Page 60 - ATP-P 11th Ed
P. 60
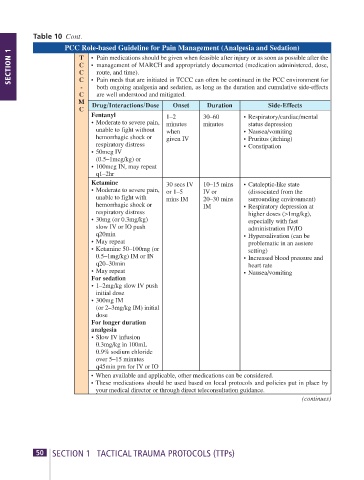
Table 10 Cont.
PCC Role-based Guideline for Pain Management (Analgesia and Sedation)
SECTION 1 T • Pain medications should be given when feasible after injury or as soon as possible after the
C • management of MARCH and appropriately documented (medication administered, dose,
C
route, and time).
C
- • Pain meds that are initiated in TCCC can often be continued in the PCC environment for
both ongoing analgesia and sedation, as long as the duration and cumulative side-effects
C are well understood and mitigated.
M Drug/Interactions/Dose Onset Duration Side-Effects
C
Fentanyl 1–2 30–60 • Respiratory/cardiac/mental
• Moderate to severe pain, minutes minutes status depression
unable to fight without when • Nausea/vomiting
hemorrhagic shock or given IV • Pruritus (itching)
respiratory distress • Constipation
• 50mcg IV
(0.5–1mcg/kg) or
• 100mcg IN, may repeat
q1–2hr
Ketamine 30 secs IV 10–15 mins • Cataleptic-like state
• Moderate to severe pain, or 1–5 IV or ( dissociated from the
unable to fight with mins IM 20–30 mins surrounding environment)
hemorrhagic shock or IM • Respiratory depression at
respiratory distress higher doses (>1mg/kg),
• 30mg (or 0.3mg/kg) especially with fast
slow IV or IO push administration IV/IO
q20min • Hypersalivation (can be
• May repeat problematic in an austere
• Ketamine 50–100mg (or setting)
0.5–1mg/kg) IM or IN • Increased blood pressure and
q20–30min heart rate
• May repeat • Nausea/vomiting
For sedation
• 1–2mg/kg slow IV push
initial dose
• 300mg IM
(or 2–3mg/kg IM) initial
dose
For longer duration
analgesia
• Slow IV infusion
0.3mg/kg in 100mL
0.9% sodium chloride
over 5–15 minutes
q45min prn for IV or IO
• When available and applicable, other medications can be considered.
• These medications should be used based on local protocols and policies put in place by
your medical director or through direct teleconsultation guidance.
(continues)
50 SECTION 1 TACTICAL TRAUMA PROTOCOLS (TTPs) ATP-P Handbook 11th Edition 51