauma to, or compression in, the hip area. A history
of diabetes, abdominal or pelvic pathologic conditions,
hip arthritis, or previous hip or other orthopedic surgery
in that area should be explored. 12,23–25
Clinical tests to evaluate MP include the pelvic compres-
sion test and the femoral nerve neurodynamic test. For
the pelvic compression test, the patient lies on the unaf-
Reprinted with permission from Grossman et al. as adapted with
13
permission from Aszmann OC et al. Plast Reconstr Surg 1997;100: fected side. The evaluator uses his or her hand to apply
600–604. a downward compressive force on the pelvis and holds
96 Journal of Special Operations Medicine Volume 17, Edition 1/Spring 2017