Page 81 - Journal of Special Operations Medicine - Winter 2015
P. 81
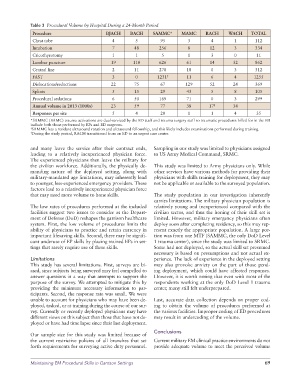
Table 3 Procedural Volume by Hospital During a 24-Month Period
Procedure BJACH BACH SAMMC* MAMC RACH WACH TOTAL
Chest tube 4 5 95 3 4 1 112
Intubation 7 48 256 8 12 3 334
Cricothyrotomy 1 1 5 1 3 0 11
Lumbar puncture 19 110 626 61 14 32 862
Central line 2 11 278 18 0 3 312
FAST 3 0 1231 † 11 6 4 1255
Dislocations/reductions 22 75 67 129 52 24 369
Splints 5 15 29 43 5 8 105
Procedural sedations 6 50 169 71 0 3 299
Annual volume in 2013 (1000s) 23 59 77 38 17 ‡ 34
Responses per site 5 4 20 1 1 4 35
*SAMMC (BAMC) trauma activations are dual-serviced by the ED staff and trauma surgery staff so traumatic procedures billed for in the ED
include both those performed by EPs and ED surgeons.
† SAMMC has a resident ultrasound rotation and ultrasound fellowship, and this likely includes examinations performed during training.
‡ During the study period, RACH transitioned from an ED to an urgent care center.
and many leave the service after their contract ends, Sampling in our study was limited to physicians assigned
leading to a relatively inexperienced physician force. to US Army Medical Command, SRMC.
The experienced physicians then leave the military for
the civilian workforce. Additionally, the physically de- This study was limited to Army physicians only. While
manding nature of the deployed setting, along with other services have various methods for providing their
military-mandated age limitations, may inherently lead physicians with skills training for deployment, they may
to younger, less-experienced emergency providers. These not be applicable or available to the surveyed population.
factors lead to a relatively inexperienced physician force
that may need more volume to hone skills. The study population in our investigation inherently
carries limitations. The military physician population is
The low rates of procedures performed at the included relatively young and inexperienced compared with the
facilities suggest two issues to consider as the Depart- civilian sector, and thus the honing of their skill set is
ment of Defense (DoD) reshapes the garrison healthcare limited. However, military emergency physicians often
system. First, the low volume of procedures limits the deploy soon after completing residency, so this may rep-
ability of physicians to practice and retain currency in resent exactly the appropriate population. A large por-
important lifesaving skills. Second, there may be signifi- tion was from one MTF (SAMMC, the only DoD Level
cant underuse of EP skills by placing trained EPs in set- 1 trauma center), since the study was limited to SRMC.
tings that rarely require use of these skills. Some had not deployed, so the actual skill set presumed
necessary is based on presumptions and not actual ex-
Limitations perience. The lack of experience in the deployed setting
This study has several limitations. First, surveys are bi- may also provoke anxiety on the part of those pend-
ased, since subjects being surveyed may feel compelled to ing deployment, which could have affected responses.
answer questions in a way that attempts to support the However, it is worth noting that even with most of the
purpose of the survey. We attempted to mitigate this by respondents working at the only DoD Level 1 trauma
providing the minimum necessary information to par- center, many still felt underprepared.
ticipants. Second, the response rate was small. We were
unable to account for physicians who may have been de- Last, accurate data collection depends on proper cod-
ployed, tasked, or at training during the course of our sur- ing to obtain the volume of procedures performed at
vey. Currently or recently deployed physicians may have the various facilities. Improper coding of ED procedures
different views on this subject than those that have not de- may result in undercoding of the volume.
ployed or have had time lapse since their last deployment.
Conclusions
Our sample size for this study was limited because of
the current restrictive policies of all branches that set Current military EM clinical practice environments do not
forth requirements for surveying active duty personnel. provide adequate volume to meet the perceived volume
Maintaining EM Procedural Skills in Garrison Settings 69