Page 23 - JSOM Winter 2025
P. 23
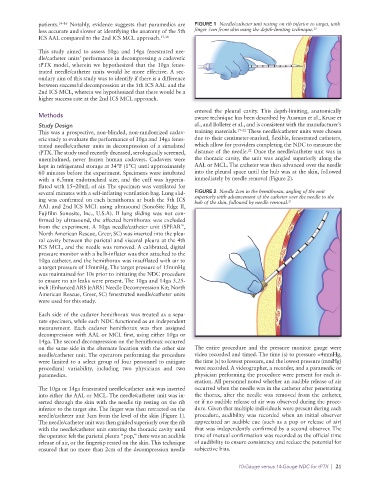
patients. 14–16 Notably, evidence suggests that paramedics are FIGURE 1 Needle/catheter unit resting on rib inferior to target, with
less accurate and slower at identifying the anatomy of the 5th finger 3cm from skin using the depth-limiting technique. 23
ICS AAL compared to the 2nd ICS MCL approach. 17,18
This study aimed to assess 10ga and 14ga fenestrated nee-
dle/catheter units’ performance in decompressing a cadaveric
tPTX model, wherein we hypothesized that the 10ga fenes-
trated needle/catheter units would be more effective. A sec-
ondary aim of this study was to identify if there is a difference
between successful decompression at the 5th ICS AAL and the
2nd ICS MCL, wherein we hypothesized that there would be a
higher success rate at the 2nd ICS MCL approach.
entered the pleural cavity. This depth-limiting, anatomically
Methods aware technique has been described by Ausman et al., Kruse et
Study Design al., and Bolleter et al., and is consistent with the manufacturer’s
This was a prospective, non-blinded, non-randomized cadav- training materials. 19–22 These needle/catheter units were chosen
eric study to evaluate the performance of 10ga and 14ga fenes- due to their centimeter-marked, flexible, fenestrated catheters,
trated needle/catheter units in decompression of a simulated which allow for providers completing the NDC to measure the
22
tPTX. The study used recently deceased, serologically screened, distance of the needle. Once the needle/catheter unit was in
unembalmed, never frozen human cadavers. Cadavers were the thoracic cavity, the unit was angled superiorly along the
kept in refrigerated storage at 34°F (1°C) until approximately AAL or MCL. The catheter was then advanced over the needle
60 minutes before the experiment. Specimens were intubated into the pleural space until the hub was at the skin, followed
with a 6.5mm endotracheal size, and the cuff was hyperin- immediately by needle removal (Figure 2).
flated with 15–20mL of air. The specimen was ventilated for
several minutes with a self-inflating ventilation bag. Lung slid- FIGURE 2 Needle 2cm in the hemithorax, angling of the unit
ing was confirmed on each hemithorax at both the 5th ICS superiorly with advancement of the catheter over the needle to the
hub of the skin, followed by needle removal.
23
AAL and 2nd ICS MCL using ultrasound (SonoSite Edge II,
Fujifilm Sonosite, Inc., U.S.A). If lung sliding was not con-
firmed by ultrasound, the affected hemithorax was excluded
from the experiment. A 10ga needle/catheter unit (SPEAR ,
™
North American Rescue, Greer, SC) was inserted into the pleu-
ral cavity between the parietal and visceral pleura at the 4th
ICS MCL, and the needle was removed. A calibrated, digital
pressure monitor with a bulb-inflater was then attached to the
10ga catheter, and the hemithorax was insufflated with air to
a target pressure of 15mmHg. The target pressure of 15mmHg
was maintained for 10s prior to initiating the NDC procedure
to ensure no air leaks were present. The 10ga and 14ga 3.25-
inch (Enhanced ARS [eARS] Needle Decompression Kit; North
American Rescue, Greer, SC) fenestrated needle/ catheter units
were used for this study.
Each side of the cadaver hemithorax was treated as a sepa-
rate specimen, while each NDC functioned as an independent
measurement. Each cadaver hemithorax was then assigned
decompression with AAL or MCL first, using either 10ga or
14ga. The second decompression on the hemithorax occurred
on the same side in the alternate location with the other size The entire procedure and the pressure monitor gauge were
needle/catheter unit. The operators performing the procedure video recorded and timed. The time (s) to pressure <4mmHg,
were limited to a select group of four personnel to mitigate the time (s) to lowest pressure, and the lowest pressure (mmHg)
procedural variability, including two physicians and two were recorded. A videographer, a recorder, and a paramedic or
paramedics. physician performing the procedure were present for each it-
eration. All personnel noted whether an audible release of air
The 10ga or 14ga fenestrated needle/catheter unit was inserted occurred when the needle was in the catheter after penetrating
into either the AAL or MCL. The needle/catheter unit was in- the thorax, after the needle was removed from the catheter,
serted through the skin with the needle tip resting on the rib or if no audible release of air was observed during the proce-
inferior to the target site. The finger was then retracted on the dure. Given that multiple individuals were present during each
needle/catheter unit 3cm from the level of the skin (Figure 1). procedure, audibility was recorded when an initial observer
The needle/catheter unit was then guided superiorly over the rib appreciated an audible cue (such as a pop or release of air)
with the needle/catheter unit entering the thoracic cavity until that was independently confirmed by a second observer. The
the operator felt the parietal pleura “pop,” there was an audible time of mutual confirmation was recorded as the official time
release of air, or the fingertip rested on the skin. This technique of audibility to ensure consistency and reduce the potential for
ensured that no more than 2cm of the decompression needle subjective bias.
10-Gauge versus 14-Gauge NDC for tPTX | 21